Common menu bar links
Institutional links
Diseases & Conditions
Health & Safety
Research & Statistics
Agency Information
Search Box
E-mail this page
Summary Report National Thematic Workshop on FASD
[Previous] [Table of Contents]
Appendices
Appendix 1: Agenda
Day One - March 29, 2005
| 8:15 | Continental Breakfast |
| 9:00 | Welcome and Introductions Agenda and Process |
| 9:30 | Opening Presentations
|
| 10:00 | The National Framework for Action on Substance Use and Abuse |
| 10:15 | Fetal Alcohol Spectrum Disorder (FASD): A Framework for Action |
| 10:30 | Refreshments |
| 10:45 | Small Discussion Groups |
| 11:45 | Insights from Discussion |
| 12:00 | Lunch (provided) |
| 1:00 | A National Tour of FASD |
| 2:15 | Refreshments |
| 2:30 | Small and Large Group Discussions (Linking FASD and the National Framework) |
| 3:45 | Group Reports |
| 4:15 | Summary of Day One |
| 4:30 | Adjourn |
Day Two - March 30, 2005
| 7:45 | Continental Breakfast |
| 8:30 | Debrief of Day One and Overview of Day Two |
| 8:45 | Small and Large Group Discussions (National FASD Priorities) |
| 10:00 | Refreshments |
| 10:20 | Group Reports |
| 11:45 | Insights from Discussion |
| 12:00 | Lunch |
| 1:00 | Action/Implementation Planning |
| 2:00 | Presentation of Action Plans |
| 2:45 | Next Steps |
| 3:00 | Wrap-Up and Closing Remarks |
| 3:15 | Adjourn |
Appendix 2: Invitation and Participant Lists
Invitees
| 1. Dr. Christine Loock | 2. Dr. Nicole LeBlanc |
| 3. Sterling K. Clarren | 4. Mary Cox-Millar |
| 5. Della Maguire | 6. Mark Schindel |
| 7. Darren Joslin | 8. Margaret Leslie |
| 9. Susan Santiago | 10. Louise Morin |
| 11. Dr. Jo Nanson | 12. Ms. Donna De Filippis |
| 13. Kim Meawasige | 14. Ms. Darlene Oakes |
| 15. Howard Collins | 16. Bill Ross |
| 17. Mr. Helie for Jan Westcott | 18. Jan Lutke |
| 19. Dr. Sarah Nikkel for Judith Allanson | 20. Michelle Dubik |
| 21. Deborah Kacki | 22. Dr. Lindsay Crowshoe |
| 23. Ms. Elizabeth Dawson | 24. Mr. Miguel LeBlanc |
| 25. Ms. Lona Hegeman | 26. Ms. Wendy Burgoyne |
| 27. Ms. Judy Pakozdy |
28. The Hon. Judge Mary Ellen Turpel Ladond |
| 29. Mrs. Dawn Ridd | 30. Dawn Bruyere |
| 31. NAHO | 32. Anne Fuller |
| 33. Ms. Nancy Poole | 34. Ms. Barbara Smith |
| 35. Ms. Donna Wheway | 36. Ms. Donna Debolt |
| 37. Ms. Audrey McFarlane | 38. Carol Parder for Ms. Laura Heal |
| 39. Ms. Ruth Morin | 40. Ms. Bonnie Buxton |
| 41. Diane Fox | 42. Eugenie Dore |
| 43. Dr. Françoise Bouchard | 44. Karen Palmer |
| 45. Colleen Ryan for Linda Dabros | 46. Robin Gearing |
| 47. Marie-Claude Paquette | 48. Dr. Lori Vital-Cox |
| 49. Patricia Blakely | 50. Lois Crossman |
| 51. Dr. Louise Nadeau | 52. Dr. James F. Brien |
| 53. Mary Johnston, PHAC | 54. Tammy Bambrick |
| 55. Isabelle Mélançon | 56. Diane Stefaniak |
Appendix 3: Workshop Background Paper
Key Findings on FASD and Alcohol Policy in Canada March 2005
Introduction
On March 29 and 30, 2005, the Canadian Centre on Substance Abuse (CCSA), in partnership with the Public Health Agency of Canada (PHAC), will host a National Thematic Workshop on Fetal Alcohol Spectrum Disorder (FASD). The objectives of the workshop are:
- to identify and to prioritize issues of national significance related to FASD
- to identify specific FASD work relevant to the development of the alcohol portion of the National Framework for Action on Substance Abuse
- to assemble and disseminate information that supports the ongoing consideration of important FASD issues
This paper is a summary of the status of key relevant FASD information regarding prevention, diagnosis, intervention/treatment and alcohol policy. Its intention is to stimulate and guide discussion over the course of the two-day workshop - it is not intended as a comprehensive literature review.
What Is FASD?
FASD is an umbrella term describing the range of effects that can occur in an individual whose mother drank alcohol during pregnancy. These effects may include physical, mental, behavioural and learning disabilities with lifelong implications. The term "FASD" is not intended for use as a clinical diagnosis (Chudley et al., 2005). The diagnoses under the FASD umbrella include fetal alcohol syndrome (FAS), partial-FAS, and alcohol-related neurodevelopmental disorder (ARND).
FASD is the leading cause of developmental and cognitive disabilities among Canadian children, (Health Canada, 1996; Canadian Pediatric Society, 2002) and has surpassed Down syndrome, spina bifida and cerebral palsy in estimated prevalence in the United States (Anon., 1983).
Effects of FASD
Human and animal studies have clearly demonstrated that alcohol is both a physical and a behavioural teratogen and that heavy prenatal alcohol exposure can lead to the distinct pattern of birth defects characteristic of fetal alcohol syndrome (Jones et al., 1973; Randall and Taylor, 1979; Randall and Riley, 1981). Neurobehavioural effects associated with pFAS and ARND are just as debilitating as those characteristic of FAS (Mattson et al., 1997; Mattson and Riley, 1999). Thus, the consequences of FASD include irreversible, lifelong disabilities that affect physical, cognitive, social and behavioural development. A recent study concluded that the impact of FASD on the affected individual's health related to quality of life (HRQoL) is profound (Stade, 2003).
Individual, family and community impacts of FASD are dynamic. For example, research suggests that as children with FASD reach adolescence, their social and behavioural problems increase (Olson et al., 1997; Streissguth et al., 1991). Adolescents with FASD have been shown to have increased rates of mental illness, substance abuse and school failure, as well as early and repeated trouble with the law (Fast et al., 1999; Fast and Conry, 2004). Adults with FASD suffer from a range of psycho-social problems that increase the likelihood of confinement in detention, jail, prison, or a psychiatric or alcohol/drug inpatient setting (Streissguth et al., 2004).
Fortunately, appropriate intervention has been shown to mitigate the onset of secondary disabilities (i.e. those not attributed directly to the physical and neurobehavioural damage of FASD), including depression and conduct disorders, disrupted school experience, inappropriate sexual behaviour, alcohol and drug problems, dependent living, and problems with employment and the law (Streissguth et al., 1997). Expert researchers in the field (Streissguth et al., 1997; Streissguth, 1997; Streissguth and Kanter, 1997; Astley and Clarren, 1999) have called for early diagnosis and prompt intervention with families of alcohol-affected children to promote the development of these children and to minimize the occurrence of secondary disabilities.
FASD and its related secondary disabilities exert a significant impact on Canada's economy. Individuals affected by prenatal exposure to alcohol often require specialized education, mental health attention, care and facilities throughout their lifetime and tend to overutilize systems and services (Loney et al., 1998). In addition, the many secondary disabilities that arise impact their ability to live independently, function according to societal norms and remain gainfully employed. Thus, the economic cost of FASD is significant.
Economic Cost of FASD
Researchers in the United States have estimated that the lifetime direct health care costs for an individual with FAS are approximately $1.4 million (Lupton et al., 2004). Canadian research has estimated annual adjusted costs associated with FASD at the individual level to be $14,342 (Stade, 2003). These costs include those incurred by the health care system related to health service utilization and direct out-of-pocket expenses incurred by the biological, adoptive and foster parents. The additional lifetime costs (from age 0-65) for affected individuals were estimated at just under $850,000. This estimate does not include indirect costs (including those related to the correctional or justice system) or opportunity costs (such as lost potential or productivity).
At an estimated cost of $14,342/individual/year, FASD is more than 10 times as expensive as childhood asthma, estimated at $1,400/patient/year (Ungar and Coyte, 2001).
Maternal Alcohol Use
In general, most outcome measures for alcohol use and abuse have increased in Canada in recent years, with exceptions being around alcohol consumption during pregnancy and drinking and driving.
Women were asked about alcohol consumption during pregnancy and during breastfeeding in the Canadian Community Health Survey (cycle 2.1) 2003. Figure 1 illustrates the data from women who had been pregnant in the last 5 years, but unfortunately these data do not report on the amount consumed during each of these drinking sessions.
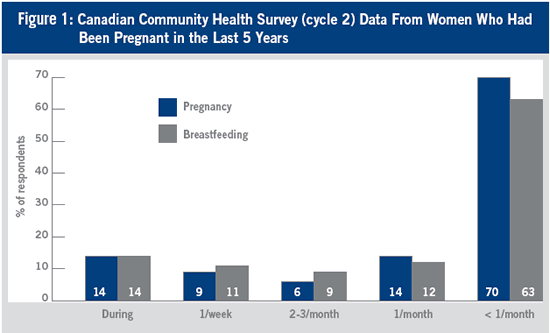
Canada's National Longitudinal Surveys of Children and Youth, conducted in 1994-1995 and repeated again in 1998-1999, asked respondents to report on their alcohol consumption during pregnancy. The number of Canadian women who report drinking alcohol at some point during their pregnancy has decreased from 17% to 25% in a 1994-1995 survey (National Longitudinal Survey of Children and Youth (Statistics Canada, 1995) to 14.4% in 1998-1999 (Statistics Canada, 1999). In the same surveys, 7% to 9% of respondents reported drinking throughout their pregnancy in 1994-1995 and 4.9% reported the same in 1998-1999. Incidentally, in the later survey 3% reported binge drinking during pregnancy.
The most recent data from the Canadian Addiction Survey (CAS) released on March 23, 2005 suggest that the rate of past-year drinking (any amount of alcohol consumed) among females was 76.8%. Nearly 33% of females reported drinking at least once a week. The survey did not address drinking during pregnancy (Canadian Centre on Substance Abuse, 2005).
Adolescent drinking is also of concern since teenaged girls are of childbearing age. The Health Behaviours in School Aged Children Survey 2000/01 shows that 23% of Grade 10 girls reported that they had an alcoholic drink at least once a week. This rate increased steadily from 3% at Grade 6 to 11% at Grade 8 to 18% at Grade 9. Forty-two percent of Grade 10 girls said they had been drunk at least twice. While variable, the same study shows that the majority of students first tried alcohol between the ages of 12 and 14 and first got drunk between the ages of 13 and 15. The trends in these data seem to be going in the inverse direction to the tobacco use data for Canada.
Risk Factors
The severity of the effects of prenatal alcohol exposure depends on interactions between maternal and fetal physiology and genetics, timing and duration of fetal exposure, pattern of maternal drinking, and a number of maternal lifestyle factors, including higher maternal age, lower education level, cocaine use, smoking, custody changes, lower socio-economic status, and paternal drinking and drug use at the time of pregnancy (Sood et al., 2001), as well as reduced access to pre- and postnatal care and services, inadequate nutrition and a poor developmental environment (e.g. stress, abuse, neglect) (Bingol et al., 1987).
Defining the Scope of the Problem
Prevalence estimates of FASD vary widely (Roberts and Nanson, 2000). The prevalence of FAS in the United States has been estimated to be 0.5 to 2 cases per 1,000 live births and FASD as 9.1 cases per 1000 live births (Sampson et al., 1994).
In Canada, a few small studies have estimated prevalence of FASD in sub-populations. One study conducted in an isolated community in British Columbia reported FAS rates of 190 per 1,000 live births (Robinson et al., 1987), while another conducted in a First Nations community in Manitoba reported rates between 55 and101 per 1,000 (Square, 1997). Other surveys conducted in Yukon and northern British Columbia estimated the rate of FAS and related effects as 46 per 1,000 and 25 per 1,000 respectively (Asante and Nelms- Maztke, 1985). It is important to note, however, that these estimates are specific to these communities and cannot be extrapolated to apply to the Canadian population as a whole. The rate used as an estimate of national prevalence rate of FASD in Canada is 9.1 per 1,000 live births, based upon Sampson's data from Seattle (Sampson et al., 1994).
Addressing the Problem Prevention in Canada
There are three levels of prevention - primary, secondary and tertiary. Primary prevention targets the entire population and includes public awareness campaigns, community education and alcohol control measures. Secondary prevention specifically targets at-risk populations and can include outreach, screening and referral for women who are pregnant, or of childbearing age, and using substances. Tertiary prevention targets those for whom FASD is already a concern, such as women who are at risk of having a child affected by prenatal substance use, or women who have already given birth to a child with FASD (Roberts and Nanson, 2000).
Primary Prevention
There are two key national resources on FASD. The first is the CCSA's FASD Information and Consultation Service, which provides links to support groups, prevention projects, resource centres and experts on FASD.
The second is the toll-free bilingual Motherisk Alcohol and Substance Use Helpline (1-877-FAS-INFO) that provides information and counselling to pregnant and breastfeeding women, their families and health care providers on the effects of alcohol use and other substances during pregnancy and lactation; referrals to services in the caller's home community; and referrals to FASD assessment at The Hospital for Sick Children in Toronto.
At the provincial/territorial and community levels, primary prevention ranges from large, multifaceted campaigns to very basic awareness efforts. The Canadian provinces and territories are at different stages of primary prevention programs, services and campaigns, and all recognize the importance of FASD prevention.
There is a growing body of research specific to primary prevention and the public awareness of the risks of drinking alcohol during pregnancy. An Environics survey of Ontario women of childbearing age in July 2004 determined that there are high levels of awareness that alcohol use in pregnancy leads to lifelong consequences. A national survey in 2000 showed similarly high levels of general awareness (Environics, 2000). Awareness breaks down around more specific issues, such as the amount that may be "safe" to drink in pregnancy and when to stop drinking (Best Start, 2004).
Other research has sought to establish a link between awareness activities and behaviour. Efforts that take a single approach, such as signs or warning labels, have shown mixed results and limited impact (Health Canada, 2000; Caprara et al., 2004), while multilevel campaigns that include media, workshops, public events and links to additional services are more effective (THCU, 1999). Cumulative exposure to health messages has also been found to have effect (Kaskutas and Graves, 1994).
Numerous resources have been developed to provide guidance on where to start, what works, guiding values, building partnerships, understanding the audience, defining the message, and evaluating the impact of a prevention campaign (Roberts and Nanson, 2000; BC FAS Resource Society, 2004). Organizations such as Ontario's Best Start have sought to define effective communication messaging about alcohol and pregnancy, based on the evaluation of its 2004 alcohol and pregnancy campaign in Ontario (Best Start: Evaluation 2004).
Most recently, the Alberta Centre for Child, Family, and Community Research funded a state of the evidence review on FASD prevention. The report should be available on its Web site in spring 2005 (http://www.research4children.com).
Secondary and Tertiary Prevention
Secondary and tertiary prevention efforts have been developed based upon the evaluation of community-based prenatal and early childhood projects (including Community Action Program for Children, Canadian Prenatal Nutrition Program, Aboriginal Head Start, Early Childhood Development Initiative) and women-centred research aimed at identifying noncoercive ways to reach and support pregnant women who use alcohol and other substances (Poole, 2000; Pepler et al., 2002).
Research and help guides have focused on the barriers to access, such as homelessness and the effects of early engagement of pregnant women using substances (Hicks, 1997); identification and support of children and families affected by prenatal alcohol exposure (Leslie and Roberts, 2004); barriers to treatment, such as the fear of apprehension, for substance-use mothers (Poole and Isaac, 2001); effects of homelessness on women's health (Kappel Ramji Consulting Group, 2002); and applied strategies to support pregnant women with substance use problems (Leslie and Reynolds, 2002; AADAC 2003).
Researchers have also considered the role of the physician in screening for alcohol use during pregnancy and have found varying attitudes and approaches to preconception counselling (Tough et al., 2005), as well as varying levels of awareness and ability to provide FAS diagnosis (Sarkar, 2003).
Many workshops, conferences, teleconferences and training manuals have been developed for physicians and front-line workers (e.g. CCSA FAS Tool Kit; Motherisk and Best Start physician training; Breaking the Cycle/CCSA Nurturing Change). Also, new ways to transfer knowledge (e.g. Web-based information) have been tested through projects such as the "Demonstration Project to Provide On-Line Training and Consultation on Evidence-Based Practices for Front-Line Practitioners in Health Canada's CAPC/CPNP Network" (2002). What emerges from this cursory review is a patchwork of intermittent prevention activities throughout Canada. At one end of the spectrum are single-message prevention activities and products; at the other end are a few coordinated multilevel campaigns. At best, prevention activities to date have aimed at promoting healthy choices in pregnancy to achieve healthy birth outcomes. At worst, prevention messaging has oversimplified the problem by suggesting that any woman can "just say no," "FASD is 100% preventable" or that "any amount of alcohol during pregnancy will cause FAS."
Growing evidence suggests, however, that FASD prevention requires integrated programs that deliver culturally sensitive perinatal services to high-risk women, neonatal screening, and prompt and sustained intervention for affected children and mothers. Furthermore, these programs should be based on an understanding of the determinants of health and factors that contribute to alcohol use in pregnancy and addiction. It would also be desirable to gather Canadian data on risk factors so that appropriately targeted programs and services can be developed.
The Diagnostic Process
Early diagnosis of FAS, pFAS and ARND is the crucial first step in the timely delivery of effective intervention. In fact, diagnosis before age 6 is recognized as a major factor in preventing the onset of secondary disabilities (Astley and Clarren, 1999). Also, diagnosis in early childhood may "serve as a clinical biomarker for unrecognized maternal mental health and addiction concerns and provide an opportunity to offer interventions, support and counseling for the birth mother." It may also prompt interventions for other affected siblings and help to prevent alcohol exposure during subsequent pregnancies (Loock et al., 2005). In effect then, early diagnosis identifies two patients (baby and mother) and possibly more (siblings and partners).
Diagnosis extends beyond physical examination, and the diagnostic procedure is complex and labour-intensive. A diagnosis is not a label, but rather a blueprint for intervention and prevention. As stated in the recently released Canadian Guidelines for diagnosis, "the diagnostic process consists of screening and referral, the physical examination and differential diagnosis, the neurobehavioural assessment and treatment, and follow-up" (Chudley et al., 2005). This is accomplished through the coordinated efforts of a multidisciplinary team of health and allied health experts.
Comprehensive, age-appropriate neurobehavioural assessment consists of standardized measures of intelligence, language, memory, attention, executive functioning, sensorimotor, visuospatial and social/emotional functioning. Time must also be spent with parents or guardians to discuss the results of the assessment and to share information regarding appropriate resources in their community, based on a report summarizing the test results, the diagnosis and specific recommendations for home and school. Ideally, the diagnostic process should also include pre- and post-assessment counselling and support to the mother and child (Chudley et al., 2005). As women learn more about the risks of prenatal alcohol use in relation to their own children, they may become aware that they experience many symptoms consistent with FASD (Rouleau et al., 2003). Adult FASD assessment of these women may help to promote renewed hope among those who always knew "something was wrong" but were unable to identify the nature and cause of their disability. Clearly, setting standards for diagnosis also leads to questions. For example:
- Who will deliver this basket of specialized diagnostic services and supports?
- How can capacity be built to ensure that services are accessed in urban as well as rural areas throughout Canada?
- If pre- and post-counselling and support are important parts of the diagnostic process, what service models are best and how are they to be funded?
- How does the process need to be adapted to address special populations and contexts (i.e. rurality, culture)?
Intervention
As discussed above, intervention is an important element of tertiary prevention. It is also an element of the diagnostic process that calls for treatment and follow-up. FASD management requires a seamless and comprehensive assessment-diagnosis-intervention-support continuum for both the mother and the child.
Interventions for persons affected by prenatal substance use seek to prevent and reduce harmful effects associated with the primary and secondary disabilities of FASD (Roberts and Nanson, 2000). Effective intervention aims at promoting the development of affected individuals throughout the stages of life, and supporting those caring for them. Those charged with their care will have to face a multiplicity of issues, including appropriate medical care, educational and vocational supports, social problems associated with the affected individual's impulsivity, poor judgment and decision-making skills, and interactions with the law and criminal justice system.
Much of what is known about effective interventions has been gained through the experiences of biological, adoptive and foster parents who are raising affected children, and community workers who have been meeting the challenge of FASD management one issue (or crisis) at a time. Recognizing that so many children and adolescents with FASD are living in foster care, case managers are learning that the best case scenario is diagnosis by age 6, stable placement in a family that is trained to help the child over each developmental hurdle and supported with respite, and that the child is placed in a school program that understands and supports the primary disabilities of FASD. But the task is far from easy. Appropriate service planning requires the development of case management standards, shared information and reconciling often competing mandates and demands of agencies charged with child safety, community safety and family preservation.
A topic of much discussion relates to FASD and intervention within the criminal justice system and the appropriateness of incarceration for FASD-affected individuals. Does the justice system have the capacity to ensure that these individuals are treated properly? And if not, what judicial or extra-judicial options exist (UBC, 2005)? Others within the criminal justice system have taken steps to incorporate First Nations practices and values into the mainstream legal system (Turpel-Lafond, 2004). This paper cannot begin to enumerate the many efforts of individuals and groups nationwide to grasp at least a piece of the problem and implement workable solutions, but much valuable work is being done. Comprehensive, lifelong intervention requires leadership and coordination of FASD initiatives at the community, regional, provincial/territorial and national levels. A number of provincial/territorial and federal priorities have been identified related to family supports, education, funding and research.
Current issues related to intervention include:
- What are appropriate ways to deliver culturally sensitive services and support (Masotti et al., 2003)?
- How can barriers to access be overcome for Aboriginal women and families?
Research
Canada has leading researchers in the field of FASD. Research focuses on mechanisms underlying neurobehavioural development, prevention in Aboriginal communities, biomarkers for screening pregnant women for alcohol use, effective interventions and antioxidant therapy to prevent disabilities associated with prenatal alcohol exposure.
Policy and Prevention
There is considerable debate concerning effective alcohol policy. Some researchers recommend policies that lower overall alcohol consumption, in the belief that information and education campaigns have little if any impact on drinking rates or damage from alcohol use (Giesbrecht, 2003). Others propose that policy should be aimed at reducing problem drinking (Grant and Litvak, 1997).
In Canada, a variety of regulatory measures have been implemented to decrease alcohol consumption, in general. These include increased taxation, government monopoly of retail sales, minimum purchase age and limiting hours of service. The measure shown to be most effective to date is increased pricing through taxation. Other policies have been adopted at the municipal and provincial levels, to varying effect (Roberts and Nanson, 2000). Some provinces and territories require warnings about the dangers of alcohol consumption during pregnancy to be printed on liquor store bags and receipts. Sandy's Law has gained recent press. It requires the placement of signs that warns about the effects of alcohol use during pregnancy in places where liquor is sold in Ontario.
At the federal level, Bill C-206 requiring the application of warning labels on alcoholic beverages is currently being debated in the House. The purpose of Bill C-206 is to require alcoholic beverages to bear a warning regarding the effects of alcohol on the ability to operate vehicles and machinery and on the health of consumers, and the possibility of birth defects when consumed during pregnancy. As with so many issues related to policy and prevention, there are strong opinions for and against the effectiveness and utility of warning labels (Babor et al., 2003).
Effective FASD-related policies will require partnership, cooperation and communication among provincial and territorial governments, the federal government and private stakeholders. The following guidelines for alcohol policy development have been recommended by Edwards et al. (1994).
- There is no one policy panacea. The effective policies will be a mix.
- Some policy measures are more effective than others. The basic, evidencebased policy mix includes taxation, control of physical access, drinking-driving countermeasures and treatment - particularly primary care. Educational strategies, restrictions on advertising and community action programs are additional measures with the potential for long-term pay-off.
- Political feasibility and public acceptance are important in selecting alcohol policies.
- Policy choices have national and international dimensions.
- Policy choices have to be determined not only by what is effective, but by what provide value for money.
A number of principles and criteria for effective policy were discussed at the Roundtable on Alcohol Policy, hosted by CCSA on November 18 and 19, 2004. Roundtable participants noted that effective policy:
- generates buy-in
- can adapt to different communities
- reflects community needs and is driven by community
The group recommended that a national Centre for Excellence on FASD be created and selected five policy areas for further discussion and exploration:
- promoting the use of brief intervention
- developing and promoting policies to reduce chronic disease
- addressing drinking context and use of targeted intervention
- structuring alcohol taxes in a discerning and purposeful manner
- developing the culture of moderation vs. a culture of intoxication (i.e. a culture of healthy lifestyles) (CCSA, Draft Key Messages Report, 2005)
Policy and Treatment
Pregnant substance-using women have been profoundly impacted by alcohol and drugrelated policies and sanctions (Roberts and Nanson, 2000). Aside from neglect and inadequate service delivery (e.g. services for pregnant women based on treatment models for men and failure to provide child care for women seeking treatment), pregnant substance-using women have faced coercive civil and criminal sanctions. In Canada, the case of Ms. G. highlighted the issue of mandatory treatment for pregnant substance-using women, while in the United States, prosecutors in various states are charging women who use alcohol and other drugs while pregnant with serious crimes, such as misdemeanor counts of endangering the welfare of a child and homicide.
In Canada, the court ruled against mandatory treatment of pregnant women. Still, there is a need for comprehensive treatments and services that respect the rights of women, while also preventing FASD. Examples such as the Sheway Program in Vancouver and Breaking the Cycle in Toronto illustrate that effective solutions require collaboration among those charged with child welfare and protection, health care provision for mother and child, women's addiction services, counselling, family planning, housing and other services (Pepler et al., 2002; Poole, 2003). The challenge is to continue to enhance these existing models, duplicate them and ensure that they are sustained through adequate funding and support.
Two National Frameworks for Action
In 2003, Health Canada introduced the Framework for Action on FASD. Developed through consultation with hundreds of organizations and individuals across Canada, the FASD Framework lays out a vision for the future, five broad goals, strategies and guiding principles.
The Framework for Action on FASD recognizes that individual and collaborative action is required in all sectors, at all levels - federal, provincial, territorial and community. The five broad goals calling for action are:
- Increase public and professional awareness and understanding of FASD and the impact of alcohol use during pregnancy.
- Develop and increase capacity.
- Create effective national screening, diagnostic and data-reporting tools and approaches.
- Expand the knowledge base and facilitate information exchange.
- Increase commitment and support for action on FASD.
Meanwhile, Health Canada and CCSA are engaged in a broad consultation on a proposed National Framework for Action on Substance Use and Abuse. The initial goal is "to determine the level of commitment across Canada to developing such a Framework." A comprehensive process is underway to involve stakeholders in the development of the Framework. To date, several regional consultations have been held, along with thematic workshops. A biennial forum that will introduce a draft National Framework will follow, and finally a National Addictions Conference will occur in late 2005 to also inform the Framework. Likewise, a series of reports and studies will provide key information about:
- substance use in the Canadian population
- culturally appropriate surveys in each of Canada's territories that complement the Canadian Addictions Survey
- education and training needs of treatment professionals
- data on the health and economic well-being of Canadians
Summary and Questions to Consider
Given the impact of FASD on individuals, families, communities and the Canadian economy, the state of prevention and intervention efforts in Canada, the current debates over alcohol policy development and the persistent lack of funding for FASD-related efforts, it may be helpful to integrate FASD-related issues into a broader alcohol framework. Thus:
- How should the Framework for Action on FASD and the National Framework for Action on Substance Use and Abuse be linked?
- Which FASD-related themes would best link?
- How would integration of FASD into the National Framework for Action on Substance Use and Abuse be most effectively conducted?
- What would be the benefits of a coordinated effort?
- Who would be the necessary partners and how would the partnerships be developed?
- Where would funding come from?
- Would there be jurisdictional barriers (i.e. provincial/territorial vs. federal)
- That would have to be overcome?
- What would be the draft FASD strategy?
- What would be the draft action plan?
- What might be the consequences of proceeding with a National Framework on Substance Use and Abuse that does not include a FASD component?
- Is there a risk of confusion, duplication of effort, competing priorities?
It is expected that answers to these questions, as well as others, will determine the best use of efforts and resources to improve outcomes for FASD-affected individuals and families in the long run.
Sources
- Alberta Alcohol and Drug Abuse Commission. (2003). Help
guide for professionals
working with women who use substances: Screening, intervention, referral. Edmonton:
Author. Available at http://www.aadac.com/ - Asante K.O., & Nelms-Maztke, J. (1985). Report on the
survey of children with
chronic handicaps and fetal alcohol syndrome in the Yukon and Northwest British
Columbia. Whitehorse: Council for Yukon Indians. - Astley, S.J., & Clarren, S.K. (1999). Diagnostic guide
for fetal alcohol syndrome (FAS)
and related conditions: The 4-digit diagnostic code. Seattle: University of Washington. - Babor T. et al. (2003). Alcohol: No ordinary commodity.
Research and public policy.
New York: Oxford University Press. - Best Start. (2002). Preventing and addressing alcohol use
in pregnancy (physician
training). Available at www.beststart.org/resources/alc_reduction/pdf/community_planning_guide.pdf. - Best Start. (2003). Keys to a successful alcohol and
pregnancy communications
campaign 2003. Retrieved 17 March 2005 from
http://www.beststart.org/resources/alc_reduction/pdf/keys.pdf. - Best Start. (2004). Ontario's Provincial Alcohol and
Pregnancy Campaign - Be Safe:
Have an alcohol-free pregnancy. Retrieved May 2004 from
www.ohpe.ca/index2.php?option=com_content&do_pdf=1&id=247l. - Best Start. (2004). Best Start Alcohol and Pregnancy
Campaign - Evaluation results.
Available at http://www.beststart.org/apcampaign/results.htm. - Bingol, N., Schuster, C., Fuchs, M., Losub, S., Turner, G.,
Stone, R.K. et al. (1987).
The influence of socioeconomic factors on the occurrence of fetal alcohol syndrome.
Advancements in Alcohol Substance Abuse, 6(4),105-118. - Breaking the Cycle, & CCSA. (2004). Nurturing change:
Working effectively with high risk
women and children to prevent and reduce harms associated with FASD. Available at
http://www.mothercraft.ca/database/projects_publications/Nurturing%20Change%20Final-
GR1.pdf. - British Columbia FAS Resource Society. (1998). Community
action guide.
- Canadian Centre on Substance Abuse. (2002). FAS tool
kit. Available at
http://www.ccsa.ca/toolkit/Introduction.htm - Canadian Centre on Substance Abuse. (2001). Enhancing fetal
alcohol syndrome
(FAS)-related Interventions at the prenatal and early childhood stages in Canada.
Available at http://www.ccsa.ca - Canadian Centre on Substance Abuse. (2005). Draft key
messages report.
Roundtable on alcohol policy. Hosted by the CCSA, Ottawa, 18-19 November 2004. - Canadian Centre on Substance Use. (2005). Canadian
Addiction Survey: A national
survey of Canadians' use of alcohol and other drugs: Prevalence of use and related
harms. Available at http://www.ccsa.ca/pdf/ccsa-004028-2005.pdf. - Canadian Paediatric Society (CPS) Statement. (2002). Fetal
alcohol syndrome.
Paediatric Child Health, 7(3), 161-174. - Caprara, D., Soldin, O., & Koren, G. (2004) To label or not
to label: The pros and cons
of alcohol warning labels in pregnancy. Journal of FAS International, 2, e9. Available at
http://www.motherisk.org/JFAS/detail.php?id=62. - Chudley, A., Conry, J., Cook, J., Loock, C., Rosales, T., &
LeBlanc, N. (2005). Fetal
alcohol spectrum disorder: Canadian guidelines for diagnosis. Canadian Medical
Association Journal, 172(5 Suppl.). Available from
http://www.cmaj.ca/cgi/content/abstract/172/5_suppl/S1?maxtoshow=&HITS=10&hits=
10&RESULTFORMAT=&fulltext=FASD&andorexactfulltext=and&searchid=1110923392
465_1548&stored_search=&FIRSTINDEX=0&sortspec=relevance&resourcetype=1&jo
urnalcode=cmaj. - Clark, E., Lutke, J., Minnes, P., & Ouellette-Kuntz, H.
(2004). Secondary disabilities
among adults with fetal alcohol spectrum disorder in British Columbia. Journal of FAS
International, 2, e13. Available at http://www.motherisk.org/JFAS/detail.php?id=66 - Cohen-Kerem, R., & Koren, G. (2003). Antioxidants and fetal
protection against
ethanol teratogenicity. I. Review of the experimental data and implications to humans.
Neurotoxicogy and Teratology, Jan-Feb, 25(1), 1-9. - Edwards, G. et al. (2002). Alcohol policy and the public good,
p. 211. WHO Europe.
Oxford: Oxford Medical Publications. Quoted in: Kendal, P. (2002). Public health
approach to alcohol policy: A report of the provincial health officer. Victoria, BC: BC
Ministry of Health Planning. - Environics Research Group Limited. (2000). Awareness of the
effects of alcohol use
during pregnancy and fetal alcohol syndrome: Results of a national survey. Final
report. Prepared for Health Canada. - FACE. (2004). Panel Discussion - 4th Annual Research Roundtable
(2004). Question
of ethics: Neonatal screening for prenatal alcohol exposure. Webcast available at
http://www.motherisk.org/JFAS/detail.php?id=67. - Fast, D.K., Conry, J., & Loock, C.A. (1999). Identifying
fetal alcohol syndrome among
youth in the criminal justice system. Journal of Developmental and Behavioral
Pediatrics, 20(5), 370-372. - Fast, D.K., & Conry, J. (2004). The challenge of fetal
alcohol syndrome in the criminal
legal system. Addiction Biology, 9(2),161-166; discussion 167-168. - Giesbrecht, N. (2003). Rising per capital alcohol consumption
and drinking-related
harm: Suggestions for meeting the challenge. The Globe, (4). Available at
http://www.ias.org.uk/resources/publications/theglobe/globe200304/gl200304_p7.html. - Grant, M., & Litvak, J. (Eds.). (1997). Drinking
patterns and their consequences. New
York: Taylor and Francis. Kendal, P. (2002). Public health approach to alcohol policy:
A report of the provincial health officer. Victoria, BC: BC Ministry of Health Planning. - Health Canada. (1996). Joint statement: Prevention of fetal
alcohol syndrome (FAS),
fetal alcohol effects (FAE) in Canada. Ottawa: Author. - Hicks, L. (1997). Drug addiction and pregnant/parenting
women: Factors affecting
client engagement. Toronto: Breaking the Cycle and University of Toronto. - Jing, H., & Li, Y. (2004). Effects of ethanol on mouse
embryonic brain development
and heat shock protein 73 expression. Toxicology in Vitro, 18(5), 601-607. - Jones, K.L., & Smith, D.W. (1973). Recognition of the fetal
alcohol syndrome in early
infancy. Lancet, 2(836), 999-1001. - Jones, K.L., Smith, D.W. et al. (1973). Pattern of malformation
in offspring of chronic
alcoholic mothers. Lancet, 1(815), 1267-1271. - Kappel Ramji Consulting Group. (2002). Common occurrence:
The impact of
homelessness on women's health. Phase II: Community based action research -
Final report. Toronto: Sistering. - Kaskutas, L.A., & Graves, K. (1994). Relationship between
cumulative exposure to
health messages and awareness and behavior-related drinking during pregnancy.
American Journal of Health Promotion, 9(2), 115-124. - Leslie, M., & Reynolds, W. (2002). The SMART guide:
Motivational approaches within
the stages of change for pregnant women who use alcohol: A training manual for
service providers. Kingston, Ont.: Action on Women's Addictions Research and
Education (AWARE) and Breaking the Cycle. - Leslie, M., & Roberts, G. (2004). Nurturing change:
Working effectively with high-risk
women and children to prevent and reduce harms associated with FASD. Available at
http://www.ccsa.ca - Loney, E., Habbick, B. et al. (1998). Hospital utilization of
Saskatchewan people with
fetal alcohol syndrome. Canadian Journal of Public Health, 89(5), 333-336. - Loock C., Conry, J., Cook, J., Chudley, A., & Rosales, T.
(2005). Identifying fetal alcohol
spectrum disorder in primary care. Canadian Medical Association Journal, 172(5).
Retrieved 15 March 2005 from http://www.cmaj.ca/cgi/content/full/172/5/628?etoc - Lupton, C., Burd, L., & Harwood, R. (2004). Cost of fetal
alcohol spectrum disorders.
American Journal of Medical Genetics, 127 C(1), 42-50. - Masotti, P. et al. (2003). Urban FASD interventions: Bridging
the cultural gap.
Journal of FAS International, 1: e17. Available at
http://www.motherisk.org/JFAS/details.php?id=45 - Mattson, S.N., Riley, E.P. et al. (1997). Heavy prenatal
alcohol exposure with or
without physical features of fetal alcohol syndrome leads to IQ deficits. Journal of
Pediatrics, 131(5), 718-721. - Mattson, S.N., & Riley, E.P. (1999). Implicit and explicit
memory functioning in
children with heavy prenatal alcohol exposure. Journal of the International
Neuropsychological Society, 5(5), 462-471. - Anon. (1983). Leading major congenital malformations among
minority groups in the
United States. Morbidity and Mortality Weekly Report, (37), 17-24. - Olson, H.C., Streissguth, A.P., Sampson, P.D., Barr, H.M.,
Bookstein, F.L., & Thiede,
K. (1997). Association of prenatal alcohol exposure with behavioral and learning
problems in early adolescence. Journal of the American Academy of Child and
Adolescent Psychiatry, 36(9),1187-1194. - Pepler, D.J., Moore, T.E., Motz, M.H., & Leslie, M. (2002).
Breaking the cycle:
The evaluation report (1995-2000). Toronto: Health Canada. - Poole, N., & Isaac, B. (2001). Apprehensions: Barriers
to treatment for substanceusing
mothers. Vancouver: BC Centre of Excellence for Women's Health. Available at
http://www.bccewh.bc.ca/ - Poole, N. (2000). Evaluation report of the Sheway Project
for high-risk pregnant and
parenting women. Vancouver: BC Centre of Excellence for Women's Health. Available
at http://www.bccewh.bc.ca/ - Poole, N. (2003). Mother and child reunion: Preventing
fetal alcohol spectrum
disorder by promoting women's health. Vancouver: British Columbia Centre of
Excellence for Women's Health. Available at http://www.bccewh.bc.ca/publications-resources/documents/motherchildreunion.pdf. - Randall, C.L., & Taylor, W.J. (1979). Prenatal ethanol
exposure in mice: Teratogenic
effects. Teratology, 19(3), 305-311. - Randall, C.L., & Riley, E.P. (1981). Prenatal alcohol
exposure: Current issues and the
status of animal research. Neurobehavioral Toxicology and Teratology, 3(2), 111-115. - Roberts, G., & Nanson, J. (2000). Best practices: Fetal
alcohol syndrome/fetal alcohol
effects and the effects of other substance use during pregnancy. Ottawa: Health
Canada, Canada's Drug Strategy Division. - Robinson, G.C., Conry, J.L., & Conry, R.F. (1987). Clinical
profile and prevalence of
fetal alcohol syndrome in an isolated community in British Columbia. Canadian
Medical Association Journal, 137(3), 203-207. - Rouleau, M., Levichek, Z., & Koren, G. (2003). Are mothers
who drink heavily in
pregnancy victims of FAS? Journal of FAS International, 1, e4. Available at
http://www.motherisk.org/JFAS/detail.php?id=29 - Sampson, P.D., Bookstein, F.L. et al. (1994). Prenatal alcohol
exposure, birthweight,
and measures of child size from birth to age 14 years. American Journal of Public
Health, 84(9), 1421-1428. - Sarkar, M. (2003). What do obstetric textbooks teach about
alcohol in pregnancy?
Journal of FAS International, 1, e8. Available at
http://www.motherisk.org/JFAS/news.php?id=20 - Sood, B., Delaney-Black, V. et al. (2001). Prenatal alcohol
exposure and childhood
behavior at age 6 to 7 years: I. Dose-response effect. Pediatrics, 108(2), E34. - Statistics Canada. (1995). National Longitudinal Survey of
Children and Youth,
1994-1995. Ottawa: Statistics Canada. - Statistics Canada. (1999). National Longitudinal Survey of
Children and Youth,
1998-1999. Ottawa: Statistics Canada. - Streissguth, A.P., Aase, J.M., Clarren, S.K., Randels, S.P.,
LaDue, R.A., & Smith, D.W.
(1991). Fetal alcohol syndrome in adolescents and adults. Journal of the American
Medical Association, 265(15), 1961-1967. - Streissguth, A., Barr, H.M. et al. (1997). Primary and
secondary disabilities in
fetal alcohol syndrome. In: The challenge of fetal alcohol syndrome: Overcoming
secondary disabilities, A.P. Streissguth & J. Kanter (eds.,), pp. 25-39. Seattle:
University of Washington Press. - Streissguth, A.P. (1997). Fetal alcohol syndrome: A guide
for families and
communities. Baltimore: Paul H. Brookes Publishing. - Streissguth, A.P., & Kanter, J. (1997). Understanding
the occurrence of secondary
disabilities in clients with fetal alcohol syndrome (FAS) and fetal alcohol effects (FAE).
Seattle: University of Washington School of Medicine. - Streissguth, A.P., Bookstein, F.L., Barr, H.M., Sampson, P.D.,
O'Malley, K., & Young,
J.K. (2004). Risk factors for adverse life outcomes in fetal alcohol syndrome and fetal
alcohol effects. Journal of Developmental and Behavioral Pediatrics, 25(4), 228-238. - Stade, B. (2003). The burden of prenatal exposure to alcohol:
Measurement of quality of
life and costs. Doctoral dissertation, University of Toronto. Presentation at 4th Annual
FACE Research Roundtable. Available at http://www.motherisk.org/JFAS/detail.php?id=40 - Square, D. (1997). Fetal alcohol syndrome epidemic on Manitoba
reserve.
Canadian Medical Association Journal, 157(1), 59-60. - The Health Communication Unit. (1999). Overview of Health
Communication
Campaigns. Available at
http://www.thcu.ca/infoandresources/general_communication.htm#tp - Tough, S., Clarke, M., Hicks, M., & Clarren, S. (2005).
Attitudes and approaches of
Canadian providers to preconception counselling and the prevention of fetal alcohol
spectrum disorders. Journal of FAS International, 3, e3. Available at
http://www.motherisk.org/JFAS/ - Turpel-Lafond, M.E. (2004). Fetal alcohol spectrum disorder:
The perspective of a
First Nations judge. Under trials - Justice issues facing Aboriginal children and youth.
Special report of the Ontario Federation of Indian Friendship Centres. - University of British Columbia. (2005). Fetal alcohol spectrum
disorder. Equality of
access: Rights and the right thing to do. Victoria, B.C.: Author. - Ungar, W., & Coyte, P. (2001). Prospective study of the
patient-level cost of asthma
care in children. Pediatric Pulmonary, 32, 101-108.