
Survey of Healthcare Providers Views and Experiences with Vaccine Hesitancy
Final Report
Contract number: 6ED034/164671/001/CY
POR Registration Number: POR # 118-16
Contract date: 2017-03-07
Report date: March 31, 2018
Fieldwork dates: November 21, 2017 - January 25, 2018
Prepared for:
Public Health Agency of Canada (PHAC)
Prepared by:
Environics Research Group
PA 9385
Ce rapport est aussi disponible en français sur demande
For more information on this report:
info@hc-sc.gc.ca
Table of Contents
The Public Health Agency of Canada (PHAC) identified the need for public opinion research to understand healthcare providers' (HCP) perspectives of, and experiences with, vaccine delay/refusal at a time when the number of Canadians who are delaying/refusing immunization is increasing. The research was needed to understand how HCPs communicate with patients about vaccination, how the rate of hesitancy is changing over time and what tools and resources HCPs are aware of/utilize.
Specifically, the aims of the research are to:
To address the research objectives, an online survey was conducted with 2,004 healthcare providers who provide vaccines or advice on vaccines. Five separate groups of healthcare providers were surveyed between November 21, 2017 - January 25, 2018:
The cost of this research was $138,312.00 (HST included).
The following presents the key findings of the research, first in terms of the overall themes, followed by a brief summary of each individual healthcare profession.
With these broad findings in mind, the following paragraphs highlight unique aspects of the experiences and opinions of each HCP type.
Family physicians have the broadest scope in terms of the patients they see and the vaccines they provide; they are the most likely to be providing vaccines and/or advice at least a few times a week (78%). While half say that patient vaccine hesitancy is unchanged from five years ago, the remainder are twice as likely to say this behaviour has increased (33%) than decreased (17%). Notably, they are not as likely as nurses, pharmacists and specialists to feel they have adequate access to information resources to help them address patient vaccine concerns. Family physicians are also least likely to use social media to learn and/or share information about health issues including vaccination.
Like family physicians, nurses see a diverse group of patients and are almost as frequently engaged in providing vaccines and/or advice. Their experiences with patient vaccine hesitancy and their own personal beliefs about vaccine safety and efficacy also generally mirror those of family physicians. Where nurses stand out is in their greater use of both printed and digital informational materials, including being by far the most likely to send home printed materials about vaccination with patients. They are most likely to know about PHAC resources and to make use of them, to subscribe to CIG email updates and to be familiar with the CANImmunize app. Finally, they are more likely than others to say they have adequate resources for patients where there is a language barrier (although only 36% say they do).
As a group, pharmacists report a more limited scope for administering vaccines (mostly adults, seniors, and to a lesser extent, children), have been doing so for less time than most other HCPs and do it less frequently (and in Quebec, pharmacists are not allowed to vaccinate). Perhaps for this reason, relatively few (27%) feel very prepared to handle patient concerns (although this is on par with family physicians). Pharmacists have a positive view of vaccine safety, efficacy and regulation, but are less likely than other HCP types to strongly disagree with negative statements about vaccines (e.g., that administering multiple vaccines at a single visit could reduce their efficacy or overwhelm the immune system). They are not, however, any more reluctant to recommend vaccines. Pharmacists are relatively more likely to use digital vaccine resources, especially online resources or web portals. Given their typical workspace, they are less likely to hang general health promotional posters in their office, clinic or waiting room or to give such materials to a patient.
For this study, specialists included obstetricians/gynaecologists and paediatricians. Thus, their practice with respect to vaccines is focused on pregnant women, infants and children. With the caveat that low numbers of specialists responded to the survey (n=78), they are the most likely to report that patient vaccine reluctance (55%, n=42) and mentions of incorrect vaccine information (52%, n=40) are happening more often than five years ago; substantial minorities also perceive more outright refusals and alternative schedule requests than before. Likely as a result, they are far more likely than others to see vaccine reluctance as a significant public health issue. At the same time, specialists are among the most likely to feel very prepared to address patient vaccine concerns (on par with nurses).
Midwives administer and/or provide advice on vaccines almost exclusively for pregnant women and infants, and the frequency with which they do this is the lowest of the HCP types. They are more likely to report experiencing patient vaccine hesitation in all its forms, including reluctance, refusal and requesting an alternative schedule. They are the most likely to report hearing patient concerns about the long-term effects of vaccines, specific ingredients (such as mercury) and to say their patients are reluctant about all infant vaccines (50%). It is possible that they may attract more vaccine hesitant patients (parents).
Midwives are consistently less likely to hold positive views about vaccines (and most likely to say they are not sure about safety, efficacy etc). They are also most likely to have concerns about administering multiple vaccines at a single visit and to be themselves reluctant to recommend at least one vaccine (most often citing the adult HPV or infant varicella vaccines). Midwives are the least likely of all HCPs to say they are 'very prepared' to address patient vaccine concerns. They are also the least likely to feel they have adequate information resources to help them address patient concerns about vaccines.
I hereby certify as a Senior Officer of Environics Research that the deliverables fully comply with the Government of Canada political neutrality requirements outlined in the Communications Policy of the Government of Canada and Procedures for Planning and Contracting Public Opinion Research. Specifically, the deliverables do not contain any reference to electoral voting intentions, political party preferences, standings with the electorate, or ratings of the performance of a political party or its leader.
Sarah Roberton
Vice President, Corporate and Public Affairs
sarah.roberton@environics.ca
613.699.6884
Supplier name: Environics Research Group
PWGSC contract number: 6ED034/164671/001/CY
POR Registration Number: POR # 118-16
Original contract date: 2017-03-07
For more information, contact info@hc-sc.gc.ca
The benefits of immunization are well-established, and although these benefits have been promoted by governments, public healthcare organizations and healthcare representatives for a long time now, some Canadians delay or refuse to get immunized. Recent research even suggests that the number of Canadians who are delaying or refusing immunization is increasing.
Healthcare providers are an important agent in the uptake of immunization. As authorities on an important personal issue, they are also opinion leaders. Evidence from the 2013 Childhood National Immunization Coverage Survey (cNICS) indicates that HCPs are the most trusted source of immunization information for Canadians.
Budget 2016 committed $25 million over five years ($5M annually), starting in 2016-17, to PHAC to increase immunization coverage rates. This survey of HCPs will facilitate evaluation of key PHAC published resources (i.e.: National Advisory Committee on Immunization statements, the Canadian Immunization Guide) and their role in building capacity in HCPs to address vaccine hesitancy. The survey of HCPs will also inform the direction of the Centre for Immunization and Respiratory Infectious Diseases (CIRID) programs by providing relevant information on the views/needs of HCPs in addressing concerns of their vaccine hesitant patients, and on immunization more generally. The Agency will use the survey results to advise program activity and to establish a baseline for measuring program effectiveness through a future survey.
PHAC identified a need to build on existing research to better understand healthcare providers' perspectives of, and experiences with, vaccine delay/refusal. This research will help PHAC to answer questions, such as: how do HCPs communicate with their patients about immunization? Do HCPs see hesitancy among patients increasing or decreasing? What resources, tools, and tactics are HCPs using to address vaccine hesitancy? Are HCPs aware of all of the tools and resources available to them? What tools or resources do HCPs find effective? Do HCP's know about or use PHAC resources and tools? This research will also facilitate evaluation of key PHAC published resources and their role in building capacity in HCPs to address vaccine hesitancy.
The research supports commitments announced in Budget 2016 to update the national immunization coverage goals & disease reduction targets, improve Canada's ability to identify under- and un-immunized Canadians and develop a focused program to improve vaccine access/uptake. It also helps PHAC improve immunization initiatives and the resources that HCPs use. In particular, the research findings will be used to help PHAC develop and disseminate resources for HCPs and Canadians to help them make an informed decision about immunization. Survey questions on HCPs' experience of vaccine hesitancy, knowledge, attitudes and beliefs will help the Agency understand and answer the questions and concerns that Canadians and healthcare providers have about immunization. Overall, this research will help direct program activities designed to increase immunization uptake in Canada.
More specifically, the aims of the research are to:
The results of this research will be used to:
The results of this research are based on an online survey conducted with a total of 2,004 healthcare providers who administer and/or provide advice about vaccines to patients. Five separate types of healthcare providers were surveyed between November 21, 2017 and January 25, 2018:
Survey respondents for all HCP types except midwives were gathered using a proprietary, 'opt-in' panel. Because the samples used in online panel surveys are based on self-selection and not a probability sample, no formal estimates of sampling error can be calculated.
The sample was designed to achieve completed surveys with 2,000 Canadian HCPs. Survey respondents were screened to ensure that they administer and/or provide advice about vaccines to patients. The eligibility rate among HCPs who started the survey is 80 percent or more for each HCP type; the table below summarizes the eligibility rate.
| Health Care Provider Group | Started Survey | Do not administer/provide advice about vaccines | Administer/provide advice about vaccines | ||
| Proportion | Count | Proportion | Count | ||
| Family Physicians | 549 | 3% | 14 | 97% | 535 |
| Midwives | 345 | 14% | 48 | 86% | 297 |
| Nurses | 588 | 16% | 95 | 84% | 493 |
| Pharmacists | 755 | 20% | 154 | 80% | 601 |
| Specialists (obstetricians/gynecologists and paediatricians) | 89 | 12% | 11 | 88% | 78 |
| Total | 2,326 | 14% | 322 | 86% | 2,004 |
A random sample of family physicians, nurses, specialists and pharmacists were invited to participate through the mdBriefCase online panel of healthcare providers. Quotas were set by region within each health profession to ensure the final sample is representative of the distribution of HCPs across the country.
The sample of midwives is based on the mailing list of the Canadian Association of Midwives (CAM). No regional or other quotas were set for this target audience.
The table below summarizes the actual number of completed surveys by region within each health profession. In most cases, the regional distribution of respondents in each profession closely matches population statistics drawn from the 2016 CIHI Health Workforce Survey and the CAM website. As a result, minimal weighting factors were used to ensure the data matched the population distribution. Since no population estimates exist for HCPs who provide vaccines or vaccine advice, the weighting targets are based upon the overall universe of HCP types (regardless of whether they provide vaccines/advice).
The only segment that was not weighted is pharmacists in Quebec since they do not currently provide vaccines. Instead, their unweighted distribution in the data was maintained (four percent) and the remaining regions were redistributed proportionately to the number of pharmacists outside of Quebec.
Region (Unweighted) |
Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Atlantic | 38 | 6 | 34 | 27 | 3 |
| Quebec | 35 | 24 | 113 | 22 | 16 |
| Ontario | 325 | 175 | 207 | 406 | 41 |
| Manitoba/Saskatchewan | 38 | 11 | 47 | 38 | 4 |
| Alberta | 45 | 21 | 47 | 51 | 7 |
| BC/Territories | 54 | 60 | 45 | 57 | 7 |
| Region (Weighted) |
Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Atlantic | 38 | 2 | 43 | 57 | 5 |
| Quebec | 124 | 38 | 118 | 22 | 18 |
| Ontario | 194 | 157 | 170 | 274 | 30 |
| Manitoba/Saskatchewan | 33 | 17 | 39 | 57 | 5 |
| Alberta | 67 | 21 | 61 | 94 | 11 |
| BC/Territories | 79 | 62 | 62 | 97 | 9 |
PHAC developed a draft questionnaire, which was revised and finalized based on recommendations from Environics. It was designed to meet all of the research objectives set out for this project and adhere to Federal Government standards for public opinion research. The final study questionnaire is included as Appendix B.
Prior to finalizing the survey for field, a pre-test (soft launch) was conducted in English and French on November 21, 2017 with a total of 43 respondents. The pre-test assessed the questionnaire in terms of question wording and sequencing, respondent sensitivity to specific questions and to the survey overall and to determine the survey length; standard Government of Canada pre-testing questions were also asked. Following the pre-test, three questions were removed to reduce the questionnaire length. Since there were no other substantive changes, all of the pre-test interviews were kept as part of the final sample.
The survey was programmed by Environics in a secure, fully featured web-based survey environment. To maintain respondent confidentiality, invitations to the survey were managed by mdBriefCase (including a unique URL survey link for each respondent) and the Canadian Association of Midwives (including an open link that was valid for all midwives). Data collection for the mdBriefCase sample took place between November 21, 2017 and January 25, 2018, and for the CAM sample between December 15, 2017 and January 25, 2018. All respondents to the survey were paid a $25 incentive for their participation. The average length of time to complete the survey was 21 minutes.
All respondents were offered the opportunity to complete the surveys in their official language of choice. All research work was conducted in accordance with the Standards for the Conduct of Government of Canada Public Opinion Research - Online Surveys and the standards set by the Marketing Research and Intelligence Association (MRIA), as well as applicable federal legislation (Personal Information Protection and Electronic Documents Act, or PIPEDA). Both the research design and the questionnaire were also submitted for review to the Health Canada/PHAC Research Ethics Board (REB). The survey was registered with the MRIA's research registra-tion system, which permits the public to verify the legitimacy of a survey, inform themselves about the industry and/or register a complaint.
A total of 31,063 survey invitations were sent to health care professionals. Overall, 2,326 responded to this email invitation and clicked on the survey link, resulting in a seven percent contact rate. Respondents who do not administer vaccines or provide advice are removed in the calculation of the overall participation rate, which was 6%. The contact rate was highest for midwives; it ranged from 3-8% for the HCP types sourced from the mdBriefCase panel.
| # of respondents | Family Physicians | Nurses | Pharmacists | Specialists (obstetricians/ gynecologists & paediatricians) | mdBriefCase (Total) | Midwives | Total |
| (A) Sent an email invite | 9,007 | 6,954 | 10,580 | 2,302 | 29,563 Footnote * | 1,500 | 31,063 Footnote * |
| (B) Started Survey | 549 | 588 | 755 | 89 | 1,981 | 345 | 2,326 |
| (C) Contact Rate (B / A) | 6% | 8% | 7% | 4% | 7% | 23% | 7% |
| (D) Not qualified | 14 | 95 | 154 | 11 | 274 | 48 | 322 |
| (E) Completed Survey | 535 | 493 | 601 | 78 | 1,707 | 297 | 2,004 |
| (F) Participation Rate (E / A) | 6% | 7% | 6% | 3% | 6% | 20% | 6% |
Some respondents within the mdBriefCase panel had profession information that could not be classified or was unknown. These cases (720 in total) have been included in the total invites number but not within each profession type. Although the proportion of respondents without profession information is very small (2%), the contact/participation rates for each profession (outside of midwives) may be slightly lower than reported here.
Two rounds of reminder emails were sent throughout the fieldwork period to attempt to reach those who had been sent an initial invite but had not yet completed the survey. This was done to maximize the contact rate and minimize the effects of nonresponse bias.
The mdBriefCase panel contains more than 100,000 HCPs and includes a significant proportion of the total population of each healthcare profession within Canada. In most cases, the panel also appears to be regionally representative of each healthcare profession.
We believe that this research provides a broad and solid understanding of the attitudes and opinions of HCPs. However, there are some limitations that should be taken into consideration when interpreting the results.
Provided under a separate cover is a detailed set of "banner tables" presenting the results for all questions by HCP type (profession). These tables are referenced by the survey question given underneath each table or graph. A detailed description of the methodology used to conduct this research is presented in Appendix A.
Sample sizes are provided for every question in the report, including where a subset of all respondents was asked to provide a response. A description of what proportion of the entire data set is represented in the data displayed is given below each table/graph.
In this report, results are expressed as percentages unless otherwise noted. Results may not add to 100% due to rounding or multiple responses. Net results cited in the text may not exactly match individual results shown in the charts due to rounding. In cases where fewer than 20 responses are provided for a given question within a HCP group, the results are suppressed to protect anonymity.
A majority of family physicians and specialists report administering or providing advice about vaccines for more than 15 years. Three quarters of nurses say they have done so for at least six years, while three-quarters of midwives have done so for between one and 15 years. Reflecting relatively recent changes in professional duties, the majority of pharmacists have been doing so for five years or less (in most provinces, pharmacists only began vaccinating less than 10 years ago and in Quebec they are not currently allowed).
| Length of time | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Less than 1 year | 1% | 6% | 4% | 5% | 2% |
| 1 to 5 years | 18% | 39% | 21% | 60% | 14% |
| 6 to 15 years | 24% | 37% | 40% | 22% | 25% |
| More than 15 years | 57% | 18% | 35% | 13% | 59% |
Q2. For approximately how many years have you been administering vaccines or providing advice to your patients on vaccines? Base: All respondents
There are also distinctions in how often HCP respondents administer or provide vaccine advice. Approximately three in ten family physicians, nurses and specialists do so on a daily basis, with majorities doing so at least a few times a week. Midwives and pharmacists administer or provide vaccine advice less often, with majorities in each profession who say they do so once a week or less often.
| Frequency | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Daily | 33% | 1% | 28% | 15% | 30% |
| A few times a week | 45% | 25% | 35% | 32% | 28% |
| About once a week | 12% | 35% | 11% | 20% | 21% |
| Less often than once a week | 10% | 40% | 25% | 33% | 22% |
Q3. How often do you administer vaccines or provide advice about vaccines? Base: All respondents
A majority of family physicians report providing vaccines/advice to patients of every type, although most commonly adults and seniors. Similarly, a majority of nurses say the same, albeit with fewer providing vaccines/advice to each type of patient than do family physicians. Specialists (which include obstetricians/gynecologists and paediatricians) are more likely to provide vaccines/advice to infants and children than to other patient types, while midwives are most likely to do this for pregnant women and infants. Pharmacists tend to provide vaccines/advice mostly to adults and seniors.
| Patient types | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Infants/young children (0-6yrs) | 75% | 81% | 57% | 14% | 72% |
| Children (7-17yrs) | 78% | 1% | 62% | 60% | 66% |
| Adults (18-64yrs) | 92% | 28% | 90% | 95% | 37% |
| Seniors (65yrs+) | 94% | 1% | 79% | 90% | 11% |
| Pregnant women | 61% | 86% | 51% | 45% | 25% |
| Other | 9% | 2% | 9% | 4% | 3% |
Q4. To whom do you administer vaccines and/or provide advice on vaccines? Base: All respondents
HCP respondents report that it is relatively common for patients to express reluctance about vaccines some of the time (ranging between 62% and 73% by HCP type) or more often. Having a patient refuse a vaccine or request an alternative schedule happens less commonly, with a majority of HCP respondents reporting that this occurs 'rarely' or 'never.' An exception is midwives, who are more likely to say their patients refuse a vaccine or request an alternative schedule 'some of the time' than do other HCPs.
| Frequency | Express Reluctance | Refuse a Vaccine | Request an Alternative Schedule | |
| Family Physicians (n=535) | Every/Most of the time | 9% | 2% | 3% |
| Some of the time | 62% | 36% | 34% | |
| Rarely/Never | 29% | 62% | 63% | |
| Midwives (n=297) |
Every/Most of the time | 19% | 2% | 10% |
| Some of the time | 70% | 54% | 68% | |
| Rarely/Never | 11% | 44% | 22% | |
| Nurses (n=493) |
Every/Most of the time | 6% | 1% | 2% |
| Some of the time | 63% | 39% | 33% | |
| Rarely/Never | 30% | 60% | 65% | |
| Pharmacists (n=601) |
Every/Most of the time | 6% | 3% | 3% |
| Some of the time | 66% | 41% | 30% | |
| Rarely/Never | 28% | 57% | 67% | |
| Specialists (n=78) |
Every/Most of the time | 5% | 0% | 1% |
| Some of the time | 73% | 20% | 34% | |
| Rarely/Never | 23% | 80% | 64% |
Q5. When you recommend a vaccine or vaccines to patients, how often do they…? Base: All respondents
HCP respondents have mixed views about the change in frequency of vaccine reluctance, refusal and alternative schedule requests over the past five years. In general, HCPs are most likely to say that the frequency of these behaviours has not changed; the remainder are divided about whether they are encountering these behaviours more or less often. Small numbers of Specialists are more likely than others to say that reluctance, refusal and alternative schedule requests are happening more often; otherwise, there is no clear pattern in the results.
| Sample size | Frequency | Express Reluctance | Refuse a Vaccine | Request an Alternative Schedule | |
| Family Physicians | (425) | More often | 33% | 26% | 14% |
| About the same | 49% | 53% | 58% | ||
| Less often | 17% | 20% | 18% | ||
| Midwives | (163) | More often | 20% | 12% | 21% |
| About the same | 58% | 54% | 51% | ||
| Less often | 23% | 29% | 21% | ||
| Nurses | (365) | More often | 29% | 21% | 17% |
| About the same | 53% | 52% | 48% | ||
| Less often | 18% | 24% | 24% | ||
| Pharmacists | (195) | More often | 24% | 14% | 5% |
| About the same | 38% | 49% | 56% | ||
| Less often | 36% | 29% | 19% | ||
| Specialists | (66) | More often | 55% | 42% | 32% |
| About the same | 37% | 38% | 42% | ||
| Less often | 9% | 20% | 10% |
Q6A-C. Compared to five years ago, do you find the following has been happening more often, less often, or with about the same frequency? Base: Respondents with more than five years experience administering/providing advice about vaccines. Note: The 'Not Sure' category has been removed for clarity (results range from 0-3% for reluctance / 0-8% for refusal / 7-21% for alternative schedules).
There is also no clear consensus among HCP respondents about how often patients express strong support for vaccines compared to five years ago. Roughly half of each HCP type feels it is happening with the same frequency as before; the balance of pharmacists, nurses and midwives feel it is happening more often, while the balance of family physicians and specialists say it is happening less often.
Majorities of each HCP (with the exception of pharmacists) say that the extent to which patients seem knowledgeable about vaccines is about the same as five years ago, and most of the remainder in each case (and particularly for pharmacists) find it has been happening more often.
When asked how often patients are mentioning incorrect information compared to five years ago, it is most common for HCP respondents to say it is happening with the same frequency. Of the remainder, family physicians, nurses and specialists tend to say it is happening more often than less. It is worth noting that responses to this question are dependent on the beliefs of the HCP respondent themselves; their perception of 'incorrect information' may differ from that of the larger healthcare community.
|
Q6D-F. Compared to five years ago, do you find the following has been happening more often, less often, or with about the same frequency? Base: Respondents with more than five years experience administering/providing advice about vaccines.
Note: The 'Not Sure' category has been removed for clarity (results range from 2-6% for expressing strong support / 1-7% for seeming knowledgeable / 3-10% for mentioning incorrect information).
HCP respondents were shown a list of possible reasons why patients may not want themselves or their family members vaccinated, and asked which, if any, they have heard in the last year. In interpreting this data, it is important to consider the role of confirmation bias (both the possibility that a patient's/parent's beliefs may be a reflection of, or influenced by, the HCP respondent's beliefs or that HCPs will better recall parental concerns consistent with their own beliefs).
The top parental concerns reported by all HCP types are those related to vaccine safety, and particularly:
Significant proportions of each HCP type have also heard reasons related to under-estimating the threat of disease, lack of trust in institutions, and belief in alternative therapies. A small number of HCPs wrote in patient concerns about a specific connection to autism (as an 'other' mention); however, other HCPs may have chosen to categorize these concerns as 'heard of adverse reaction' or 'worried about possible long-term effects.' Thus, no conclusions about the extent of autism concerns can be drawn from these findings.
Midwives and specialists (who are among the most likely to administer/provide advice about infant vaccines) are more likely than others to hear patients say it is better to wait until the child is older or that too many injections are being given at one time. (This is an example of where a HCP's own set of beliefs may influence parental concerns and/or factor into how the HCP responds to this question).
Relative to other HCP types, pharmacists are more likely to hear about logistical concerns and accessibility, such as difficulties getting to the clinic and getting time off work.
| Reasons selected | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Concerns about vaccine safety | |||||
| Know or heard of someone who had an adverse reaction to a vaccine | 67% | 59% | 62% | 62% | 70% |
| Worried about specific ingredients in vaccines (e.g., mercury, thimerosal) | 62% | 84% | 61% | 54% | 69% |
| Worried about possible long-term effects | 57% | 75% | 51% | 39% | 69% |
| Worried that the vaccine will actually cause the illness it is meant to prevent | 53% | 30% | 58% | 58% | 42% |
| Think there are too many injections being given at one time | 44% | 66% | 47% | 17% | 63% |
| Worried about immediate side effects (i.e. adverse events following immunization) | 44% | 42% | 42% | 41% | 61% |
| Fear of needles/Find needles too painful | 41% | 18% | 42% | 49% | 42% |
| Think it is better to wait until child is older | 39% | 69% | 33% | 9% | 59% |
| Think there are too many antigens in vaccines | 22% | 27% | 21% | 10% | 43% |
| Under-estimating threat of disease | |||||
| Believe that the disease is not a big concern ("I had it when I was a kid and I'm OK") | 55% | 45% | 52% | 50% | 62% |
| Believe the vaccine is not needed anymore (as the disease is gone or almost gone) | 37% | 28% | 40% | 31% | 49% |
| Lack of trust in institutions | |||||
| Conspiracy theories (pharmaceutical companies and/or government) | 51% | 58% | 55% | 50% | 64% |
| Distrust of healthcare professionals | 21% | 29% | 11% | 12% | 31% |
| Beliefs in alternatives to vaccines | |||||
| Believe natural immunity is enough | 49% | 46% | 43% | 42% | 60% |
| Believe alternate therapies are a better choice (e.g., homeopathy) | 35% | 45% | 34% | 23% | 45% |
| Believe if other children are vaccinated their own children do not need to be | 22% | 20% | 24% | 15% | 25% |
| Concerns about vaccine effectiveness | |||||
| Concerned vaccines don't protect against the disease | 41% | 34% | 41% | 49% | 39% |
| Other (shown on screen) | |||||
| Find it difficult to get the vaccine (e.g. time off work, transportation to clinic, too busy) | 15% | 5% | 19% | 23% | 19% |
| Religious beliefs do not allow for/discourage vaccination | 11% | 13% | 12% | 8% | 16% |
| Other mentions (written in) | |||||
| Connection to autism | 2% | 2% | 2% | 1% | 7% |
| Financial concerns / costs | 2% | 1% | 1% | 2% | 0% |
| Weakened immune system | 1% | 1% | 1% | 0% | 0% |
| Other | 2% | 7% | 2% | 1% | 3% |
| None | 2% | 1% | 2% | 1% | 0% |
Q7. In the last year, what reason(s), if any, have patients provided as to why they do not want themselves or their family members vaccinated? Base: All respondents
HCP respondents who provide vaccines/advice for each of type of patient were asked which vaccines (if any) patients were reluctant to receive.
Infant vaccines. Family physicians, specialists and nurses were most likely to identify MMR, MMRV, varicella and rotavirus as the infant vaccines about which patients express reluctance. Substantial minorities of family physicians and specialists mentioned that patients were reluctant about all infant vaccines.
Half of all midwives involved in infant vaccines mentioned their patients were reluctant about all infant vaccines; varicella and the MMR vaccines were the two most commonly mentioned by name. A relatively small proportion of pharmacists provide vaccines/advice to infants and among this group, a wide variety of vaccines were mentioned but at relatively low levels.
| Infant vaccines | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample size | (442) | (242) | (282) | (92) | (58) |
| Measles, Mumps, Rubella (MMR) | 36% | 14% | 34% | 10% | 41% |
| Measles, Mumps, Rubella, Varicella (MMRV) | 25% | 8% | 26% | 5% | 35% |
| Varicella (chickenpox) | 25% | 21% | 39% | 13% | 34% |
| Rotavirus | 14% | 7% | 26% | 2% | 24% |
| Diphtheria, tetanus, pertussis, polio, haemophilus influenzae type B (DTaP-IPV-Hib) | 8% | 9% | 8% | 7% | 20% |
| Pneumococcal | 6% | 3% | 8% | 8% | 10% |
| Diphtheria, tetanus, pertussis, hepatitis B, polio, haemophilus influenzae type (DTaP-HB-IPV-Hib) | 5% | 8% | 7% | 5% | 15% |
| Hepatitis A & B (HAHB) | 3% | 1% | 2% | 5% | 3% |
| Meningococcal | 3% | 4% | 6% | 5% | 14% |
| Hepatitis A (HA) | 2% | 1% | 4% | 4% | 3% |
| Hepatitis B (HB) | 2% | 6% | 8% | 3% | 7% |
| All infant vaccines | 26% | 50% | 17% | 16% | 33% |
| None/no patients identified specific vaccines they are reluctant to receive | 5% | 8% | 6% | 13% | 7% |
| Not sure/Not applicable | 3% | 8% | 3% | 8% | 0% |
Q8. In the last year, which of the following specific vaccines, if any, did patients say that they are reluctant to receive (for themselves or for their family members)? Base: HCPs who administer/provide advice on infant vaccines.
Child/adolescent vaccines. Across all HCP types, the HPV vaccine is the children/adolescent vaccine that patients seem most reluctant about. The MMR, MMVR and varicella vaccines are also among the more common causes of reluctance. Midwives do not commonly provide vaccines/advice to this group and thus the base size is too small to report their experiences.
| Children and adolescent vaccines | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample size | (448) | (BTS) | (308) | (363) | (56) |
| Human papillomavirus (HPV) | 52% | 66% | 35% | 60% | |
| Measles, Mumps, Rubella (MMR) | 21% | 20% | 8% | 27% | |
| Measles, Mumps, Rubella, Varicella, (MMRV) | 17% | 14% | 5% | 22% | |
| Varicella (chickenpox) | 17% | 25% | 12% | 21% | |
| Tetanus, diphtheria, pertussis (Tdap) | 6% | 5% | 5% | 11% | |
| Meningococcal | 6% | 8% | 6% | 11% | |
| Diphtheria, tetanus, pertussis, polio (DTaP-IPV) / Tetanus, diphtheria, pertussis, polio (Tdap-IPV) | 4% | 5% | 3% | 10% | |
| Hepatitis B (HB) | 3% | 7% | 5% | 8% | |
| Hepatitis A (HA) | 2% | 3% | 6% | 2% | |
| Hepatitis A & B (HAHB) | 2% | 5% | 9% | 5% | |
| All children's/adolescent vaccines | 13% | 9% | 5% | 11% | |
| None/no patients identified specific vaccines they are reluctant to receive | 6% | 7% | 13% | 4% | |
| Not sure/Not applicable | 3% | 2% | 8% | 0% |
Q8. In the last year, which of the following specific vaccines, if any, did patients say that they are reluctant to receive (for themselves or for their family members)? Base: HCPs who administer/provide advice on children/adolescent vaccines.BTS indicates base size too small to report
Adult vaccines. The top adult vaccines about which HCP respondents consistently hear reluctance include herpes zoster (shingles), HPV and pneumococcal vaccines. The exception is midwives, who hear concerns primarily about HPV and Tdap (a new NACI recommendation for pregnancy) vaccines.
| Adult vaccines | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample size | (527) | (278) | (476) | (597) | (33) |
| Herpes zoster (shingles) | 42% | 5% | 28% | 48% | 29% |
| Human papillomavirus (HPV) | 42% | 20% | 29% | 26% | 46% |
| Pneumococcal | 28% | 2% | 23% | 25% | 13% |
| Tetanus, diphtheria, pertussis (Tdap) | 11% | 17% | 15% | 6% | 18% |
| Tetanus, diphtheria (Td) | 10% | 1% | 11% | 5% | 2% |
| Hepatitis A & B (HAHB) | 8% | 1% | 8% | 13% | 7% |
| Meningococcal | 6% | 2% | 6% | 8% | 10% |
| Hepatitis A (HA) | 5% | 1% | 4% | 6% | 0% |
| Hepatitis B (HB) | 5% | 3% | 8% | 6% | 0% |
| All adult vaccines | 6% | 9% | 8% | 3% | 6% |
| None/no patients identified specific vaccines they are reluctant to receive | 7% | 11% | 10% | 17% | 7% |
| Not sure/Not applicable | 4% | 13% | 4% | 10% | 6% |
Q8. In the last year, which of the following specific vaccines, if any, did patients say that they are reluctant to receive (for themselves or for their family members)? Base: HCPs who administer/provide advice on adult vaccines.
The large majority of HCP respondents believe that patient reluctance/concern about vaccines is at least somewhat of an issue facing public health; few say it is not a very big issue or not an issue at all. Specialists are the most likely to see this as a significant public health issue (53%) while among other types of HCPs, this proportion ranges between 36-38%.

| Profession | A significant issue | Somewhat of an issue | Not a very big issue | Not an issue at all | Not sure |
| Family Physicians (n=535) | 36% | 47% | 16% | 1% | 1% |
| Midwives (n=297) | 38% | 42% | 15% | 2% | 3% |
| Nurses (n=493) | 37% | 50% | 12% | 1% | 0% |
| Pharmacists (n=601) | 36% | 51% | 11% | 0% | 1% |
| Specialists (n=78) | 53% | 38% | 9% | 0% | 0% |
Q37. Overall, to what extent do you think patient reluctance/concern about vaccination is an issue facing public health today? Base: All respondents
The large majority of HCP respondents of all types say they are at least somewhat prepared with the knowledge/skills necessary to address patient concerns about vaccines (ranging from 81 to 96 percent). Specialists (43%) and nurses (40%) are the most likely to say they are very prepared, while family physicians (28%), pharmacists (27%) and midwives (14%) are less so.
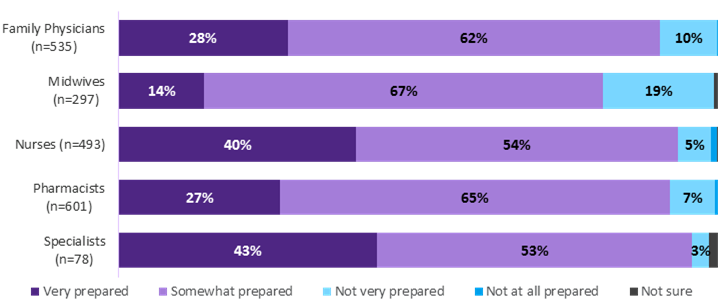
| Profession | Very prepared | Somewhat prepared | Not very prepared | Not at all prepared | Not sure |
| Family Physicians (n=535) | 28% | 62% | 10% | 0% | 0% |
| Midwives (n=297) | 14% | 67% | 19% | 0% | 1% |
| Nurses (n=493) | 40% | 54% | 5% | 1% | 0% |
| Pharmacists (n=601) | 27% | 65% | 7% | 1% | 0% |
| Specialists (n=78) | 43% | 53% | 3% | 0% | 1% |
Q9. In general, to what extent do you feel prepared with the knowledge and skills necessary to address patients who have concerns about vaccines? Base: All respondents
HCP respondents were asked their level of agreement with seven positively-worded statements about vaccination. A broad consensus emerges among family physicians, nurses, pharmacists and specialists that the vaccines in use in Canada are safe and effective, and that they trust the recommendations of the NACI and the regulatory system for vaccines in Canada. Large majorities also agree it is important to inform patients about all vaccines recommended for their age/condition (even if not publicly funded) and to give vaccines at the recommended times (according to the provincial or territorial schedule). Very few disagree with any of these statements (ranging from 1-5%, except for midwives).
Midwives are consistently less likely to strongly agree with these statements than the other HCP groups, and in turn, are more likely to either disagree or to say they are not sure about the statements. Despite this, midwives' overall agreement (strongly and somewhat agree combined) with all these statements outweighs disagreement.
| % Response | Family Physicians | Midwives | Nurses | Pharmacists | Specialists | |
| Sample Size | Response | (535) | (297) | (493) | (601) | (78) |
| Vaccines in use in Canada are safe | Strongly Agree | 80% | 54% | 82% | 82% | 84% |
| Agree (Net) | 99% | 89% | 99% | 98% | 96% | |
| Disagree (Net) | 1% | 5% | - | 1% | 2% | |
| Not sure | - | 6% | 1% | - | 2% | |
| I trust the recommendations of the National Advisory Committee on Immunization | Strongly Agree | 79% | 40% | 79% | 79% | 83% |
| Agree (Net) | 99% | 77% | 99% | 97% | 95% | |
| Disagree (Net) | 1% | 11% | 1% | 2% | 2% | |
| Not sure | 1% | 13% | 1% | 1% | 3% | |
| In general, vaccines in use in Canada are effective | Strongly Agree | 71% | 60% | 75% | 72% | 78% |
| Agree (Net) | 99% | 92% | 98% | 98% | 98% | |
| Disagree (Net) | 1% | 3% | 1% | 1% | 2% | |
| Not sure | - | 5% | 1% | - | - | |
| I trust that the vaccine regulatory system in Canada is safe and working effectively | Strongly Agree | 70% | 43% | 75% | 71% | 75% |
| Agree (Net) | 98% | 81% | 98% | 97% | 93% | |
| Disagree (Net) | 1% | 8% | 1% | 3% | 5% | |
| Not sure | 2% | 11% | 1% | 1% | 2% | |
| Vaccines are as safe as or safer than other prescription medications | Strongly Agree | 69% | 47% | 67% | 65% | 80% |
| Agree (Net) | 94% | 77% | 94% | 94% | 94% | |
| Disagree (Net) | 2% | 13% | 3% | 5% | 3% | |
| Not sure | 4% | 10% | 3% | 1% | 3% | |
| It is important to inform patients about all vaccines recommended for their age/condition, even if not publicly funded | Strongly Agree | 68% | 50% | 75% | 75% | 61% |
| Agree (Net) | 97% | 83% | 97% | 97% | 95% | |
| Disagree (Net) | 2% | 9% | 1% | 2% | 4% | |
| Not sure | 1% | 8% | 2% | 1% | 1% | |
| It is important to give vaccines at the recommended times (according to the provincial or territorial schedule) | Strongly Agree | 66% | 26% | 73% | 70% | 75% |
| Agree (Net) | 98% | 71% | 98% | 98% | 97% | |
| Disagree (Net) | 2% | 21% | 2% | 2% | 3% | |
| Not sure | - | 8% | - | - | - |
Q10. To what extent do you agree or disagree with the following statements… Base: All respondents
HCP respondents were also asked about their level of agreement with four negatively-worded statements. HCPs of every type strongly disagree with the notion that providing the HPV vaccine to adolescents could increase their likelihood of engaging in unprotected sexual activity.
Similarly, a majority strongly disagree that the practice of administering multiple vaccines at a single visit could overwhelm the immune system or reduce vaccine efficacy. The exception is midwives, who are less likely to strongly disagree with these two statements (due mainly to a larger proportion who say they are not sure).
In general, HCP respondents disagree overall (strongly and somewhat combined) with the idea that the pharmaceutical industry pushes certain vaccines for profit only (ranging from 56% to 62%). Midwives are again the exception (40% disagree overall, with a higher than average proportion who did not provide an opinion).
| % Response | Family Physicians | Midwives | Nurses | Pharmacists | Specialists | |
| Sample Size | Response | (535) | (297) | (493) | (601) | (78) |
| Administering the HPV vaccine to adolescents could increase their likelihood of engaging in unprotected sexual activity | Agree (net) | 6% | 8% | 7% | 13% | 8% |
| Strongly disagree | 73% | 72% | 76% | 62% | 68% | |
| Disagree (net) | 92% | 84% | 91% | 82% | 86% | |
| Not sure | 2% | 9% | 2% | 5% | 6% | |
| Administering multiple vaccines at a single visit could overwhelm the immune system | Agree (net) | 7% | 29% | 11% | 15% | 14% |
| Strongly disagree | 67% | 30% | 63% | 54% | 72% | |
| Disagree (net) | 88% | 51% | 84% | 80% | 78% | |
| Not sure | 5% | 21% | 5% | 5% | 7% | |
| Administering multiple vaccines at a single visit could reduce their efficacy | Agree (net) | 7% | 6% | 5% | 14% | 8% |
| Strongly disagree | 65% | 41% | 70% | 55% | 74% | |
| Disagree (net) | 88% | 59% | 88% | 82% | 84% | |
| Not sure | 5% | 35% | 6% | 4% | 8% | |
| The pharmaceutical industry pushes certain vaccines for profit only | Agree (net) | 33% | 36% | 27% | 33% | 26% |
| Strongly disagree | 23% | 20% | 31% | 27% | 30% | |
| Disagree (net) | 56% | 40% | 62% | 59% | 57% | |
| Not sure | 11% | 24% | 11% | 9% | 17% |
Q10. To what extent do you agree or disagree with the following statements… Base: All respondents
Just over one in ten family physicians, nurses, pharmacists and specialists said they, themselves, are reluctant to administer at least one vaccine. This proportion is higher among midwives at one in three (34%).
| Reluctance to recommend vaccines | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Yes, reluctant to recommend at least one vaccine | 14% | 34% | 13% | 13% | 12% |
| Not Reluctant to recommend ANY vaccines | 77% | 47% | 80% | 69% | 73% |
| Not sure/Not applicable | 9% | 18% | 7% | 18% | 15% |
Q11. Are there any vaccines you are reluctant to recommend? Base: All respondents
HCPs who indicated they were reluctant to recommend at least one vaccine were asked which vaccine(s) this applied to and the reasons for their reluctance. Due to small sample sizes, these results have been analyzed qualitatively. The data suggests that HCP respondents are most likely to be reluctant about herpes zoster (adults) citing the level of effectiveness and expense of Zostavax vaccine, while welcoming the new Shingrix vaccine. Varicella was also discussed given the perceived lack of severity of this disease and the lifelong immunity to chickenpox after having the disease. Rotavirus (infants) was mentioned given the expense and perceived lack of necessity in an industrialized country. HPV vaccines (adults and children/adolescents) continue to be discussed for a variety of reasons, and this is thought to be because the vaccine is relatively new.
Family physicians and nurses said they are very comfortable understanding and applying recommendations for vaccines among most patient types, including infants, children, adults, seniors and individuals with chronic diseases. Specialists are most comfortable with vaccine recommendations for infants and children, pharmacists with adults and seniors, and midwives with infants and pregnant women.
In most cases, the remainder of HCPs say they are somewhat comfortable (rather than uncomfortable) with this role. The exceptions are the substantial minority of midwives (ranging from 40% for adults to 66% for seniors) and pharmacists (from 34% for adults to 40% for seniors) who say they are unsure how comfortable they would be for specific patient types.
HCP respondents are least comfortable in vaccine recommendations for individuals who are immunocompromised. Nearly two-thirds of family physicians and nurses (64% each) say they would be at least somewhat comfortable in this situation, while half of pharmacists and specialists say the same. A majority of midwives (62%) are unsure how comfortable they would be advising this patient type.
| % Very comfortable | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Infants/young children (0-6yrs) | 66% | 47% | 54% | 13% | 73% |
| Children (7-17yrs) | 65% | 4% | 55% | 22% | 65% |
| Adults (18-64yrs) | 70% | 15% | 72% | 51% | 22% |
| Seniors (65+) | 70% | 3% | 65% | 54% | 15% |
| Pregnant women | 41% | 51% | 35% | 15% | 23% |
| Individuals with chronic diseases | 57% | 4% | 56% | 34% | 34% |
| Individuals who are immunocompromised | 26% | 1% | 25% | 11% | 18% |
Q14. How comfortable are you in understanding and applying recommendations for vaccination among the following groups? Base: All respondents
HCP respondents were asked what minimum information they need to recommend a new vaccine before guidance is issued by the National Advisory Committee on Immunization (NACI). There is no consensus among HCPs, but they are most likely to say they would prefer to wait for the NACI recommendations or for the vaccine to be listed in their provincial/territorial schedule before recommending it.
Some family physicians and pharmacists would rely on their own reading of the scientific literature or input from colleagues. Midwives, nurses and specialists are more likely to consult with colleagues over relying on their own reading of the literature.
| Minimum information needed | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Prefer to wait for recommendations from the NACI in the Canadian Immunization Guide | 41% | 27% | 36% | 46% | 33% |
| Prefer to wait until the vaccine is listed in my provincial/territorial immunization schedule or manual | 22% | 28% | 24% | 16% | 11% |
| Consult with colleagues, such as immunization experts or my local public health department | 19% | 24% | 26% | 14% | 36% |
| My own reading of the scientific literature and/or the product monograph | 14% | 5% | 9% | 20% | 12% |
| Other | 2% | 4% | 3% | 1% | 1% |
| Not sure | 2% | 12% | 2% | 3% | 6% |
Q27. When a new vaccine becomes available, but before there is guidance issued by the National Advisory Committee on Immunization in the Canadian Immunization Guide, what is the minimum information you need to recommend it? Base: All respondents
HCP respondents were asked about messages they had found to be particularly effective in helping vaccine hesitant patients become more comfortable with vaccinations. The messages fell into three broad categories: reinforcing the effectiveness of vaccines, addressing the concerns raised by patients and providing information.
Generally speaking, providing information, research and evidence about vaccines was the most common approach suggested by HCPs along with providing a risk vs. benefit analysis. Reinforcing the effectiveness and benefits of vaccines, both in general (they save lives) and at preventing specific diseases, were also common approaches. Relatively few HCPs use messages directed at dispelling existing myths.
| Message | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Provide information (Any) | 47% | 44% | 48% | 43% | 54% |
| Provide information / research / evidence | 18% | 26% | 28% | 16% | 19% |
| Provide information: risk vs. benefit | 18% | 16% | 18% | 17% | 23% |
| Provide information: personal stories / individual examples | 14% | 6% | 7% | 7% | 16% |
| Provide information: discuss herd immunity / herd health | 3% | 10% | 6% | 10% | 3% |
| Reinforce effectiveness (Any) | 28% | 20% | 26% | 26% | 27% |
| Reinforce effectiveness: prevents diseases / specific diseases | 15% | 7% | 16% | 15% | 18% |
| Reinforce effectiveness: benefits / vaccines save lives | 13% | 6% | 9% | 9% | 9% |
| Reinforce effectiveness: protects the vulnerable (e.g. elderly, children) | 3% | 10% | 5% | 5% | 5% |
| Address concerns (Any) | 19% | 20% | 21% | 15% | 20% |
| Address concerns: reinforce safety of vaccines | 9% | 8% | 8% | 7% | 9% |
| Address concerns / answer questions | 6% | 9% | 11% | 5% | 11% |
| Address concerns: dispel myths | 3% | 4% | 2% | 2% | - |
Q16. Do you have a particularly effective message that really helps vaccine hesitant patients become more comfortable with vaccinations? Base: All respondents NOTE: Only options with at least 4% responses among a given HCP group are included.
HCP respondents have mixed opinions about their comfort level administering or providing advice on vaccines where language barriers exist. Half or fewer or each HCP type said they are at least somewhat comfortable doing so. Nurses and family physicians reported the highest levels of comfort, while midwives and pharmacists are less comfortable. This may be explained by the typical length of time that pharmacists and midwives report having administered vaccines (these two groups are the least experienced).
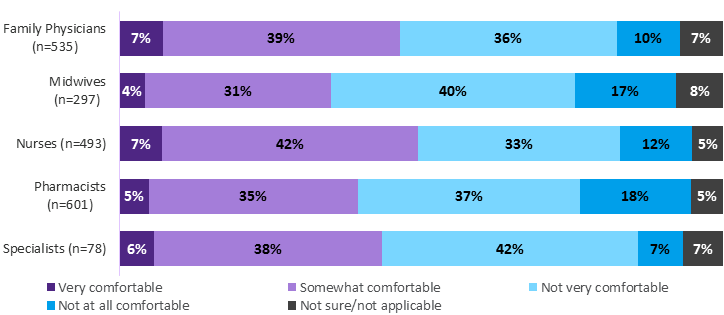
| Profession | Very comfortable | Somewhat comfortable | Not very comfortable | Not at all comfortable | Not sure/not applicable |
| Family Physicians (n=535) | 7% | 39% | 36% | 10% | 7% |
| Midwives (n=297) | 4% | 31% | 40% | 17% | 8% |
| Nurses (n=493) | 7% | 42% | 33% | 12% | 5% |
| Pharmacists (n=601) | 5% | 35% | 37% | 18% | 5% |
| Specialists (n=78) | 6% | 38% | 42% | 7% | 7% |
Q17. How comfortable are you in administering or providing advice on vaccines where language barriers exist? Base: All respondents
Majorities of family physicians, nurses, pharmacists and specialists feel that they have adequate information resources to help them address patient concerns about vaccines. Midwives were the least likely to agree that they had adequate resources, with fewer than half (44%) saying they do.
HCP respondents were considerably less likely to say they have adequate access to resources to support patients in languages other than English or French. Nurses reported the highest access (at 36%) but only around one in five of the other HCP types said they had adequate resources in non-official languages.
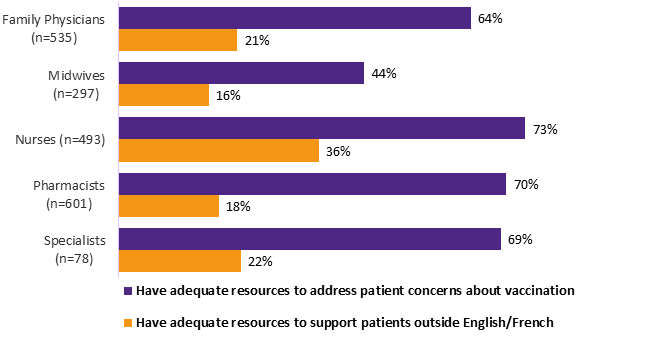
| Profession | Have adequate resources to address patient concerns about vaccination | Have adequate resources to support patients outside English/French |
| Family Physicians (n=535) | 64% | 21% |
| Midwives (n=297) | 44% | 16% |
| Nurses (n=493) | 73% | 36% |
| Pharmacists (n=601) | 70% | 18% |
| Specialists (n=78) | 69% | 22% |
Q19. Do you feel that you have adequate access to information resources that help you address patient concerns about vaccination / to support patients who do not speak English or French? Base: All respondents
HCP respondents were asked where they prefer to get information to update their own vaccination/immunization knowledge, from a list provided (note that this list did not include provincial/ territorial guidance documents such as the Protocole d'immunisation du Québec, which may subsequently be reflected in the 'other resources' category).
The most commonly preferred source among each HCP group is the Canadian Immunization Guide. Statements from the National Advisory Committee on Immunization (NACI) are also preferred by a majority of each HCP group outside of midwives (of whom only 40% prefer it). Medical journals are a preferred source among a majority of family physicians, midwives and specialists. Social media was mentioned by a very small minority of HCP respondents (2-5%).
Conferences are a particular preference among specialists. Nurses are less likely to prefer professional association newsletters than other HCP groups, but more likely to prefer webinars.
| Information Preference | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| The Canadian Immunization Guide | 79% | 70% | 83% | 87% | 83% |
| Statements from the National Advisory Committee on Immunization (NACI) | 68% | 40% | 66% | 71% | 76% |
| Medical journals | 59% | 57% | 39% | 43% | 68% |
| Conferences | 56% | 28% | 47% | 37% | 63% |
| Professional association newsletter | 31% | 46% | 26% | 50% | 55% |
| Webinars | 22% | 22% | 47% | 39% | 19% |
| Other resources | 12% | 15% | 22% | 10% | 6% |
Q20. In general, where do you prefer to get information to update your own vaccination/immunization knowledge? Base: All respondents. NOTE: Only options with greater than 5% responses among a given HCP group are included.
Respondents were shown thumbnail images of PHAC resources and asked if they had ever used or were aware of them.
Awareness. Awareness of existing PHAC resources varies. The Canadian Immunization Guide is the most well-known resource among each group of HCPs, with the great majority aware of it. The PHAC resource "A Parent's Guide to Vaccination" is reasonably well known among nurses and midwives, whereas less than half of family physicians, pharmacists and specialists are aware of it.
Fewer than half of each HCP type are aware of the Canada Communicable Disease Report (CCDR) Journal and the new PHAC products, "Not just for kids. An Adult Guide to Vaccination" and the "Teens, meet Vaccines" guide. Awareness of all three of these tools is higher among nurses.
| % Aware of this resource | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Canadian Immunization Guide (CIG) | 88% | 77% | 89% | 91% | 89% |
| A Parent's Guide to Vaccination | 42% | 61% | 62% | 44% | 46% |
| The Canada Communicable Disease Report journal (CCDR) | 32% | 24% | 45% | 39% | 26% |
| Not just for kids. An Adult Guide to Vaccination | 29% | 19% | 41% | 33% | 18% |
| Teens, meet Vaccines (guide) | 19% | 13% | 30% | 21% | 22% |
Q21. Please indicate if/how you use each of the following PHAC resources for your own knowledge and/or in explaining vaccines to patients. Base: All respondents
Ever used. A majority of all HCP types report having used the Canadian Immunization Guide (CIG) (based on the thumbnail image); this tool is more widely used by pharmacists, nurses and family physicians. The CIG is more commonly used for keeping HCP's own knowledge up to date than to explain vaccines to patients.
The resource "A Parent's Guide to Vaccination" is most commonly used by midwives and nurses, primarily to explain vaccines to patients.
Relatively few HCP respondents have used the Canada Communicable Disease Report Journal, "Not just for kids. An Adult Guide to Vaccination," or "Teens, meet Vaccines", but all three are most widely used by nurses.
| Resource | Usage (% among all respondents) | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) | |
Canadian Immunization Guide (CIG) |
% Ever Use | 73% | 56% | 78% | 79% | 64% |
| % Use to explain vaccines to patients | 20% | 19% | 33% | 35% | 27% | |
| % For own knowledge/staying up to date | 65% | 46% | 68% | 69% | 50% | |
A Parent's Guide to Vaccination |
% Ever Use | 23% | 44% | 39% | 24% | 27% |
| % Use to explain vaccines to patients | 17% | 35% | 34% | 18% | 23% | |
| % For own knowledge/staying up to date | 9% | 16% | 13% | 12% | 5% | |
The CCDR Journal |
% Ever Use | 16% | 14% | 25% | 20% | 10% |
| To explain vaccines to patients | 3% | 2% | 7% | 7% | 0% | |
| Own knowledge/staying up to date | 14% | 13% | 21% | 17% | 10% | |
Not just for kids. An Adult Guide to Vaccination |
% Ever Use | 15% | 8% | 23% | 18% | 7% |
| % Use to explain vaccines to patients | 10% | 4% | 17% | 13% | 4% | |
| % For own knowledge/staying up to date | 7% | 5% | 11% | 12% | 3% | |
Teens, meet Vaccines (guide) |
% Ever Use | 9% | 4% | 15% | 11% | 10% |
| To explain vaccines to patients | 6% | 2% | 12% | 7% | 9% | |
| Own knowledge/staying up to date | 4% | 2% | 7% | 7% | 2% |
Q21. Please indicate if/how you use each of the following PHAC resources for your own knowledge and/or in explaining vaccines to patients. Base: All respondents
Frequency of use. Frequency of use of each of these resources varies considerably, when measured among HCP respondents who have ever used them. The CIG is one of the most frequently used resources on a monthly basis. Although relatively few family physicians make use of most of the PHAC resources outside the CIG, those who do use them make frequent use of the "Teens, meet Vaccines" guide and the "Not just for kids. An Adult Guide to Vaccination" products (just under half use each at least monthly).
| Resource | Usage (% among all respondents) | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Canadian Immunization Guide (CIG) | Sample size | (320) | (134) | (263) | (372) | (42) |
| % Use this resource at least monthly | 46% | 21% | 57% | 49% | 43% | |
| A Parent's Guide to Vaccination | Sample size | (81) | (110) | (122) | (87) | (BTS) |
| % Use this resource at least monthly | 33% | 44% | 45% | 20% | ||
| CCDR | Sample size | (68) | (36) | (98) | (96) | (BTS) |
| % Use this resource at least monthly | 21% | 8% | 31% | 25% | ||
| Not just for kids. An Adult Guide to Vaccination | Sample size | (79) | (25) | (92) | (88) | (BTS) |
| % Use this resource at least monthly | 46% | 15% | 40% | 27% | ||
| Teens, meet Vaccines (guide) | Sample size | (55) | (BTS) | (76) | (70) | (BTS) |
| % Use this resource at least monthly | 47% | 29% | 24% |
Q22. How often do you use <resource>? Base: Respondents who have ever used the resource at Q21 (where respondents use more than two of the listed resources, they were asked about only two of them, assigned randomly). BTS indicates base size too small to report.
Subscribe to CIG email updates. Although a majority of each group of HCPs report using the Canadian Immunization Guide, only a small fraction subscribes to the email updates. Nurses are most likely to do so (19%).

| Profession | % Subscribe |
| Family Physicians (n=535) | 6% |
| Midwives (n=297) | 2% |
| Nurses (n=493) | 19% |
| Pharmacists (n=601) | 6% |
| Specialists (n=78) | 4% |
Q25. Are you subscribed to receive email updates on the Canadian Immunization Guide? Base: All respondents
HCP respondents who do not currently subscribe to the CIG email updates were asked the main reasons why they do not (from a list provided). The top reason given is that they were unaware of the service, cited by roughly four in five non-subscribers. Relatively few give other reasons, such as not having time to read the emails/getting too much email already, that they have sufficient vaccine information or that they do plan to subscribe but just have not done so yet.
| Reason for not subscribing | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample size | (439) | (276) | (374) | (517) | (64) |
| I was unaware of it before today | 86% | 78% | 74% | 79% | 82% |
| Don't have enough time to read it/I get too much email | 14% | 21% | 13% | 14% | 12% |
| I have enough information about vaccines/vaccination | 5% | 4% | 8% | 5% | 12% |
| Plan to subscribe but have not yet | 4% | 5% | 9% | 10% | 6% |
| I prefer other sources of information about vaccines/vaccination | 4% | 5% | 7% | 3% | 3% |
| I am not interested | 2% | 6% | 3% | 2% | 4% |
| Other | 2% | 7% | 8% | 3% | 1% |
Q26. What would you say are the main reasons you do not subscribe to this email update? Base: Respondents who do not subscribe to CIG email updates.
Website. HCP respondents use PHAC's Immunization website for a range of purposes (asked open-ended, without providing response options). The most common theme is that HCPs are trying to locate specific information (e.g. to look up recommendations/the immunization schedule or to verify information). Some HCPs also use it to stay up to date on the most current information. Most of the HCP types use the website in broadly similar ways.
Social media. Very few HCP respondents in any group are aware that PHAC's Chief Public Health Officer has a Twitter account. Fewer than 10% of any profession indicated awareness.
| Reason | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Look up recommendations / information about appropriate vaccines | 25% | 18% | 25% | 36% | 20% |
| Access current information / update myself / stay up to date | 22% | 26% | 30% | 25% | 19% |
| Verify information / confirm information | 20% | 14% | 16% | 18% | 16% |
| Access immunization information | 19% | 18% | 22% | 21% | 15% |
| Access the immunization schedule / confirm the child immunization schedule | 16% | 12% | 12% | 19% | 11% |
| Educate myself / answer my questions | 13% | 13% | 14% | 11% | 18% |
| Research / as a reference / as a resource | 12% | 23% | 23% | 17% | 11% |
| Access the Canadian Immunization Guide / CIG | 5% | 1% | 5% | 5% | 1% |
| Other | 2% | 3% | 2% | 1% | 4% |
| DK / NA | 15% | 13% | 11% | 7% | 24% |
Q35. Please finish the following sentence: I use the Public Health Agency of Canada's Immunization website to...? Base: All respondents
Respondents were asked about the printed health promotion resources they use in their practice (from a list provided). A large majority of HCP respondents from each group use pamphlets, posters and fact sheets (on any topic, and not specifically vaccine-related). These resources are used in a variety of ways by the different HCP types. Family physicians, nurses and specialists are most likely to display or provide them in the waiting room. Providing them to patients during an office appointment is the most common way for midwives and nurses to use these materials, although this practice is common for a majority of each of the HCP groups outside of pharmacists. Family physicians, nurses and specialists also commonly display these materials in interview/exam rooms. Likely due to how their work is structured, nurses and midwives are relatively more likely than the other HCPs to provide printed materials to patients during group sessions or patient home visits. A minority of HCP respondents say they do not use printed health promotion resources in their practice.
| Ways of using printed promotion resources | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Displayed/provided in waiting room | 60% | 60% | 64% | 58% | 66% |
| Given to patient during office appointment | 55% | 70% | 66% | 29% | 51% |
| Displayed in interview/exam room | 47% | 34% | 58% | 20% | 48% |
| During group education sessions (e.g., prenatal class) | 9% | 19% | 23% | 9% | 3% |
| Given to patient during home visits | 3% | 34% | 22% | 5% | 1% |
| I don't use printed resources | 12% | 12% | 6% | 17% | 7% |
| Not sure/Not applicable | 4% | 2% | 4% | 9% | 7% |
Q30. This question is about the health promotion resources you use in your practice, and not just those related to vaccine information. In which of the following ways do you use printed health promotion resources (e.g. posters, pamphlets, fact sheets, or infographics) in your practice? Base: All respondents
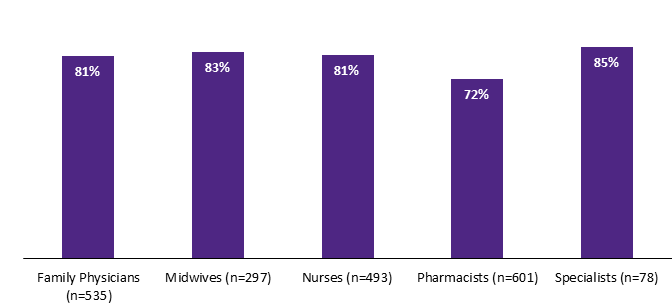
Most HCP respondents hang health promotion or educational posters in their office, clinics and waiting rooms. This is true of a large majority of every HCP group, although the practice is least common among pharmacists (72%).
| Profession | % Subscribe |
| Family Physicians (n=535) | 81% |
| Midwives (n=297) | 83% |
| Nurses (n=493) | 81% |
| Pharmacists (n=601) | 72% |
| Specialists (n=78) | 85% |
Q31. Do you hang any health promotion or educational posters in your office/clinic/waiting room? Base: All respondents
Printed resources. The majority of all HCP types use printed vaccine information materials, most often for their patients or for both their patients and themselves (less commonly just for themselves). Posters, fact sheets and booklets/pamphlets are all used more often than infographs, which the majority of these HCP groups say they have not used. Midwives are less likely than other HCP types to make use of posters about vaccine information.
| Printed Resources | Usage | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) | |
Posters |
For myself only | 4% | 1% | 4% | 3% | 1% |
| For my patients only | 42% | 32% | 40% | 43% | 44% | |
| For both myself and my patients | 27% | 11% | 33% | 26% | 25% | |
| Not sure/Not applicable | 27% | 56% | 22% | 29% | 30% | |
Fact Sheets |
For myself only | 13% | 14% | 6% | 12% | 7% |
| For my patients only | 26% | 16% | 24% | 21% | 27% | |
| For both myself and my patients | 39% | 43% | 59% | 52% | 42% | |
| Not sure/Not applicable | 22% | 27% | 11% | 14% | 23% | |
Booklets or pamphlets |
For myself only | 8% | 7% | 7% | 8% | 11% |
| For my patients only | 26% | 21% | 23% | 26% | 24% | |
| For both myself and my patients | 43% | 48% | 55% | 49% | 43% | |
| Not sure/Not applicable | 23% | 24% | 15% | 16% | 22% | |
Infographs |
For myself only | 8% | 6% | 14% | 11% | 5% |
| For my patients only | 9% | 7% | 8% | 10% | 6% | |
| For both myself and my patients | 17% | 18% | 23% | 19% | 13% | |
| Not sure/Not applicable | 66% | 69% | 55% | 60% | 75% |
Q32. Now thinking specifically about vaccine information, which of the following format(s) do you use for yourself or to provide vaccine information to your patients? Base: All respondents
Digital formats. In general, there is less reported use of digital tools compared to printed ones. The exception is online/digital resources/web portals, which are used by a majority of all HCP groups. Short videos, mobile applications and videos/films/documentaries are used by a minority of HCP respondents; nurses and pharmacists are most likely to report using them.
Notably, these digital tools are much more commonly used for the HCP themselves than are printed tools.
| Digital Resources | Usage | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) | |
Online resources / web portals / digital resources |
For myself only | 31% | 18% | 34% | 49% | 17% |
| For my patients only | 3% | 4% | 3% | 4% | 16% | |
| For both myself and my patients | 35% | 47% | 39% | 27% | 31% | |
| Not sure/Not applicable | 31% | 31% | 23% | 20% | 37% | |
Short Videos |
For myself only | 14% | 7% | 26% | 26% | 10% |
| For my patients only | 4% | 3% | 5% | 5% | 7% | |
| For both myself and my patients | 9% | 11% | 14% | 12% | 8% | |
| Not sure/Not applicable | 72% | 79% | 55% | 56% | 74% | |
Mobile Applications |
For myself only | 10% | 5% | 11% | 18% | 7% |
| For my patients only | 4% | 4% | 10% | 2% | 4% | |
| For both myself and my patients | 13% | 8% | 16% | 13% | 10% | |
| Not sure/Not applicable | 73% | 83% | 63% | 67% | 79% | |
Videos / Films / Documentaries |
For myself only | 12% | 10% | 27% | 26% | 10% |
| For my patients only | 4% | 1% | 2% | 2% | 5% | |
| For both myself and my patients | 8% | 10% | 9% | 8% | 4% | |
| Not sure/Not applicable | 76% | 79% | 62% | 64% | 81% |
Q32. Now thinking specifically about vaccine information, which of the following format(s) do you use for yourself or to provide vaccine information to your patients? Base: All respondents
Relatively few HCP respondents in any group are aware of the free mobile vaccine app CANImmunize, offered by the Ottawa Hospital Research Institute. It is best known by nurses (36% aware).
| % Aware | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| CANImmunize | 16% | 9% | 36% | 19% | 27% |
Q29. Before today, did you know about the free mobile vaccine tracking app called CANImmunize (formerly ImmunizeCA)? Base: All respondents
Sending patients home with printed material about vaccination. Outside of midwives, a majority of HCP respondents regularly provide printed materials to patients to take home with information about vaccinations (such as pamphlets and fact sheets). A large majority of nurses (77%) say they do this often or sometimes, while around six in ten family physicians, pharmacists and specialists and less than half (45%) of midwives report doing so. Few HCPs in any group say they never send patients home with printed information about vaccines.

| Profession | Often | Sometimes | Rarely | Never | Do not use |
| Family Physicians (n=535) | 17% | 44% | 23% | 5% | 11% |
| Midwives (n=297) | 19% | 27% | 26% | 10% | 19% |
| Nurses (n=493) | 40% | 37% | 13% | 2% | 7% |
| Pharmacists (n=601) | 17% | 39% | 26% | 6% | 11% |
| Specialists (n=78) | 19% | 42% | 22% | 9% | 9% |
Q33. How often do you send patients home with print material about vaccinations such as pamphlets or fact sheets? Base: All respondents
Use of social media platforms to learn and share information about vaccination and other health topics is not widespread. Fewer than three in ten of any HCP type say they do so; this is more common among nurses, midwives and pharmacists. The most common platform is Facebook, while very few use Twitter or other social media platforms.
| Usage | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Use any (net) | 14% | 28% | 25% | 27% | 15% |
| 10% | 24% | 20% | 21% | 9% |
Q34. What social media platform(s), if any, do you use to learn and/or share information about vaccination or other health topics? Base: All respondents
HCP respondents were asked what PHAC can do to assist them in addressing patient reluctance about vaccinations (open-ended, without providing response options). Generally, the ideas fall into three categories. First, HCPs would like to see PHAC raise public awareness of the issue, possibly through advertising or a media campaign, or by providing social or traditional media content. A second suggestion is to educate and inform the public, by providing evidence, reinforcing the benefits of vaccines, and dispelling myths. Third, some HCPs would like printed materials or guides on the topic.
| Suggestions | Family Physicians | Midwives | Nurses | Pharmacists | Specialists |
| Sample Size | (535) | (297) | (493) | (601) | (78) |
| Provide more advertising / launch a media campaign | 12% | 2% | 5% | 13% | 8% |
| Provide education / public education | 11% | 14% | 16% | 14% | 13% |
| Provide information / science-based research / evidence / analysis | 11% | 16% | 12% | 7% | 12% |
| Provide printed materials / posters / pamphlets | 9% | 5% | 4% | 9% | 15% |
| Improve awareness / public awareness | 7% | 7% | 6% | 8% | 8% |
| Provide social media content | 7% | 4% | 9% | 7% | 6% |
| Address concerns - dispel myths | 6% | 6% | 8% | 6% | 7% |
| Address concerns / answer questions (general) | 5% | 15% | 5% | 3% | 8% |
| Reinforce effectiveness / benefits / vaccines save lives (general) | 4% | 6% | 5% | 5% | 5% |
| Provide radio / television content | 4% | 0% | 6% | 5% | 1% |
| Other | 5% | 7% | 4% | 4% | 4% |
| No / nothing / Don't know / No answer | 22% | 19% | 20% | 21% | 14% |
Q38. Based on your experience, do you have any suggestions on how the Public Health Agency of Canada can assist healthcare professionals in addressing patient reluctance about vaccination? Base: All respondents NOTE: Only suggestions mentioned by at least 5% of HCPs in any group are displayed.
The research results indicate that Canadian healthcare professionals of all types are encountering patient reluctance around vaccines on a fairly regular basis; this appears to have translated into widespread concern about the impact on public health. HCPs are encountering the full gamut of patient concerns, including concerns about safety, lack of trust in institutions and under-estimating the threat of disease, nor are the concerns limited to only one or two vaccines. HCPs have not identified a single 'magic bullet' for addressing these concerns with patients, and their approach largely depends on the patient group and the specific concern raised.
HCPs are reasonably confident in their ability to address patient vaccine concerns, but there is room for improvement. They widely report using the Canadian Immunization Guide (CIG) to inform themselves, but few subscribe to the CIG email updates due to a lack of awareness. There is also lower awareness and use of other PHAC resources. Making HCPs more aware of these resources and promoting their usefulness for specific patient types would be of benefit by supporting HCPs and providing them with tools to help educate their patients. A perceived lack of vaccine-related resources in languages other than English and French is also a key gap worth addressing.
The different HCP types each have specific areas where they feel comfortable and have expertise with respect to vaccines. It will be challenging to build HCP's comfort level providing vaccines and advice to patient types outside their typical practice scope. Instead, the focus should be on providing supports of specific relevance to each of the health professions. This will ensure a multi-pronged approach to reaching the Canadian public at all ages and stages of life.
Subject line: The Public Health Agency of Canada wants to hear from you about vaccination.
Dear [contact],
You are invited to participate in an online survey about vaccination, an important issue facing healthcare professionals. The survey is being conducted by Environics Research, an independent research company, on behalf of the Public Health Agency of Canada.
Participants who qualify and complete the survey will receive a $25 (CAD) Virtual Visa electronic Gift card!
The survey will take about 15 minutes to complete. You will be asked for your opinions about your experiences with vaccine practices. Your participation is voluntary and completely confidential. All your answers will remain anonymous and will be combined with responses from other participants. Please note that responses throughout the survey should NOT include personal information or information about specific cases.
If you don't have time to complete the survey in one sitting, you can return to it by clicking on the link below again. Once the survey period closes on [DATE], if you decide not to complete the entire survey, your answers will not be retained.
Please click on the following link to complete the survey in English:
Insert link
Please click on the following link to complete the survey in French:
Insert link
This survey is registered with the Marketing Research and Intelligence Association. Click here [pop-up in new browser windowFootnote *] to verify its authenticity.
If you have any questions about the survey, please contact Sarah Roberton of Environics Research by phone 613-699-6884) or email (sarah.roberton@environics.ca) or Martine Dubuc of the Public Health Agency of Canada at phone 613-851-0281) or email (martine.dubuc2@canada.ca).
To learn more about vaccines in Canada, please visit Canada.ca/vaccines
Welcome and thank you for your interest in our survey.
D1. In which province or territory do you practice?
01 British Columbia
02 Alberta
03 Saskatchewan
04 Manitoba
05 Ontario
06 Quebec
07 New Brunswick
08 Nova Scotia
09 Newfoundland & Labrador
10 Prince Edward Island
11 Yukon
12 Northwest Territories
13 Nunavut
98 Practising outside Canada thank and terminate: "Thank you. We are only looking for professionals working in Canada at this time"
D2. What is your primary profession?
Select one only
01 Registered Nurse (RN)
02 Nurse Practitioner
03 Family Physician/General Practitioner
04 Obstetrician/Gynecologist
05 Paediatrician
06 Midwife (RM or AM)
07 Pharmacist
88 Other, please specify:
This survey will ask you about your day-to-day experience with your patients/clientele and vaccination. By vaccination, we mean routine recommended vaccines, such as DTaP-IPV and MMR for children, or pertussis and tetanus for adults. Please exclude travel vaccines and flu shots from your answers. Please ensure that your responses do NOT include personal information or information about specific cases.
01 Yes
02 No thank and terminate: "Thank you. We are only looking for professionals who administer or provide advices on vaccines at this time."
01 Less than 1 year
02 1 to 5 years
03 6 to 15 years
04 More than 15 years
01 Daily
02 A few times a week
03 About once a week
04 Less often than once a week
01 Infants/young children (0-6yrs)
02 Children (7-17yrs)
03 Adults (18-64yrs)
04 Seniors (65yrs+)
05 Pregnant women
99 other (do not specify)
a. Express reluctance, concern or hesitation about vaccination;
b. Refuse a vaccine altogether;
c. Request an alternate schedule (e.g. wishes to delay, "spread out" vaccines, or does not want to receive the recommended number of doses).
Repeat scale for each of above
01 Every time
02 Most of the time
03 Some of the time
04 Rarely
05 Never
a. A patient expresses reluctance, concern or hesitation about vaccination
b. A patient refuses a vaccine altogether
c. A patient requests an alternate schedule (e.g. wishes to delay, "spread out" vaccines, or does not want to receive the recommended number of doses)
d. A patient expresses strong support for vaccines
e. A patient seems knowledgeable about vaccines/vaccination
f. A patient mentions incorrect information about vaccines/vaccination
Repeat scale for each of above
01 More often
02 Less often
03 About the same
04 Not sure
Rotate order of blocks and battery items within each block. Show the section headings.
select all that apply
7.1Under-estimating threat of disease
01 Believe the vaccine is not needed anymore (as the disease is gone or almost gone)
02 Believe that the disease is not a big concern ("I had it when I was a kid and I'm OK")
7.2 Concerns about vaccine safety
03 Think there are too many antigens in vaccines
04 Worried about specific ingredients in vaccines (e.g., mercury, thimerosal)
05 Think there are too many injections being given at one time
06 Think it is better to wait until child is older
07 Worried about immediate side effects (i.e. adverse events following immunization)
08 Worried about possible long term effects
09 Worried that the vaccine will actually cause the illness it is meant to prevent
10 Fear of needles/Find needles too painful
11 Know or heard of someone who had an adverse reaction to a vaccine
7.3 Concerns about vaccine effectiveness
12 Concerned vaccines don't protect against the disease
7.4 Beliefs in alternatives to vaccines
13 Believe alternate therapies are a better choice (e.g., homeopathy)
14 Believe natural immunity is enough
15 Believe if other children are vaccinated their own children do not need to be
7.5 Lack of trust in institutions
16 Conspiracy theories (pharmaceutical companies and/or government)
17 Distrust of healthcare professionals
7.6 Other
18 Religious beliefs do not allow for/discourage vaccination
19 Find it difficult to get the vaccine (e.g. time off work, transportation to clinic, too busy)
88 Other, please specify:
98 None
99 Not sure/Not applicable
7a. (If >3 codes selected at q7) Of the reasons you identified in the previous question, which are the top 3 reasons you hear most frequently from patients as to why they do not want themselves or their family members vaccinated?
Programmer note: show the responses selected in Q7.
IF Q4= 01: Infant Vaccines
01 Diphtheria, tetanus, pertussis, polio, haemophilus influenzae type B (DTaP-IPV-Hib)
02 Diphtheria, tetanus, pertussis, hepatitis B, polio, haemophilus influenzae type (DTaP-HB-IPV-Hib)
03 Hepatitis A (HA)
04 Hepatitis B (HB)
05 Hepatitis A & B (HAHB)
06 Measles, Mumps, Rubella (MMR)
07 Measles, Mumps, Rubella, Varicella (MMRV)
08 Varicella (chickenpox)
09 Meningococcal
10 Pneumococcal
11 Rotavirus
75 All infant vaccines
IF Q4=02: Children's and Adolescent Vaccines
21 Diphtheria, tetanus, pertussis, polio (DTaP-IPV) / Tetanus, diphtheria, pertussis, polio (Tdap-IPV)
22 Tetanus, diphtheria, pertussis (Tdap)
23 Hepatitis A (HA)
24 Hepatitis B (HB)
25 Hepatitis A & B (HAHB)
26 Measles, Mumps, Rubella (MMR)
27 Measles, Mumps, Rubella, Varicella, (MMRV)
28 Varicella (chickenpox)
29 Meningococcal
30 Human papillomavirus (HPV)
76 All children's/adolescent vaccines
IF Q4=03/04/05: Adult Vaccines
31 Tetanus, diphtheria (Td)
32 Tetanus, diphtheria, pertussis (Tdap)
33 Hepatitis A (HA)
34 Hepatitis B (HB)
35 Hepatitis A & B (HAHB)
36 Meningococcal
37 Pneumococcal
38 Herpes zoster (shingles)
39 Human papillomavirus (HPV)
77 All adult vaccines
98 None/no patients identified specific vaccines they are reluctant to receive
99 Not sure/Not applicable
01 Very prepared
02 Somewhat prepared
03 Not very prepared
04 Not at all prepared
99 Not sure
| Statement | Strongly agree (4) | Somewhat agree (3) | Somewhat disagree (2) | Strongly disagree (1) | Not sure (99) |
| Vaccines in use in Canada are safe | |||||
| Vaccines are as safe as or safer than other prescription medications | |||||
| In general, vaccines in use in Canada are effective | |||||
| It is important to give vaccines at the recommended times (according to the provincial or territorial schedule) | |||||
| Administering multiple vaccines at a single visit could reduce their efficacy | |||||
| Administering multiple vaccines at a single visit could overwhelm the immune system | |||||
| I trust that the vaccine regulatory system in Canada is safe and working effectively | |||||
| The pharmaceutical industry pushes certain vaccines for profit only | |||||
| I trust the recommendations of the National Advisory Committee on Immunization | |||||
| Administering the HPV vaccine to adolescents could increase their likelihood of engaging in unprotected sexual activity | |||||
| It is important to inform patients about all vaccines recommended for their age/condition, even if not publicly funded |
01 Yes
02 No (skip to question 14)
99 Not sure/ Not applicable (skip to question 14)
IF Q4= 01: Infant Vaccines
01 Diphtheria, tetanus, pertussis, polio, haemophilus influenzae type B (DTaP-IPV-Hib)
02 Diphtheria, tetanus, pertussis, hepatitis B, polio, haemophilus influenzae type (DTaP-HB-IPV-Hib)
03 Hepatitis A (HA)
04 Hepatitis B (HB)
05 Hepatitis A & B (HAHB)
06 Measles, Mumps, Rubella (MMR)
07 Measles, Mumps, Rubella, Varicella (MMRV)
08 Varicella (chickenpox)
09 Meningococcal
10 Pneumococcal
11 Rotavirus
75 All infant vaccines
IF Q4=02: Children's and Adolescent Vaccines
21 Diphtheria, tetanus, pertussis, polio (DTaP-IPV) / Tetanus, diphtheria, pertussis, polio (Tdap-IPV)
22 Tetanus, diphtheria, pertussis (Tdap)
23 Hepatitis A (HA)
24 Hepatitis B (HB)
25 Hepatitis A & B (HAHB)
26 Measles, Mumps, Rubella (MMR)
27 Measles, Mumps, Rubella, Varicella, (MMRV)
28 Varicella (chickenpox)
29 Meningococcal
30 Human papillomavirus (HPV)
76 All children's/adolescent vaccines
IF Q4=03/04/05: Adult Vaccines
31 Tetanus, diphtheria (Td)
32 Tetanus, diphtheria, pertussis (Tdap)
33 Hepatitis A (HA)
34 Hepatitis B (HB)
35 Hepatitis A & B (HAHB)
36 Meningococcal
37 Pneumococcal
38 Herpes zoster (shingles)
39 Human papillomavirus (HPV)
77 All adult vaccines
99 - Not sure
01 Concerned about safety/potential side effects
02 Concerned about vaccine effectiveness
03 Do not believe they are needed (i.e. no longer see the disease it prevents)
04 Not publicly funded
05 Too expensive
88 Other, please specify:
99 Not sure
| Age group | Very comfortable (4) | Somewhat comfortable (3) | Not very comfortable (2) | Not at all comfortable (1) | No sure/Not applicable (99) |
| a. Infants/young children (0-6yrs) | |||||
| b. Children (7-17yrs) | |||||
| c. Adults (18-64yrs) | |||||
|
|||||
| e. Pregnant women | |||||
| f. Individuals with chronic diseases (e.g. diabetes, asthma) | |||||
| g. Individuals who are immunocompromised (e.g. cancer, HIV) |
The next few questions are about your experiences speaking with patients about vaccination.
01 Very Comfortable
02 Somewhat comfortable
03 Not very comfortable
04 Not at all comfortable
99 Not sure/ Not applicable
a. that help you address patient concerns about vaccination
b. to support patients who do not speak English or French
01 Yes
02 No
Not sure/ Not applicable
01 Medical journals
02 Professional association newsletter
03 The Canadian Immunization Guide
04 Statements from the National Advisory Committee on Immunization (NACI)
05 Conferences
06 Webinars
07 Social media
88 Other, please specify:
| Resource (thumbnail images provided beside name of each resource) |
I use to explain vaccines to patients (4) |
I use for my own knowledge and for staying up to date (3) |
I am aware of this resource but have never used [exclusive option] (2) |
I am not aware of this resource [exclusive option] (1) |
I'm not sure [exclusive option] (99) |
| Canadian Immunization Guide (CIG) | |||||
| A Parent's Guide to Vaccination | |||||
| Not just for kids. An Adult Guide to Vaccination | |||||
| Teens, meet Vaccines (guide) | |||||
| The Canada Communicable Disease Report journal (CCDR) |
ASK Q22-24 SERIES FOR UP TO 2 RESOURCES USED (CODE 3-4) AT Q21 (RANDOM SELECTION):
01 Daily
02 Weekly
03 Monthly
04 Less than a few times a year
01 Yes SKIP TO Q.27
02 No
99 Not sure SKIP TO Q.27
01 I am not interested
02 I was unaware of it before today
03 Plan to subscribe but have not yet
04 I have enough information about vaccines/vaccination
05 I prefer other sources of information about vaccines/vaccination
06 Don't have enough time to read it/I get too much email
07 Previously subscribed but did not find the information useful
88 Other (specify):
01 In most cases, my own reading of the scientific literature and/or the product monograph would be enough
02 I prefer to consult with colleagues, such as immunization experts or my local public health department
03 I prefer to wait until the vaccine is listed in my provincial/territorial immunization schedule or manual
04 I prefer to wait for recommendations from the National Advisory Committee on Immunization in the Canadian Immunization Guide
98 Other (specify)
99 Not sure
01 Yes
02 No
99 Not sure
01 Yes
02 No
99 Not sure
01 Displayed/provided in waiting room
02 Displayed in interview/exam room
03 Given to patient during office appointment
04 Given to patient during home visits
05 During group education sessions (e.g., prenatal class)
98 I don't use printed resources
99 Not sure/Not applicable
01 Yes
02 No
| For myself only (1) | For my patients only (2) | For both myself and my patients (3) | Not sure / Not applicable (99) |
|
| Printed resources | ||||
| Booklets or pamphlets | ||||
| Fact sheets | ||||
| Posters | ||||
| Infographs | ||||
| Digital resources | ||||
| Short videos | ||||
| Videos / Films / Documentaries | ||||
| Online resources / web portals / digital resources | ||||
| Mobile applications (e.g. CANImmunize) |
01 Often
02 Sometimes
03 Rarely
04 Never
99 Not sure
Check all that apply
01 Twitter
02 Facebook
03 LinkedIn
04 Instagram
88 Other, please specify:
99 I do not use any social media platforms for this purpose
I use the Public Health Agency of Canada's Immunization website to…. OPEN TEXT BOX - Non Mandatory
01 A significant issue
02 Somewhat of an issue
03 Not a very big issue
04 Not an issue at all
99 Not sure
Section 8: Respondent Characteristics
The following are questions to help us to group the results. Your responses will be anonymous and kept strictly confidential.
D3. What type of setting best describes your primary place of practice?
Select one only
01 Paediatric hospital setting
02 Other hospital setting
03 Family medicine clinic
04 Public Health clinic/setting
06 Long term care residence
07 Homecare setting
08 Pharmacy
09 School setting
88 Other (do not specify)
D4. Which of the following best describes the area where your primary place of practice is located?
01 Large urban population centre (>100,000 individuals)
02 Medium population centre (30,000 to 100,000 individuals)
03 Small population centre (1000 to 29,999 individuals)
04 Rural location
05 First Nations community (on-reserve)
D5. What are the first three digits of the postal code of your primary place of practice?
___ ___ ___
999 999 - Prefer not to answer
D6. Would you consent to being contacted on occasion by the Public Health Agency of Canada to provide your views on the development of new or updated vaccination education and/or awareness products?
01 Yes
02 No
Thank you for taking the time to participate in this survey. Please click on the Submit button to register your answers. You will receive your incentive payment once the study is complete (January 2018).
Survey redirects to http://environicsresearch.com/
MRIA registration info opens in pop-up browser window