Common menu bar links
Institutional links
Diseases & Conditions
Health & Safety
Research & Statistics
Agency Information
Search Box
A Report on Governments' Responses to the HIV/AIDS Epidemic in Canada
A National Portrait
Previous | Table of Contents | Next
3. HIV/AIDS by Jurisdiction
3.1 Canada
Surveillance Highlights
- the number of people living with HIV/AIDS may increase significantly through the coming years given the number of new infections combined with people living longer with HIV/AIDS because of the new treatment options available.
- there was approximately the same number of newly reported cases of HIV infection in 2003 as in 2002. However the number in 2003 (2,482) was higher than the number in either 2001 (2,187) or 2000 (2,127).
- unlike in the epidemic's early years, there is now a greater proportion of women, those using injection drugs and Aboriginal people who are being infected.
- the proportion of new HIV positive reports attributed to MSM has decreased from close to 75% between 1985-1994 to approximately 37% in the mid to late 1990's. There has been a slight increase in this category through the last three years, to 44%. The IDU exposure category represented 9% of positive HIV reports before 1994, increased to 33% in 1996 and 1997 and decreased to 12% in 2003. The diverse heterosexual exposure category15 has steadily increased from 7.5% before 1995 to 36.9% in 2003. From 1998 to 2003, the proportion of positive HIV test reports attributed to the endemic country heterosexual subcategory has increased from 2.9% to 10.2%.
- females represent a growing proportion of positive HIV test reports. For the last three years females have accounted for approximately one quarter of positive HIV test reports in which sex is known. This represents a rise from 8.9% during the period between 1985 and 1992.
Canada16
| Indicator | Year | ||||
|---|---|---|---|---|---|
| 2003 | 2002 | 2001 | 2000 | 1995 | |
| Prevalence Estimate (HIV and AIDS) | >56,000 | 56,000 | 49,90017 | 40,10018 | |
| AIDS Cases | |||||
| Number of AIDS cases diagnosed by year | 218 | 357 | 384 | 471 | 1,655 |
| Cumulative number of AIDS cases reported | 19,344 | 19,126 | 18,769 | 18,385 | 14,838 |
| Newly reported adult AIDS cases by sex: | |||||
| male | 163 | 300 | 321 | 405 | 1,496 |
| female | 52 | 52 | 59 | 56 | 130 |
| Newly reported adult AIDS cases by exposure category | |||||
| MSM | 71 | 117 | 151 | 218 | 1,091 |
| MSM/IDU | 5 | 6 | 14 | 15 | 74 |
| IDU | 36 | 50 | 48 | 92 | 130 |
| Heterosexual contact19 | 12 | 24 | 21 | 25 | 101 |
| HIV endemic country20 | 38 | 51 | 54 | 42 | 88 |
| NIR - HET21 | 38 | 23 | 32 | 32 | 38 |
| Blood/blood products | 1 | 2 | 7 | 7 | 43 |
| NIR22/Other | 14 | 39 | 35 | 31 | 63 |
| Newly reported AIDS cases by age | |||||
| <1-14 | 3 | 4 | 3 | 5 | 27 |
| 15-29 | 19 | 27 | 29 | 27 | 205 |
| 30-49 | 161 | 252 | 272 | 346 | 1,217 |
| 50+ | 35 | 74 | 80 | 84 | 206 |
| AIDS-related deaths | 93 | 103 | 187 | 263 | 1,500 |
| HIV Infection | |||||
| Number of positive HIV test reports | 2,482 | 2,504 | 2,187 | 2,127 | 2,996 |
| Positive HIV test reports by exposure category (Adult) | |||||
| MSM | 361 | 506 | 401 | 469 | 684 |
| MSM/IDU | 12 | 19 | 33 | 27 | 58 |
| IDU | 96 | 302 | 279 | 288 | 452 |
| Heterosexual contact | 78 | 165 | 177 | 136 | n/a |
| HIV-endemic countries | 83 | 91 | 70 | 52 | n/a |
| Heterosexual contact/HIV-endemic countries23 | 114 | ||||
| NIR-Het | 139 | 129 | 114 | 94 | 104 |
| Blood/blood products | 6 | 11 | 10 | 15 | 28 |
| Other/NIR | 94 | 91 | 91 | 97 | 186 |
| Not reported | 1,571 | 1,139 | 952 | 869 | 1,283 |
| Positive HIV test reports by sex (Adults) | |||||
| Men | 1 816 | 1 815 | 1 591 | 1 533 | 2 266 |
| Women | 615 | 620 | 524 | 484 | 534 |
| Positive HIV test reports by age | |||||
| <15 years | 9 | 18 | 16 | 17 | 59 |
| 15-19 years | 25 | 34 | 32 | 34 | 28 |
| 20-29 years | 485 | 481 | 411 | 408 | 712 |
| 30-39 years | 939 | 982 | 853 | 849 | 1,284 |
| 40-49 years | 702 | 670 | 569 | 526 | 577 |
| > 50 years | 289 | 286 | 262 | 230 | 234 |
| Age not reported | 33 | 33 | 44 | 63 | 85 |
Organization
The federal efforts to address the epidemic began in the mid-1980s but were more fully coordinated after 1990 with the first and second National AIDS Strategies. In 1997 the Government of Canada announced a new Canadian Strategy on HIV/AIDS (CSHA) that was intended to be pan-Canadian in nature and to provide a coherent, national framework for addressing the epidemic. The CSHA is generally perceived as having been successful, for example in terms of developing community capacity, placing HIV/AIDS in a human rights context and encouraging both scientific and social research.24
The CSHA has 10 strategic areas, i.e.:
- research
- community development and support to national non-governmental organizations
- care, treatment and support
- surveillance
- prevention
- Aboriginal communities
- consultation, evaluation, monitoring and reporting
- legal, ethical and human rights
- Correctional Service Canada
- international collaboration
Management responsibility lies primarily with the HIV/AIDS Policy, Coordination and Programs Division within the Public Health Agency of Canada (PHAC), although important roles are also played by the regional PHAC offices responsible for the AIDS Community Action Program (ACAP), the Surveillance and Risk Assessment Division (PHAC), the National HIV and Retrovirology Laboratories (PHAC), the First Nations and Inuit Health Branch (Health Canada), International Affairs Directorate (Health Canada), Correctional Service Canada and the Canadian Institutes of Health Research25. Intergovernmental cooperation is facilitated by the PHAC and Health Canada regional offices and by both the FPT AIDS Committee and the FPT Heads of Corrections Working Group on Health. Both of these intergovernmental committees include representatives from all jurisdictions in Canada. The Minister of Health is advised by the Ministerial Council on HIV/AIDS, which has representatives of different types of expertise, including people living with HIV/AIDS. The National Aboriginal Council on HIV/AIDS advises the PHAC and Health Canada on HIV/AIDS issues that affect the Aboriginal peoples of Canada.
The CSHA's annual budget is $42.2 million with the largest proportions being directed to research ($13.2 million) and to community development/ support to non-governmental organizations ($10 million). In 2003, additional amounts were committed by:
- the First Nations and Inuit Health Branch, Health Canada ($2.5 million); and
- the Canadian Institutes of Health Research ($4.7 million).26
Correctional Service Canada has also allocated $7.7 million for a National Methadone Maintenance program (of which $1 million comes from the Canadian Drug Strategy) and a total of $13 million for infectious disease prevention, screening, care, treatment and surveillance activities.
Canada has also made a significant contribution to the international effort to address HIV/AIDS. The Canadian International Development Agency has increased its annual funding for international HIV/AIDS programs from $22 million in 2000/01 to $80 million in 2004/05, for a total five-year investment of $270 million. In 2001, Canada also pledged $100M (USD) over four years to the Global Fund to Fight AIDS, Tuberculosis and Malaria while in 2004 it committed to effectively doubling its annual contribution. In May 2004, Canada announced a $100 million contribution to the World Health Organization (WHO) "3 by 5 Initiative." This represents over half of the current funding gap estimated by WHO for the years 2004 and 2005. Finally, Canada has committed $62 million from the Canada Fund for Africa towards the development of an AIDS vaccine and to support the work of a Canadian coalition on HIV/AIDS on the social impact of the disease, including children's education, labour and family structures. All in all, the country's five-year international investment will be more than $500 million.
Domestically, the federal government has recently announced its intention to increase the CSHA's budget to $84.4 million annually, to be phased in over five years. The Report of the Standing Committee on Health (Strengthening the Canadian Strategy on HIV/AIDS), the Five Year Review of the CSHA, Leading Together: An HIV/AIDS Action Plan for all Canada, PHAC research and input from stakeholders are guiding the development of a new policy framework for a renewed federal initiative.
Coordination and Cooperation
The CSHA incorporates a commitment to cooperation, multi-sectoral partnerships and consensus "[a]t every stage of planning and delivery...."27 A series of direction setting meetings were held and ongoing advisory groups were established (for example the Ministerial Council on HIV/AIDS and the National Aboriginal Council on HIV/AIDS) to guide the development and implementation of the CSHA, and keep it responsive to emerging issues. The Working Group on International HIV/AIDS Issues brings together several government departments and non-governmental organizations to discuss international collaboration.
PHAC, both nationally and regionally, provides funding to non-governmental organizations in recognition of the vital partnership they bring to the response. These include national organizations such as the Canadian AIDS Society, the Canadian Aboriginal AIDS Network, the Canadian HIV/AIDS Legal Network, the Canadian AIDS Treatment Information Exchange, the Canadian Treatment Action Council, the Interagency Coalition on AIDS and Development, Canadian Public Health Association, and the Canadian Working Group on AIDS and Rehabilitation.
In a similar vein, the First Nations and Inuit Health Branch of Health Canada works with and funds a variety of national and regional organizations - for example, the Assembly of First Nations and the Canadian Aboriginal AIDS Network - to undertake health promotion and HIV/AIDS-related educational efforts among Aboriginal people and particularly among the Inuit and those First Nations people living on reserve. The Health Canada regional offices also work with and provide both operational and project funding to community organizations for similar purposes. This contribution is particularly significant in those jurisdictions where both the number of people living with HIV/AIDS and the provincial/territorial contribution are relatively small.
The government/community relationship is now characterized as being both strong and mature although the commitment to consultation has been described by some key informants as slowing the decision-making process. Nevertheless, coordination and collaboration are considered to be vital given the clear benefits associated with engaging community-level knowledge and experience.
Intergovernmental collaboration and cooperation are also vital given the country's federal structure wherein responsibility for health services lies primarily with the provinces and territories even while the Government of Canada has the ability to influence health policy through its roles in setting and administering national standards and enforcing the Canada Health Act, and through financial transfers. The federal government has endeavoured to provide leadership to the Canadian effort by assuming direct responsibility for certain activities and by enabling others to assume responsibility for other activities.28
Testing, Prevention, Care and TreatmentFor the most part, the federal government is not directly involved in testing, care or treatment activities. Nevertheless it plays an active role in the effort to address HIV/AIDS at the community level, for example:
- its AIDS Community Action Program, with offices in each region, provides multi-year operational and project funding to a broad range of community organizations that are involved in a diverse array of community activities.
- it has a fiduciary responsibility for providing health care to the Inuit and to First Nations people living on reserve. The First Nations and Inuit Health Branch in Health Canada provides funding for health promotion efforts, medical treatment including HIV testing, certain drug treatments that are not covered by provincial programs and medical transportation for those having to travel for care or treatment.
- it has a direct responsibility for providing health care to those incarcerated in federal correctional institutions and to those serving in the military and the Royal Canadian Mounted Police.
- its efforts (since January, 2002) to ensure that all applicants for permanent residence in Canada older than fifteen years of age are tested for HIV.29
- its national community project funding for First Nations people living off reserve and for Inuit and Métis communities, as well as for capacity building, best practices models, information services, public information and legal, ethical and human rights.
The federal government has also played a major role in hosting national meetings and conferences, funding pilot projects, maintaining a national surveillance system and funding important research including cohort studies. Additionally, Health Canada and the Canadian Aboriginal AIDS Network have launched an educational campaign designed to enhance awareness and dialogue among First Nations, Inuit and Métis people.30 The on reserve effort faces the challenge of preserving confidentiality while endeavouring to understand the size and scope of the epidemic in those communities.
Knowledge
The federal government and the CSHA have played an important role in creating, organizing, analyzing and disseminating epidemiological and other knowledge. The federal government is uniquely well placed to blend information and experiences from many different jurisdictions, and to promote efforts to embed this knowledge in practice through information exchanges such as those of the AIDS Community Action Program (ACAP).
Federal funding, most often through the Canadian Institutes of Health Research, has enabled Canadian researchers to contribute in a very significant way to the national and international effort to address the epidemic. These researchers are also playing an important role in certain clinical trials, in assessing treatment regimens and in the international effort to develop a vaccine. Canada has also promoted a health determinants approach to the epidemic, emphasizing the impact of discrimination, stigma and other social and economic factors on HIV vulnerability. Addressing these health determinants is seen as the key to reducing vulnerability and preventing the epidemic's spread, and has become embedded in the ACAP program.
Importantly the CSHA has endeavoured to address controversial issues such as harm reduction and to raise the tenor of public discussion by funding projects on topics such as building capacity among drug users and best practices in needle exchange. Given the importance of disseminating and applying new knowledge, PHAC also funds the Canadian HIV/AIDS Information Centre (formerly, the Canadian HIV/AIDS Clearinghouse) and the Canadian AIDS Treatment Information Exchange.
Finally, PHAC gathers surveillance data from each jurisdiction and provides national-level reports and analysis. It supports surveillance efforts in some jurisdictions through its Field Surveillance Officer (FSO) positions. Currently, these PHAC FSOs are working with their provincial counterparts in Vancouver, Calgary, Regina, Winnipeg, Toronto and Halifax. PHAC also supports surveillance efforts by partnering with the provinces and territories to standardize national definitions and data collection methods and, where required, by developing software applications.
Strengthening the Effort
The literature and key informants identified the following as means for strengthening the federal government's effort to address the HIV/AIDS epidemic:
- clarify priorities, goals and performance measures within the CSHA.
- provide the leadership necessary for building public support for controversial prevention and harm reduction programs.
- provide funds adequate to the many tasks associated with addressing the epidemic.
- effectively address the epidemic among certain particularly vulnerable groups, for example gay men, Aboriginal people living on and off reserve, those incarcerated in federal correctional institutions, women and those using injection drugs.31
3.2 British Columbia
Surveillance Highlights
- there are approximately 10,500 people in BC today living with HIV/AIDS, an increase of approximately 1,000 since 1999.
- the HIV incidence rate declined from 19.6 (/100,000 population) in 1990 to 18.2 in 1995 and 10.2 in 2000. The rate increased to 10.7 in 2001 and 2002 before declining again in 2003 to 10.1.32
- in 2003, MSM accounted for 36.5% of newly reported HIV+ cases for which the exposure category was known. The IDU exposure category accounted for 25.7% and heterosexual transmission for 24.9%. The equivalent proportions in 2000 were 37.4%, 32.0% and 19.7%. In other words, the proportion among MSM remained much the same while that for IDU declined and that for heterosexual transmission increased.
- women accounted for 21.5% of newly reported HIV cases in 2003 compared to 21.3% in 2000 and 22.4% in 1995.
- in 2003, Aboriginal people accounted for 16.0% of newly reported HIV cases for whom ethnicity was identified. Women accounted for almost 42% of these Aboriginal cases. In 1995, Aboriginal people accounted for 16.7% of newly reported HIV cases for whom ethnicity was identified.
British Columbia33
| Indicator | Year | ||||
|---|---|---|---|---|---|
| 2003 | 2002 | 2001 | 2000 | 1995 | |
| Prevalence Estimate | 10,50034 | 9,50035 | |||
| AIDS Cases | |||||
| Number of AIDS cases reported by year | 75 | 88 | 77 | 144 | 335 |
| Cumulative number of AIDS cases reported | 3,730 | 3,655 | 3,567 | 3,490 | 2,599 |
| Newly reported AIDS cases by sex | |||||
| male | 66 | 79 | 70 | 126 | 308 |
| female | 9 | 8 | 7 | 16 | 26 |
| Newly reported AIDS cases by exposure category | |||||
| MSM | 5 | 25 | 29 | 64 | 220 |
| MSM/IDU | 2 | 3 | 3 | 5 | 15 |
| IDU | 16 | 15 | 12 | 32 | 41 |
| Heterosexual contact | 5 | 6 | 6 | 13 | 33 |
| Other (haemophiliac, unknown, etc.) | 47 | 39 | 27 | 30 | 26 |
| Newly reported AIDS cases by age | |||||
| <15 year | 0 | 1 | 2 | 2 | 3 |
| 15-29 | 6 | 5 | 7 | 10 | 42 |
| 30-49 | 45 | 57 | 45 | 102 | 245 |
| 50+ | 24 | 24 | 23 | 28 | 44 |
| unknown | 0 | 1 | 0 | 2 | 1 |
| Newly reported AIDS cases by ethnicity | |||||
| Caucasian | 30 | 37 | 50 | 99 | 250 |
| Aboriginal | 6 | 6 | 6 | 13 | 29 |
| Asian | 0 | 2 | 6 | 1 | 4 |
| Other & unknown | 39 | 43 | 15 | 31 | 52 |
| HIV Infection | |||||
| Total number of newly reported HIV+ cases | 423 | 438 | 437 | 408 | 682 |
| Newly reported HIV+ cases by exposure category | |||||
| MSM | 135 | 148 | 134 | 133 | 185 |
| MSM/IDU | 24 | 12 | 20 | 10 | 28 |
| IDU | 95 | 145 | 121 | 114 | 267 |
| Heterosexual contact | 92 | 98 | 103 | 70 | 68 |
| Sex Trade Worker/IDU | 18 | 15 | 11 | 19 | 40 |
| Sex Trade Worker | 2 | 0 | 1 | 1 | 0 |
| All other | 4 | 9 | 10 | 9 | 10 |
| Unknown | 53 | 11 | 37 | 52 | 84 |
| Newly reported HIV+ cases by sex | |||||
| Men | 328 | 353 | 345 | 321 | 526 |
| Women | 90 | 85 | 87 | 87 | 152 |
| Unknown | 5 | 0 | 5 | 0 | 4 |
| Newly reported HIV+ cases by ethnicity | |||||
| Caucasian | 246 | 276 | 285 | 253 | 384 |
| Aboriginal people | 59 | 66 | 69 | 58 | 90 |
| men | 34 | 39 | 38 | 36 | 55 |
| women | 25 | 27 | 31 | 22 | 34 |
| unknown | 0 | 0 | 0 | 0 | 1 |
| Asian | 28 | 47 | 28 | 25 | 30 |
| Black | 22 | 17 | 24 | 18 | 15 |
| Hispanic | 13 | 24 | 10 | 8 | 19 |
| Unknown | 55 | 8 | 21 | 46 | 144 |
| Newly reported HIV+ cases by age | |||||
| Perinatal (<18 months) | 1 | 0 | 1 | 2 | 1 |
| <15 years | 2 | 1 | 3 | 1 | 4 |
| 15-29 | 76 | 75 | 110 | 94 | 203 |
| 30-49 | 261 | 295 | 271 | 256 | 426 |
| 50+ | 82 | 66 | 50 | 54 | 41 |
| Unknown | 1 | 1 | 2 | 1 | |
Organization
British Columbia has long been guided by a provincial strategy in its effort to address HIV/AIDS, first the 1998 British Columbia's Framework for Action on HIV/AIDS and subsequently a new Priorities for Action in Managing the Epidemics, HIV/AIDS in British Columbia 2003-2007. The latter's purpose is "to complement, guide and support community and health authority efforts to address what is one of the most serious public health challenges in B.C. today."36 It is intended to serve as a blueprint, providing direction to the health authorities, community partners and provincial ministries as they each play their part in the provincial effort to address and manage the epidemic.
Priorities for Action recognizes that HIV/AIDS "is a complex disease that cannot yet be fully prevented." Its focus, therefore, is "on managing the epidemics through sustained effort in four key areas: prevention; care, treatment and support; capacity; and coordination and cooperation."37 Importantly, it establishes ambitious and quantifiable goals for the period 2003 to 2007, i.e.:
- to reduce by 50% both the number of people becoming infected each year and the number of people who are HIV-positive but unaware of their infection;
- to increase by 25% the proportion of HIV-positive individuals who are linked to appropriate services;
- to enhance the province's capacity for monitoring the HIV epidemic; and
- to create and sustain broad-based support for Priorities for Action.
The document establishes measurable objectives and key strategies for each goal and includes a commitment to monitoring and accountability for the health authorities and other partners. These accountability measures have not yet been put in place, however, and may have to be considerably more specific and focused than what the government normally expects of the health authorities. Complementing Priorities for Action is a Chee Mamuk report on the epidemic among Aboriginal people and an older Aboriginal strategy prepared by the BC Aboriginal HIV/AIDS Task Force.38
The Priorities document has been well received by portions of the community and has been described as a useful tool for their own purposes. Some are particularly taken by the province assuming the risk of articulating such ambitious goals and express the hope that it will actively pursue these goals. Other community sources, meanwhile, raise concerns that they were not involved in developing Priorities for Action and that there are not new funds attached to it.
The Ministry of Health Services is responsible for managing and monitoring the province-wide efforts and plans to enhance its capacity to do so and to create mechanisms for encouraging coordination and cooperation among stakeholders. It is assisted by the BC Centre for Disease Control (BCCDC) particularly with regard to monitoring the epidemic and the Aboriginal aspect of the epidemic. The BC Centre for Excellence in HIV/AIDS is responsible for administering the province's anti-retroviral drug program.
The Provincial Health Officer estimated in 2003 that British Columbia spent approximately $100 million on HIV-related services.
Coordination and Cooperation
Coordination and cooperation constitute an important element in the BC effort. The province's platform for action on HIV/AIDS consists of six health authorities, five having regional responsibilities and one having responsibility for specialized, province-wide programs and services. Together, these health authorities and their community partners have been challenged by Priorities for Action to develop and deliver the range of programs and services needed to achieve the provincial goals. There is some concern among key informants, however, that the level of cooperation between AIDS Service Organizations and the health authorities will vary significantly from region to region, and that there will not be any central coordination or planning. However three of the Health Authorities have completed service plans and another three are in the process of developing their plans.
The provincial Ministry of Education has developed a sexual health component for its curricula. The Ministry of Health Planning is developing a relationship with the Solicitor General's department and, in concert with the health authorities, is attempting to develop protocols for addressing HIV/AIDS-related issues within the province's correctional centres.
British Columbia participates in the FPT AIDS Committee and in the FPT Heads of Corrections Working Group on Health. There is a strong working relationship with the regional PHAC office responsible for the AIDS Community Action Program although provincial and federal resources are managed separately. There is considerable concern in the province with the jurisdictional and service divide between Aboriginal people living on and off reserve, particularly in light of the epidemic's presence among Aboriginal people and their movement between communities.
British Columbia has not integrated its HIV/AIDS-related efforts with its other public health and blood borne pathogen efforts although certain Health Authorities are moving in that direction. Importantly, municipalities are playing a larger role in the effort to address the epidemic, for example in Vancouver with its "four pillar" approach and in Victoria where discussions are underway about enhancing harm reduction services.
Testing, Prevention, Care and Treatment
La province offre des services de dépistage prénatal du VIH au moyen d'un modèle d'adhésion volontaire, c'est-à-dire qu'on demande aux femmes si elles souhaitent qu'un test The province offers prenatal testing for HIV using an opt-in model that asks women whether they wish to be tested. Between October and December 2003, the provincial laboratory received 10,900 prenatal specimens and had permission to test 8,650 (79%) for HIV. As presented in Table 2, the total number of HIV tests performed has increased slowly over time and in 2002 totalled over 146,000.39 In total 1.6 million tests have been performed since 1985.
| 1995 | 1997 | 1999 | 2001 | 2002 | 2003 |
|---|---|---|---|---|---|
| 130,338 | 140,278 | 135,284 | 135,806 | 146,489 | 135,654 |
Some key informants expressed concern that the province's health care system focuses too heavily on acute care and devotes insufficient attention and resources to prevention, primary care and population health. They suggested that more vigorous leadership is required in this regard.
Knowledge
The BC Centre for Excellence in HIV/AIDS is a Canadian and international leader in terms of generating and disseminating new knowledge on all aspects of the epidemic. The BC Centre for Disease Control, meanwhile, has provided training to different groups of professionals, hosts the Chee Mamuk Aboriginal program and partners with a variety of community-based AIDS-related organizations. Certain key informants suggested there is a need to improve the timeliness of the HIV/AIDS-related data disseminated by the BCCDC so they better inform community services.
It is also suggested that greater attention and emphasis needs to be placed on outcome-based evaluation in order to ensure that always limited resources are being spent in the most effective manner possible.
Strengthening the Effort
Key informants suggested a variety of means for strengthening the province's effort to address the epidemic:
- enhance public awareness and political commitment and leadership at all levels. There is a concern that HIV/AIDS has "fallen off the public radar" and consequently is no longer a priority.
- build a more effective sentinel surveillance system that better captures trends within the most vulnerable populations.
- place greater emphasis upon prevention and population health.
- commit additional financial resources to the epidemic and for both the Health Authorities and the community-based service organizations. Two key informants suggested that "everything is in place to address the epidemic except for the level of resources needed to do so."
- nstitute a system of tied federal transfers, with strict accountability requirements, in order to foster more effective intergovernmental cooperation and to ensure that federal dollars are used to achieve the province's public health goals.
- roaden membership on inter-sectoral committees addressing HIV/AIDS by including representatives of community organizations, the Health Authorities and other governments.
- stablish a "champion" among the health authorities to assume leadership responsibility for HIV/AIDS.
3.3 Alberta
Surveillance Highlights40
- there are approximately 3,200 people living with HIV/AIDS in Alberta.
- in 2003, the rate for newly reported cases of HIV was much higher in Edmonton than in Calgary, at 7.0 and 5.4/100,000 respectively. Exposure category patterns vary significantly by region with IDU being most common in Edmonton and MSM in Calgary. In that year, however, there was a proportionate rise among MSM in both cities.
- provincially, in 2003, the most commonly reported exposure category was MSM (39% of all cases) followed by IDU (22%).
- between 1999 and 2003, 30% of all newly reported HIV cases were among Aboriginal people who account for approximately 5% of the province's total population. This varied by region however, and in 2003, 32% of new infections in the Edmonton area occurred among Aboriginal people compared to 5% in the Calgary area.
Alberta41
| Notes: Data extracted by Year of Reporting. Age Groups constructed using Age at Report Date. N/A = not available |
|||||
| Indicator | Year | ||||
|---|---|---|---|---|---|
| 2003 | 2002 | 2001 | 2000 | 1999 | |
| Prevalence Estimate | N/A | N/A | N/A | N/A | 3,200 |
| AIDS Cases | |||||
| Number of AIDS cases reported by year | 40 | 33 | 42 | 49 | 41 |
| Cumulative number of AIDS cases reported | 1,160 | 1,119 | 1,087 | 1,045 | 996 |
| Newly reported AIDS cases by sex | |||||
| male | 28 | 28 | 37 | 42 | 38 |
| female | 12 | 5 | 5 | 7 | 3 |
| Newly reported AIDS cases by exposure category | |||||
| MSM | 13 | 9 | 19 | 22 | 16 |
| IDU | 8 | 10 | 10 | 10 | 6 |
| MSM and IDU | 0 | 1 | 4 | 2 | 4 |
| Hetero Endemic/Partner at Risk/NIR | 18 | 10 | 8 | 15 | 14 |
| Other | 0 | 3 | 1 | 0 | 1 |
| Unknown | 1 | 0 | 0 | 0 | 0 |
| Newly reported AIDS cases by age | |||||
| children & youth (0-19 yrs) | 0 | 1 | 0 | 0 | 0 |
| adults (20-59 yrs) | 37 | 32 | 38 | 48 | 41 |
| seniors (60+ yrs) | 3 | 0 | 4 | 1 | 0 |
| AIDS-related deaths | 6 | 4 | 11 | 17 | 11 |
| HIV Infection | |||||
| Total number of reported HIV cases | 157 | 179 | 168 | 191 | 162 |
| Newly reported cases of HIV infection by exposure category | |||||
| MSM | 61 | 34 | 36 | 53 | 38 |
| MSM/IDU | 1 | 5 | 6 | 2 | 6 |
| IDU | 35 | 76 | 65 | 79 | 64 |
| HIV/AIDS-endemic countries | 15 | 18 | 18 | 14 | 18 |
| Heterosexual contact - Partner at Risk | 25 | 20 | 22 | 20 | 11 |
| NIR - Heterosexual | 19 | 18 | 19 | 21 | 22 |
| NIR-Other | 0 | 8 | 2 | 1 | 3 |
| Perinatal | 0 | 0 | 0 | 1 | 0 |
| Unknown | 1 | 0 | 0 | 0 | 0 |
| Newly reported cases of HIV infection by sex | |||||
| Men | 121 | 122 | 123 | 127 | 117 |
| Women | 36 | 57 | 45 | 64 | 45 |
| Newly reported cases of HIV infection by ethnicity | |||||
| White | 88 | 81 | 85 | 101 | 101 |
| Black | 17 | 20 | 20 | 16 | 18 |
| Aboriginal | 40 | 68 | 58 | 64 | 31 |
| Asian | 7 | 5 | 4 | 8 | 5 |
| Other | 4 | 4 | 1 | 1 | 5 |
| Unknown Ethnicity | 1 | 1 | 0 | 1 | 2 |
| Newly reported cases of HIV infection by age | |||||
| 0-14 yrs | 0 | 0 | 0 | 1 | 0 |
| 15-24 yrs | 19 | 13 | 16 | 22 | 24 |
| 25-59 yrs | 131 | 165 | 146 | 165 | 136 |
| 60+ yrs | 7 | 1 | 6 | 3 | 2 |
Organization
In 1999, Alberta first articulated an HIV/AIDS Strategy encompassing the period 1998/99 to 2002. Although it did not have specific or quantifiable goals and objectives, it proved to be an important plan for addressing HIV/AIDS and, according to one key informant, for providing "permission to go forward with different initiatives." It was also useful for identifying different stakeholders' roles and responsibilities, including Alberta Health and Wellness, the Regional Health Authorities, community AIDS organizations and Health Canada.
Work is currently underway on a replacement strategy that will have measurable goals and accountability requirements, and will again identify the roles and responsibilities of key stakeholders in the prevention, treatment, care and support of people living with HIV/AIDS. It will be premised upon a population health perspective. The new Strategy will more fully integrate HIV/AIDS with other blood-borne pathogens and sexually transmitted infections (STIs) in the expectation that approach may:
- again raise the profile of HIV/AIDS and its interactions with other blood-borne pathogens and STIs;
- help overcome the "silos" that can compromise effective action and result in more support and resources given the promise of reduced duplication; and
- better reflect the community level reality where HIV/AIDS-related organizations have already incorporated hepatitis C and other STIs into their efforts.
Alberta Health and Wellness provides approximately $2.3 million to support community-based programming through the Alberta Community HIV Fund and an additional $70,000 for the Non-Prescription Needle Use Project.42 The province also funds a community developer who provides blood-borne prevention programming primarily to off reserve Aboriginal groups. Other funding is provided through the Regional Health Authorities' global budgets.
Coordination and Cooperation
There is a strong working relationship with the regional PHAC office, and the provincial and federal governments have worked together to create an innovative model for funding. The Alberta Community HIV Fund (ACHF) is a joint community/provincial/federal funding disbursement model developed through consultation with representatives from community-based HIV/AIDS organizations, persons living with HIV/AIDS, the Regional Health Authorities, and provincial and federal health departments. The ACHF replaces both the PHAC guidelines for the AIDS Community Action Program and the Alberta Health and Wellness guidelines for community organization grants.
The fund provides for a simplified and transparent funding process that helps to prevent duplication and improve coordination. Through its operational and project-based funding,43 the ACHF supports:
- efforts to create supportive environments and to provide care and support;
- prevention, harm reduction and health promotion initiatives; and
- measures to strengthen community-based organizations.
This funding approach is seen by many as a best practice for joint work between federal and provincial governments.
Testing, Prevention, Care and Treatment
Alberta faces a significant challenge in that its epidemics are different from region to region. In Edmonton, for example, the epidemic is concentrated in the inner city with the exposure categories being primarily injection drug use and heterosexual transmission, and with Aboriginal people being the most vulnerable group. In Calgary, meanwhile, the epidemic is much more heavily concentrated in the MSM population
Regional Health Authorities undertake contact tracing on First Nations reserves but the federal/provincial realms of responsibility inhibit the development of comprehensive and seamless services for Aboriginal people. The high degree of movement between reserves or settlements and urban centres increases the challenges associated with locating Aboriginal people for follow-up services.
While some reserve communities are increasingly committed to tackle the issues of blood borne pathogens, a harm reduction approach (for example, providing sexual health education and condoms in schools) continues to be misunderstood or rejected in other communities. Concerns around confidentiality, especially in small reserve communities and Métis settlements, may also prevent some Aboriginal people from seeking testing. Additionally, awareness of and access to culturally appropriate information on how to prevent, manage and control disease may serve as barriers to some Aboriginal peoples.
In September 1998, Alberta introduced a prenatal HIV screening program that strongly recommends testing all pregnant women for HIV. This "opt-out model," recommended by the Canadian Medical Association,44 offers women HIV testing during pregnancy with the option to decline. Informed consent remains a vital part of this initiative, however. This approach has resulted in approximately 95%-98% of all pregnant women in Alberta being tested for HIV.
Figure 5 illustrates the progressive increase in the total number of HIV serology tests conducted in Alberta each fiscal year since 2000/01.
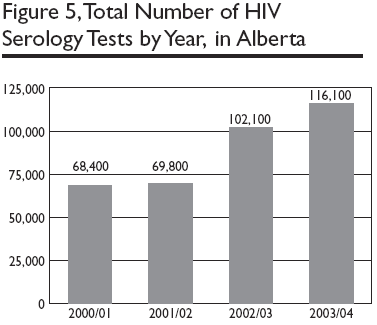
Alberta also offers anonymous testing but only one of three sites in the province has been accessed by a small number of clients in the past two years.
HIV clinical services and antiretroviral costs are funded through a separate province-wide fund, with Edmonton coordinating the Northern Alberta HIV program and Calgary the Southern Alberta program. Several HIV physicians also conduct regular clinics in five provincial and federal correctional facilities. Furthermore, the province funds a toll free STI/HIV information line that provides both recorded information 24 hours a day and access to a nurse during business hours.
The Non Prescription Needle Use (NPNU) initiative, formed in 1995, is a coordinated response of 39 government departments, agencies, organizations and community groups to reduce the harms associated with injection drug use particularly as they relate to HIV and Hepatitis C. Field level staff work with policy makers to identify issues, develop programs and policies, and work collaboratively to improve the health of those who inject drugs.
The NPNU has worked to provide greater access to methadone in the province and the number of methadone clinics has increased from one, situated in Edmonton, to five across the province. There are now two clinics in Edmonton, one in Red Deer and two in Calgary. A provincial Opioid Dependency Treatment Coordinating Committee will set direction for the delivery of this treatment in Alberta.
Key informants suggested that the range of supports and services needed to address the HIV/AIDS epidemic in Alberta are largely in place. However they identified a need:
- for public education and for programs targeted to youth and to men who have sex with men;
- to focus greater attention on Aboriginal people and communities whether on or off reserve;
- to provide the range of social supports - such as housing - that can help to reduce HIV vulnerability; and
- to meet the needs of people living in small communities given the issue of confidentiality and the cost of medical travel.
Knowledge
The Government of Alberta invests in research through the Alberta Heritage Foundation for Medical Research. Importantly, the Foundation places considerable emphasis on disseminating and applying research. Its Research in Practice initiative and newsletter, for example, were "established to ensure that important research findings make their way into clinical practice and policy settings as quickly as possible."45 Additionally the Alberta Community Council on HIV receives funding from PHAC to support a research coordinator who can assist agencies undertaking community-based research.
Strengthening the Effort
Key informants suggested a variety of means for strengthening the province's response to the epidemic:
- commit resources - although not necessarily new resources - to the emerging provincial strategy.
- respond to Aboriginal aspects of the epidemic by building relationships with First Nations and Inuit Health Branch in Health Canada, Aboriginal people and communities, Regional Health Authorities, HIV/AIDS-related agencies and other service organizations.
- enhance the ability to follow-up on identified cases particularly in rural areas.
- strengthen the prevention effort at the community, provincial and national level, and recognize that prevention campaigns must be consistent, aggressive and sustained through the long term.
- address the epidemic among populations coping with a variety of barriers such as addictions, mental health problems and housing issues.
- address the stigma and discrimination that are still associated with HIV/AIDS.
15 This exposure category is made up of three subcategories: heterosexual contact with a person who is either HIV-infected or at increased risk of HIV infection; heterosexual as the only identified risk; and origin in a country where HIV is endemic.
16 Primary source is Canada, Health Canada, 2004. Selected data for 1995 drawn from the Health Canada Surveillance Report, December 2000.
18 Prevalence estimate for 1996. See Canada, Health Canada, 2000:197.
19 Sexual contact with a person at risk.
20 Origin from an HIV-endemic country.
21 NIR-HET: Heterosexual contact is the only risk factor reported and nothing is known about the HIV-related risk factors associated with the partner.
23 Prior to 1997, it was not possible to separate the exposure categories "heterosexual contact with a person at risk" and "origin from an HIV-endemic country."
24 For a review of the CSHA, see Spigelman, 2003.
25 The Public Health Agency of Canada was created on September 24, 2004, and is largely comprised of the former Population and Public Health Branch (PPHB) of Health Canada. The HIV/AIDS Policy, Coordination and Programs Division, the Surveillance and Risk Assessment Division and the National HIV and Retrovirology Laboratories, and former regional PPHB offices are now part of the new Agency.
26 Canada, Health Canada, 2003(d):5.
27 Canada, Health Canada, 2003(d):6.
29 Canada, Health Canada, 2003(d):11.
30 Canada, Health Canada, 2003(d):10.
32 BC Centre for Disease Control (BCCDC), 2002:17.
33 Division of STD/AIDS Control, BC Centre for Disease Control Society, July 2004. See also BCCDC, HIV/AIDS Update, Annual 2002.
34 Estimated by the BCCDC to be between 8,000 and 13,000.
38 See BCCDC, 2000 and BC Aboriginal AIDS Task Force, 1999.
40 Alberta Blood-borne Pathogens Surveillance Working Group, 2003:5-6; Communicable Disease Reporting System, May 4, 2004.
41 Communicable Disease Reporting System, May 4, 2004. Prepared by Disease Control and Prevention, Alberta Health and Wellness. HIV data are available only from May 1998.
42 The Health Canada contribution to the Alberta Community HIV Fund is approximately $683,000.
43 Project funds range in size from $5,000 to $20,000.
44 Alberta Blood-borne pathogens Surveillance Group, 2003:20.
45 See http://www.ahfmr.ab.ca/publications/reports/hrip2000/from_to.php and http://www.ahfmr.ab.ca/publications/.
