Common menu bar links
E-mail this page
Evaluation of the Hepatitis C Prevention, Support and Research Program 1999/2000 – 2005/2006
Previous | Table of Contents | Next
6. Program Successes, Challenges, Gaps and Lessons Learned
The successes, challenges, gaps and lessons learned are identified for the key Program components: (1) research and surveillance; (2) prevention and community-based support; (3) care and awareness; and (4) management, policy, evaluation and public involvement.
6.1 Successes, Challenges and Gaps Remaining
While the Program had many successes, there were significant challenges associated with their achievement. These are discussed along with the gaps identified in the Five-Year Program Review.
6.1.1 Research and Surveillance Component
In partnership with the Canadian Institutes of Health Research (CIHR), the research component was, ultimately, one of the Program's greatest successes. Prior to the Hepatitis C Prevention, Support and Research Program, there was minimal Canadian research capacity in HCV and only a few scientific publications per year. Over the seven-year history of the joint initiative:
- Committed $16.5 million dollars to research operating grants, $1.7 million to salary awards and $1.1 million to training awards;
- Awarded 64 research grants spanning the four pillars of CIHR research: biomedical research, clinical research, health services research and population health research;
- Granted 5 salary awards (3 at the Investigator level, and 2 at the New Investigator level) and 12 training awards (9 fellowships, 2 doctoral research awards and one MD/PhD studentship); and
- Established the National Canadian Research Training Program (NCRTP), a major initiative to bring new scientists to the field, establish mentorships and establish new research areas including psycho-social issues; overall, leading to improved science to improve treatment, care and research knowledge.
However, a continuing challenge for the research component was the lack of sufficient, sustainable strategic funding to conduct HCV research in Canada. The 2006 research compendium, “Turning Research into Action,” indicated several repercussions including: the potential loss of research capacity in terms of new researchers entering the field, loss of research infrastructure (i.e., loss of the extensive funding required to equip labs to study HCV); and the overall loss of momentum and interest in HCV research initially engendered by the joint initiative. For example, over the extension years, grants that were already in place could be extended; however, there were no new requests for proposal (RFP) for multi-year projects.
Key informants commented that the Program “really missed an opportunity to continue the research program over the extension years and further advance social/behavioural research”. Informants noted the lack of multi-year funding had a devastating impact on the process of reviewing and implementing health research projects, i.e., identifying priorities, inviting proposals, reviewing proposals and, once proposals are accepted, planning and executing the research, analyzing the results and writing a report. Without long-term stability, no new research could be undertaken.
Both the Mid-term Evaluation and the Five-Year Program Review identified a gap in the quantity of research focusing on behavioural and social science issues, noting that this knowledge is necessary for developing effective HCV prevention, care and treatment strategies. While some progress was made, this gap still remains. The research compendium reported: “Lack of funding directed towards social behavioral research in general, and research on the social determinants of health associated with HCV infection in particular. Although the Social and Behavioural Research Issues in HIV and Hepatitis C request for proposals was launched specifically to respond to this issue, only four projects were funded under this initiative.”
Another significant gap was the implementation of an effective national structure which would enable adequate research knowledge-transfer-and-exchange. This structure would support dissemination of research findings among researchers from different disciplines, within the same discipline, to care professionals, to policy makers and to people living with, or at risk of, hepatitis C. The document review also found that only 14.1% (39 of 276) documents were related to increasing research knowledge.
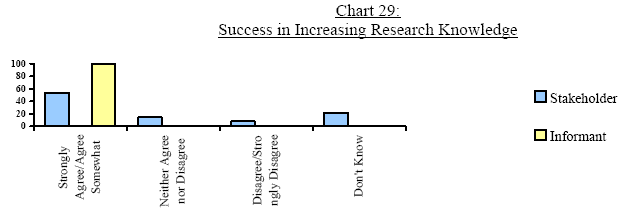
The repercussion of this gap is most clearly seen in stakeholder responses to whether the Program was able to increase research knowledge. Only 54.3% of stakeholders “strongly agreed/agreed somewhat” compared to 100% of key informants.
In Chart 29, it is interesting to note the high percentage of stakeholders who “didn't know” (21.3%) whether the Program was able to increase research knowledge. Key informant comments provided some insight indicating both the translation and dissemination of research knowledge was a challenge, and the application of research was lacking. Therefore, “even though bio-medical research knowledge increased, the lack of social/behavioural research meant that important questions were left unanswered: Why is there vulnerability? Why are some people at risk? What are the best ways to intervene? When are the best times to intervene?”
While some progress has been made on “[continuing and enhancing] coordinated and collaborative efforts in tracking, and [enhancing] surveillance of risk behaviours and community acquired infections”, this area continues to present significant challenges. Key informants suggested that surveillance should have been a more prominent component of the Program. Indeed, the document review found a paucity of nationally and regionally funded reports on slowing the spread of HCV, STIs, HBV and TB; only 8.3% (23 of 276) of documents reviewed were related to surveillance activities.
Surveillance issues related “to [building] a meaningful and mutually enriching rapport between those involved in research, epidemiology and surveillance of infectious diseases and those involved in designing and delivering programs”, were discussed in a meeting of the Hepatitis C, HIV/AIDS and STI programs held September 200523. The participants generally agreed:
- There is an absence of national standardized data collection;
- There are contradictions in evidence sources (federal, provincial);
- Some communities may not report at all or do not report in a consistent and / or timely manner; and
- Some provinces do not readily share their data.
The surveillance gap remains: “Surveillance systems need to be improved to answer the question “why”; if the evidence can be linked to goals, goals need to be measurable and operationalized, and the system must allow assessment of long term impact. Goals lend themselves to the policy context that should connect with what is happening on the ground. The challenge… is how to make this policy real.”24
References
| 23. |
Lise Pigeon & Associates. Report on the Meeting of the Hepatitis C, HIV/AIDS and STI Programs and Evidence. September 26-28, 2005. |
| 24. |
Ibid. |
Previous | Table of Contents | Next
