


   |
|||||||||||||||||
| |
||
| |
||
|
Volume 29-13
|
UPDATE: SEVERE ACUTE RESPIRATORY
|
|
| Figure 1. Number* of reported cases of severe acute respiratory syndrome, by classification and date of illness onset -Ontario, 23 February to 7 June, 2003 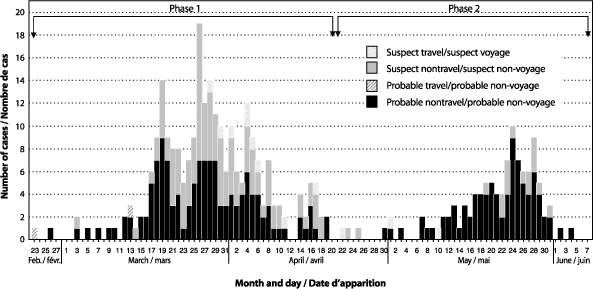 * N=361. Figure 2. Number* of reported cases of severe acute respiratory syndrome, by source of infection and date of illness onset - Toronto Canada, 15 April to 9 June, 2003
|
||
|
Editorial Note On 14 May, 2003, the WHO removed Toronto from the list of areas with recent local SARS transmission because 20 days (i.e. twice the maximum incubation period) had elapsed since the most recent case of locally acquired SARS was isolated or a SARS patient had died, suggesting that the chain of transmission had terminated. Before recognition of the second phase of the outbreak, the most recent case of locally acquired SARS in Toronto had been reported before 20 April. However, unrecognized transmission, limited initially to patient-to-patient and patient-to-visitor transmission, was apparently continuing in hospital A. After directives for increased hospital-wide infection control precautions had been lifted, an increase in the number of cases was observed, particularly among HCWs. The findings from this investigation underscore the importance
of controlling health care associated SARS transmission and highlight
the difficulty in determining when expanded precautions for SARS are no
longer necessary. Investigations in Canada and other countries have identified
HCWs to be at increased risk of SARS, and methods for performing surveillance
among HCWs have been recommended(2). The Toronto investigation
suggests that unrecognized patient-to-patient and patient-to-visitor transmission
of SARS might have been occurring with no associated cases of HCW illness
until after a province-wide lifting of the expanded precautions for SARS.
Transient carriage of pathogens on the hands of HCWs is the most common
form of transmission for several nosocomial infections, and both direct
contact and droplet spread appear to be major modes of SARS-CoV transmission(3).
HCWs should be directed to use gloves appropriately (e.g. change gloves
after every patient contact and avoid their use outside a patient's
room) and to pay scrupulous attention to hand hygiene before putting on
and after removing gloves. In addition to active and passive surveillance for fever
and respiratory symptoms among HCWs, early detection of SARS cases among
people in health care facilities in SARS-affected areas is critical, particularly
in facilities that provide care to SARS patients. Identifying hospitalized
patients with SARS is difficult, especially when no epidemiologic link
has been recognized and the presentation of symptoms is nonspecific. Patients
with SARS might develop symptoms common to hospitalized patients (e.g.
fever or prodromal symptoms of headache, malaise, and myalgias), and diagnostic
testing to detect cases is limited. Available nucleic acid amplification
assays for SARS-CoV have reported sensitivities as low as 50%(4).
Although serologic testing for SARS-CoV antibody is available, definitive
interpretation of an initial negative test requires a convalescent specimen
to be obtained > 21 days after onset of symptoms(5). Several potential approaches for monitoring patients might
improve recognition of SARS in hospitalized patients. A standardized assessment
for SARS (e.g. clinical, radiographic, and laboratory criteria) might
be used among all hospitalized patients with fever of new onset, especially
for units or wards in which clusters of febrile patients are identified.
In addition, some hospital computer information systems might allow review
of administrative and physician order data to monitor selected observations
that might serve as triggers for further investigation. The Toronto investigation found early transmission of SARS
to both patients and visitors in hospital A. In areas affected recently
by SARS, clusters of pneumonia occurring in either visitors to health
care facilities or HCWs should be evaluated fully to determine whether
they represent transmission of SARS. To facilitate detection and reporting,
clinicians in these areas should be encouraged to obtain a history from
pneumonia patients of whether they visited or worked at a health care
facility and whether family members or close contacts are also ill. Targeted
surveillance for community-acquired pneumonia in areas recently affected
by SARS might provide another means of early detection of these cases. The findings from the Toronto investigation indicate that
continued transmission of SARS can occur among patients and visitors during
a period of apparent HCW adherence to expanded infection control precautions
for SARS. Maintaining a high level of suspicion for SARS on the part of
health care providers and infection control staff is critical, particularly
after a decline in reported SARS cases. The prevention of health care
associated SARS infections must involve HCWs, patients, visitors, and
the community. References 1. Poutanen SM, Low DE, Henry B et al. Identification of severe acute respiratory syndrome in Canada. N Engl J Med 2003;348(20):1995-2005. 2. CDC. Interim domestic guidance for management of exposures to severe acute respiratory syndrome (SARS) for health-care settings. URL: <http://www.cdc.gov/ncidod/sars/exposureguidance.htm>. 3. Seto WH, Tsang D, Yung RW et al. Effectiveness of precautions against droplets and contact in prevention of nosocomial transmission of severe acute respiratory syndrome (SARS). Lancet 2003;361:1519-20. 4. Peiris JS, Lai ST, Poon LL et al. Coronavirus as a possible cause of severe acute respiratory syndrome. Lancet 2003;361:1319-25. 5. Stohr K. A multicentre collaboration to investigate the cause of severe acute respiratory syndrome. Lancet 2003;361:1730-33. Source: SARS Investigation Team, CDC; T Wallington, MD, L Berger, MD, B Henry, MD, R Shahin, MD, B Yaffe, MD, Toronto Public Health; B Mederski, MD, G Berall, MD, North York General Hospital; M Christian, MD, A McGeer, MD, D Low, MD, University of Toronto; Ontario Ministry of Health and Long-term Care, Toronto. T Wong, MD, T Tam, MD, M Ofner, L Hansen, D Gravel, A King, MD, Health Canada, Ottawa.
|
||
| Last Updated: 2003-07-01 | |||