|
[Table of
Contents]
Ā
|
Ā
|
Volume: 22S1 • April 1996
Guidelines for Preventing the Transmission of
Tuberculosis in Canadian Health Care Facilities and
Other Institutional Settings
IV. TB MANAGEMENT PROGRAM
D. Strategies for Managing Suspected or Confirmed
Infectious TB
Management strategies for handling suspected or
confirmed infectious TB in health care facilities
should include the following:
- programs for early identification and evaluation
of persons with suspected infectious TB;
- immediate isolation of persons with suspected or
confirmed infectious TB;
- notification of infection control personnel;
- efficient confirmation of diagnosis;
- early and appropriate initiation of treatment;
- notification of public health authorities;
- identification, assessment and management of
contacts, including the provision of isoniazid (INH)
preventive therapy for selected contacts; and
- evaluation of TB exposure events.
1. Programs for the Early Identification and
Evaluation of Persons with Suspected Infectious
TB
Identification of individuals with active TB
involves a careful evaluation of those known to be in
high-risk groups or presenting with the symptom complex
described below and a time course compatible with a
diagnosis of infectious TB(9,15,26,41-45).
Efforts to detect active TB should be vigorous and
thorough and should begin on initial encounter, and
even before admission, if possible. All HCWs should
participate in the early identification of persons with
suspected TB.
2. Isolation of Persons with Suspected or
Confirmed Infectious TB
All patients with suspected or confirmed infectious
TB who are admitted to a health care facility should
immediately have appropriate isolation
precautions initiated(45-51). Policies
should designate who has the authority to initiate and
discontinue isolation precautions, to monitor
compliance with isolation procedures, and to manage
breaches in isolation precautions. These activities
will usually be performed by the infection control
personnel.
Some individuals with AFB-positive smears and
non-tuberculosis mycobacterial infection will be
placed under isolation precautions if an appropriate
level of suspicion is maintained. Isolation
precautions may be discontinued for these patients
once non-tuberculosis mycobacterial infection is
identified and infection with M. tuberculosis
is excluded. It is preferable to initially "over"
isolate than to delay implementing appropriate
isolation precautions.
Additional considerations
- Provision should be made for rapid transfer of
patients to another health care setting if adequate
isolation facilities are not available.
- Elective procedures should be postponed until the
patient is non-infectious.
- Isolation precautions should be continued even in
the face of negative AFB smears if there is a high
index of suspicion of active TB (i.e., the patient is
placed on anti-tuberculosis therapy). Individuals who
have a sputum smear that is AFB-negative but
culture-positive have been shown to transmit M.
tuberculosis to other people, although at a lower
rate than individuals who have a sputum smear that is
AFB-positive. Almost 50% of persons with active
pulmonary TB reported in Canada from 1990-1993 had
positive cultures for M. tuberculosis and negative
AFB smears(8).
-
Children with pulmonary TB are not usually as
infectious as adults because children do not
usually develop cavitary or sputum smear-positive
TB. However, since there is evidence that
children can transmit TB to
others(35), isolation of children with
suspected infectious TB is prudent.
- If uncertainty exists about isolation
precautions, consultation with an expert in infection
control or TB should be sought.
Isolation precautions for patients with
suspected or confirmed infectious TB receiving care in
ambulatory care areas or emergency rooms
The following isolation precautions should be
implemented:
- on arrival, place patients in designated waiting
areas in emergency rooms or clinics that have
appropriate engineering controls and are separated
from other patients (see Section IV.E); (high-risk
facilities should have one or more isolation rooms in
the emergency department available with appropriate
engineering controls.)
- whenever possible, book appointments at times to
minimize the exposure of other patients (e.g., the
end of the day);
- provide patients with surgical masks and give
instructions regarding their proper use (N.B.
Patients should never wear a mask containing an
expiratory valve);
-
educate patients and their visitors about
practices designed to reduce or eliminate
production of airborne droplet nuclei (e.g.,
covering mouth and nose with tissues when
coughing)(52); and
-
conduct the evaluation or procedure as
efficiently as possible (e.g., limit waiting
time).
Isolation precautions for individuals with
suspected or confirmed infectious TB undergoing
procedures either as ambulatory or admitted
patients
The following isolation precautions should be
implemented:
- ensure that procedures are performed in a
treatment or procedure room with appropriate
engineering controls (see Section IV.E); [this is
especially important when cough-inducing procedures
(e.g., sputum induction, aerosol treatments and
bronchoscopy) are being performed.]
- instruct patients to cover mouth and nose with
tissues when coughing or sneezing;
- ensure that only essential personnel are present
during the procedure;
- ensure that all persons present during the
procedure wear an appropriate mask (see Section
IV.F);
- ensure that people enter or leave the procedure
room during the procedure only if absolutely
necessary (keep the door to the procedure room closed
except when people are entering or leaving the room);
- ensure that patients remain in the procedure room
until coughing subsides, thereby limiting exposure of
other individuals who are in the general waiting or
recovery areas;
- allow adequate time between patient procedures so
the air will be free of droplet nuclei or place a
notice on the procedure room door advising HCWs who
must enter the room that appropriate masks should be
worn for a specified time (see Section IV.F) [the
required length of time is based on the number of air
changes and other engineering controls (see Section
IV.E), e.g., at six air changes per hour, 69 minutes
are required to remove 99.9% of airborne
contaminants(36) (see Appendix F)]; and
- perform procedures at the end of the schedule,
whenever possible.
Isolation precautions for patients with suspected
or confirmed infectious TB admitted to acute care
facilities
The following isolation precautions should be
implemented:
- place patient in single isolation room that has
the appropriate engineering controls (see Section
IV.E); (high-risk facilities should have one or more
isolation rooms available with appropriate
engineering controls. If more than one isolation room
is required for patients with TB, consideration
should be given to locating these rooms in a single
area of the health care facility. If the health care
facility does not have a room that meets these
criteria, a plan for managing this patient must
exist. High-risk facilities with intensive care units
should have at least one isolation intensive care
room with appropriate engineering controls.)
- ensure that the patient remains in the isolation
room; (the patient should only leave the room for
essential procedures. The patient should wear a mask
if he/she must leave the isolation room.)
- keep the door and window to the isolation room
closed except when individuals are entering or
exiting the room;
- limit the number of people entering the room;
(visitors should be restricted to members of the
patient's household. Visits by children under 12
should be limited because such children are highly
susceptible to infection with M.
tuberculosis.)
- ensure that all persons entering the room wear an
appropriate mask; (see Section IV.F) and
- instruct patients, visitors, and HCWs about the
importance of adhering to TB isolation precautions.
Isolation precautions for individuals with
suspected or confirmed infectious TB who are living
in long-term care facilities
Transmission of TB to both residents and HCWs has
been reported in long-term care
facilities(32,53,54). Residents of
long-term care facilities with newly diagnosed
infectious TB should be managed according to the same
policies and procedures as patients cared for in
acute care settings. Some long-term care settings may
have appropriate isolation facilities. If appropriate
isolation facilities are not available, transfer of
the resident to a health care facility equipped to
manage TB should be arranged as soon as possible.
There may be situations where transfer is delayed or
not possible. In such circumstances, the likelihood
of transmission of TB may be minimized by the
following:
- place the patient in a single room with the door
and window closed;
- ensure that all persons entering the room wear an
appropriate mask (see Section IV.F);
- initiate appropriate treatment;
- limit the number of people entering the room;
(visits by children under 12 should be avoided
because they are highly susceptible to infection with
M. tuberculosis);
- instruct HCWs, residents and visitors about the
importance of adhering to TB isolation precautions;
- initiate contact follow-up according to
established guidelines (see Section IV.D.7); and
- discontinue isolation only after the resident is
no longer infectious.
Discontinuation of isolation precautions
Isolation precautions should be continued until
patients are assessed to be non-infectious. A number
of variables influence the length of time an
individual remains infectious. These include the
level of infectivity (see Section III), the level of
competence of the patient's immune response, the
duration of, and adherence to, chemotherapy and the
presence or absence of drug-resistant TB.
Criteria for discontinuation of isolation precautions
should not be based on a fixed interval of treatment
(e.g., 2 weeks) but rather on evidence of clinical
and, if possible, bacteriologic improvement. Although
most individuals experience bacteriologic improvement
(e.g., smears of sputum specimens usually become AFB
negative) after receiving 2 weeks of appropriate
therapy, transmission of multidrug-resistant TB has
been reported in U.S. health care facilities from
patients where isolation precautions were
discontinued after a fixed time interval of 2 weeks
of therapy(1,3).
Although there are no definite criteria for
discontinuing TB isolation precautions, the following
are suggested as guidelines. Isolation may be
discontinued when:
- consecutive sputum smears are negative for AFB on
3 separate days;
AND
- there is evidence of clinical improvement;
AND
- there is reasonable evidence of adherence to the
medication regimen for a minimum of 2 weeks.
Isolation of patients with sputum smears that are
AFB-negative may be discontinued after 2 weeks of
therapy if they have responded to treatment and drug
resistance has not been identified on culture.
If a sputum is unobtainable (e.g., sputum
expectoration or gastric lavage), discontinuation of
isolation may be based on the following:
- level of infectivity (see Section III); and
- evidence of clinical improvement; and
- reasonable evidence of adherence to the
medication regimen for a minimum of 2 weeks; and
- assumed absence of drug-resistant TB.
Serious consideration should be given to
continuing isolation precautions for the duration of
the stay in the health care facility or until cultures
are negative, if a patient has pulmonary or laryngeal
MDR-TB. If the patient does not respond to treatment or
initially responds and then redevelops signs or
symptoms suggestive of active TB, re-assessment should
occur. Re-assessment should include investigation for
drug resistance. Isolation precautions should be
re-instituted. Patients who remain in the health care
facility for an extended length of time should be
periodically assessed to ensure that they do not
redevelop signs or symptoms that may be related to
their diagnosis of pulmonary or laryngeal TB.
3. Notification of Infection
Control Personnel
Personnel designated as responsible for the TB
management program (e.g., infection control
practitioner)should receive timely notification
whenever an individual with suspected or confirmed
infectious TB is receiving treatment in the health care
facility. This person will
- educate HCWs about the rationale for isolation
precautions;
- encourage patients' and HCWs' adherence to
isolation precautions;
- ensure that occupational health personnel are
notified so that contact follow-up of HCWs may be
initiated (see Section IV.D.7); and
- ensure that public health authorities are
notified so that contact follow-up of family,
emergency responders and visitors may be initiated
(see Section IV.D.6).
4. Confirmation of Diagnosis
The clinical diagnosis of active TB should be
supported by laboratory findings, whenever possible. A
suitable laboratory specimen should be obtained
promptly using the least invasive procedure. Specimens
should be sent for an AFB smear, as well as for culture
and sensitivity. Sensitivity results are necessary to
ensure treatment with appropriate antituberculous
therapy.
Laboratory specimens
-
For patients suspected of having pulmonary TB, a
deep-coughed specimen of sputum should be
obtained promptly. If this sputum specimen is
AFB-negative on smear, two successive early
morning sputum specimens should be obtained.
- For patients suspected of having extrapulmonary
TB, appropriate specimens should be obtained,
whenever possible, and sent for AFB staining, as well
as for culture and sensitivity. Tissue specimens
obtained for mycobacterial culture should be placed
in a container with saline for transport to the
laboratory.
- Blood cultures for mycobacterium species may also
be obtained using special mycobacteria media.
- Proper collection, handling and identification of
specimens should be ensured(42,43,55).
Laboratory results
- The laboratory should ensure that AFB smear
results, using either Ziehl-Neelsen or
rhodamine/auramine stains, are available within 48
hours of specimen collection.
- Radiometric detection methods (e.g., BACTECTM)
are highly reliable and take as little as 10 days
(mean 10 to 14 days) to detect the presence of
mycobacterial growth. Final identification requires a
further 1 to 2 days if a DNA probe is used or 4 to 5
days if the traditional NAP test is used. Drug
susceptibility testing may be initiated once growth
has been detected. Drug susceptibility results are
usually available 5 to 6 days later.
- Traditional culture methods require 6 to 8 weeks
to identify M. tuberculosis and another 6 to 8
weeks to determine the drug susceptibility
pattern(41,42,55,56).
5. Initiation of Treatment
Patients with confirmed TB or those in whom the
index of suspicion is high should be started promptly
on appropriate treatment after required specimens have
been obtained(9,43,57,58) (see Appendix D). Guidelines for the
initiation of treatment for TB, including suspected
MDR-TB, are detailed in other
documents(43,57). Individuals should be
observed while taking their antituberculosis
medications.
6. Notification of Public Health
Authorities
TB is a notifiable disease in all provinces and
territories. Each province or territory has a procedure
in place for the notification of public health
authorities regarding persons with confirmed active TB.
Provincial public health laws permit the restraint of
individuals with infectious TB in facilities with
appropriate isolation areas. For those in whom TB is
suspected, notification is determined according to
local jurisdictional practices. The confidentiality of
patient information must be maintained according to
provincial law and regulation (see Section IV.H).
The health care facility TB management program should
specify who is responsible for notifying the public
health authorities. This person should
- report any patient or HCW with confirmed TB to
ensure appropriate community contact investigation
and follow-up;
- report the results of species identification and
drug susceptibility testing as soon as they are
available; and
- ensure that a discharge plan is in place before
the patient is released to facilitate follow-up and
continuation of therapy; (the discharge plan should
ensure coordination between the health care facility,
local public health authorities and the physician
providing ongoing personal health care.)
7. Identification, Assessment and
Management of Contacts
An essential element of the TB management program
is the identification, assessment and management of
patients, visitors and HCWs who have been in contact
with individuals with infectious TB. Designated
personnel (e.g., infection control or occupational
health personnel) should perform the contact follow-up
activities for patients and HCWs within the health care
facility. Public health authorities should perform
these activities for contacts outside the health care
facility (e.g., visitors, family members). Public
health authorities should be aware of the results of
the contact investigation conducted within the health
care facility. All contacts who are assessed to have a
significant exposure to the individual with infectious
TB should receive education about TB transmission and
management and should be assessed as outlined below.
Identification of
contacts
The first step in contact follow-up is to interview
the patient and review his/her health record to
determine who may have been exposed to the patient
prior to the use of appropriate isolation
precautions. It is necessary to identify where the
patient has been in the facility and any individuals
who may have been in contact with the patient.
- The person with infectious TB may have been in
ambulances, patient units, emergency rooms,
outpatient clinics, operating rooms, recreational
areas, treatment and procedure rooms, and rooms for
radiologic and other diagnostic services.
- People who may have been in contact with the
person with infectious TB include those providing
direct care (e.g., nursing staff, physicians,
ambulance attendants, therapists) as well others
having direct contact with the patient (e.g., patient
room mates, pharmacy staff, laboratory personnel,
housekeeping staff, porters, social workers,
translators, volunteers, visitors). Depending on the
level of infectivity of the patient, subsequent
interviews may be required with personnel working
elsewhere in the health care facility to determine
the degree of exposure that may have taken place.
Assessment of contacts
The next step in follow-up is to evaluate the
significance of the exposure of those identified. The
significance of the exposure is determined by several
factors, including those associated with the patient
(relative infectivity), the environment, and the
susceptibility of the exposed person (see Section III).
- No contact follow-up is required if the
individual with infectious TB was placed in
appropriate isolation upon admission and subsequently
managed appropriately.
- There are no specific criteria to assess the
significance of the exposure because of the
variability in factors that determine the risk of TB
transmission. Therefore, one approach is to view the
potential for exposure as a series of concentric
circles with the infectious patient at the centre.
Contacts with the greatest potential for significant
exposure (e.g., persons who live in the same dwelling
plus relatives, friends or care givers who have
frequent, prolonged and close contact) are placed in
the ring closest to the patient. Other individuals
are placed in the outer circles depending on their
exposure. If a high level of TST conversion is found
in individuals in the circle closest to the patient,
the investigation is expanded, as required, to
contacts placed in the outer rings of the circle
until high levels of TST conversion are not found. In
the health care facility, primary nurses, for
example, who regularly cared for the patient and who
may be involved with cough-inducing procedures would
likely be at greatest risk. The significance of the
exposure would need to be assessed, however, in terms
of other factors, such as the adequacy of engineering
controls.
- Contacts of individuals who have an AFB-negative
smear, and who are culture positive must be
identified and contact follow-up performed following
the principles described in this section. Since the
infectivity level of these individuals is low,
significant exposure would only occur following
prolonged close contact.
a. For all contacts with a previously
documented negative TST or with an unknown TST
status but no past history of treatment for
active or inactive TB
- A post-exposure TST should be administered as
soon as possible (see Appendix B).
- Two-step testing should not be routinely
performed during post-exposure testing. Advise on
whether or not two-step testing should be performed
in a specific post-exposure situation can be obtained
from the local public health authorities or experts
in tuberculosis control.
- If the first post-exposure test is negative, a
TST should be repeated in 3 months since it takes up
to 3 months for the immune system to develop a
positive TST response following infection.
b. For contacts with a previously documented
positive TST or with a past history of treatment
for active or inactive TB
- It is not recommended to perform a TST.
- Conduct an interview to determine if symptoms of
TB are present.
- Provide education about the symptoms and signs of
active TB.
- Perform a chest radiograph immediately if the
person has symptoms of TB.
- Further clinical and radiologic re-evaluation
should take place in accordance with local
juristidational practice.
Management of contacts with a
documented TST conversion or symptoms suggestive of
active TB
- Such persons should be evaluated promptly, both
clinically and radiologically, for evidence of active
TB.
- Individuals who have a TST conversion and do not
have active TB should be offered preventive therapy
(see below and Appendix
C). These individuals do not need to be excluded
from work.
- Individuals who have active TB should undergo
further investigation and have appropriate treatment
initiated (see Appendix
D). These individuals should be excluded from
work until they are determined not to be infectious.
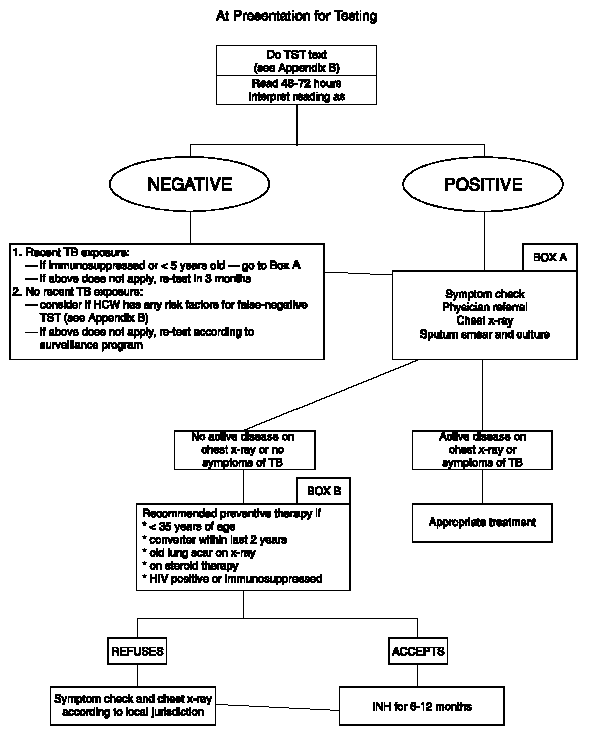
Provision of isoniazid (INH)
preventive therapy
Contact follow-up may identify HCWs and patients who
should be considered for INH preventive therapy (see
Appendix C and Figure 6). This should be offered in
accordance with local practice (e.g., by public health
authorities, the occupational health department or the
physician providing ongoing personal health care).
- All individuals considered for INH preventive
therapy should be informed about the risks of
developing TB, the rationale for accepting preventive
therapy, the need for appropriate monitoring (which
includes baseline liver function tests), and the
possibility of adverse drug reactions.
- The health records of patients or HCWs should
document whether preventive therapy was offered,
accepted and completed.
- HCWs who have documented TST conversions, whose
chest x-rays do not indicate active TB, and who
refuse INH preventive therapy or are unable to
tolerate INH preventive therapy, should be evaluated
clinically and radiologically in accordance with
local jurisdictional practice. These individuals do
not need to be excluded from work.
Ā
|