Common menu bar links
Institutional links
Diseases & Conditions
Health & Safety
Research & Statistics
Agency Information
Search Box
E-mail this page
Tuberculosis in Canadian-born Aboriginal Peoples
Special Report of the Canadian Tuberculosis Committee
Background

TB disease rates have fallen dramatically in Canada and other developed countries since the beginning of the 20th century. This significant reduction of morbidity and mortality has been accomplished through a combination of improved living standards, public health interventions, and effective drug treatment. However, Canadian-born Aboriginal peoples continue to have a disproportionate burden of TB disease.
The incidence of TB in the Aboriginal population has been shown to vary inversely with the time interval of contact with the European settlers, higher incidence rates occurring in those areas last exposed1,2.
The purpose of this report is to highlight the current trends in the epidemiology of TB disease in Aboriginal peoples across Canada.
Methodology
TB disease case data reported to the Canadian Tuberculosis Reporting System (CTBRS) from 1991-1999 were examined. The reporting system is designed to capture information on every new active or relapsed case of TB diagnosed in Canada from all provinces and territories. Cases within the CTBRS meet the Canadian Tuberculosis Standards case definition3. The case report collects information on selected demographic characteristics including ethnic origin. Ethnic origin for this report is defined as Status Indian, Non-status Indian/Metis, Inuit, Canadian-born non-Aboriginal and foreign-born. If ethnic origin was reported as unknown, the case was excluded from analysis.
Annual population estimates by origin, including estimates for specific age and sex groups, were obtained from the Demography Division of Statistics Canada (adjusted 1996 census data) and Indian and Northern Affairs Canada. Age-standardized rates (direct method) were calculated using 1996 Canadian Census data as the population denominator.
Overall Results
From 1991-1999 17,590 new active and relapsed TB cases were reported to the CTBRS. Of these, 3,013 (17%) occurred among Canadian-born Aboriginals (Aboriginals). Of the remaining cases, 4,201 (24%) occurred in Canadian-born non-Aboriginals (non-Aboriginals) and 10,281 (58%) occurred in foreign-born individuals. Reports on 95 cases lacked information on ethnic origin and were excluded from analysis. While the number of TB cases among Aboriginals decreased from 339 in 1991 to 315 cases in 1999, the proportion of TB cases that occurred in Aboriginals was relatively unchanged, from 17% to 16% (Figure 1). Age standardized rates revealed a four-fold rate of disease as compared with the national rate and as much as 20 times the rate of non-Aboriginals (Figure 2).
1999 Results
A total of 1,807 cases were reported to the CTBRS in 1999. Of these, 315 were diagnosed in Aboriginals. An additional 324 cases were reported among non-Aboriginals, and 1,152 cases were reported in the foreign-born population. Cases for which ethnic origin was unknown (16 cases) were excluded from analysis.
Geographic Distribution
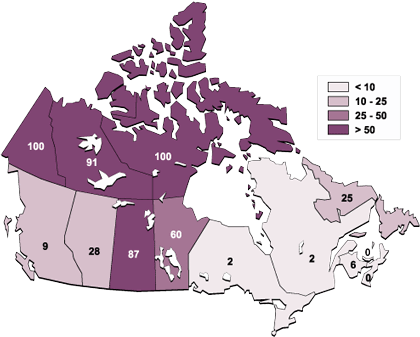
Within individual provinces and territories, TB incidence continues to show previously described patterns of higher rates in areas last exposed to European settlers. Rates were highest in the prairie provinces and the north. The territories of Nunavut and the Yukon reported 100% of cases among Aboriginals. In the Northwest Territories, Aboriginal TB represented 91% of reported cases. In Saskatchewan, Manitoba and Alberta, TB in Aboriginals accounted for 87%, 60% and 28% respectively (Figure 3).
Figure 1
Reported cases by origin in Canada, 1991-1999
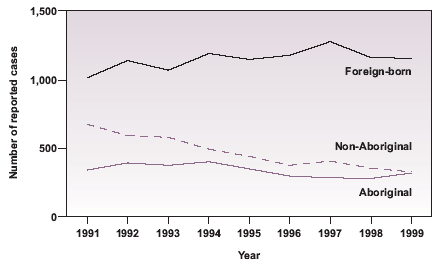
Figure 2
Age-standardized rate of TB incidence in Canada by origin,
1991-1999
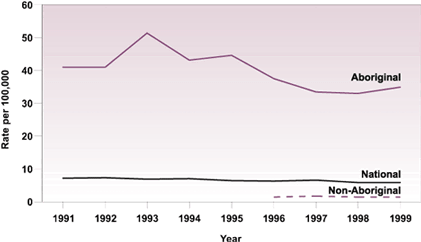
Figure 3
Proportion of reported TB cases in Aboriginal peoples in each
province/territory, 1999
Demographic Characteristics
The demographic characteristics of TB differ greatly between the Aboriginal and non-Aboriginal populations: 30% of cases in Aboriginals were in individuals less than 15 years as compared with only 9% in non-Aboriginals and less than 2% in foreign-born individuals. People more than 75 years of age accounted for only 7% of Aboriginal TB, whereas this demographic represented 20% of all TB reported in non-Aboriginals (Figure 4). Subsequently Aboriginals with TB were younger (median 27 years) than foreign-born (median 39 years) and non-Aboriginals (median 59 years). Males accounted for a majority of reported cases for all ethnic origins (Aboriginal 57%, non-Aboriginal 61%, foreign-born 52%).
Clinical Presentation
In Aboriginals, 92% of TB cases were new active cases, and relapsed cases made up the remainder. Fifty-six percent (175 cases) of the total cases were respiratory, and 30% (95 cases) were of primary origin. The Aboriginal presentation of TB is in contrast to that in non-Aboriginal and foreign-born individuals. In non-Aboriginals, respiratory TB accounted for 73% of reported cases and primary TB for only 8%. In foreign-born individuals, 65% of reported TB was respiratory.
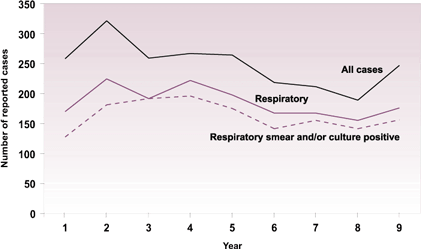
The proportion of Aboriginal TB cases that were respiratory and smear and/or culture positive has remained relatively constant over time (Figure 5). From 1991-1999 an average of 86% of respiratory cases were smear and/or culture positive. This proportion was similar to that seen in non-Aboriginals (88%).
Figure 4
Number of reported TB cases by origin and age group Canada,
1999
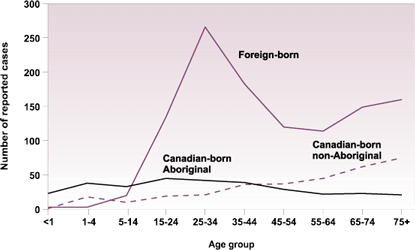
Figure 5
Respiratory smear and/or culture positive cases in Aboriginals
Drug Resistance and HIV Co-infection
Drug resistant strains of TB have not yet emerged as a significant problem in this population. Less than 2% of reported cases were resistant to one or more drugs. The extent of HIV co-infection could not be estimated using data from this surveillance system. HIV status is known for only 2% of reported Aboriginal cases.
Discussion
This report presents a current profile of TB disease in Aboriginal people in Canada. The characteristics that contrast most strikingly with other population subgroups are the stable proportion of disease in this population, the substantially higher case rates of disease and the high incidence of primary disease.
TB rates are highest among Aboriginal people in the North and lowest in the East. The current presentation of TB is consistent with the prevailing theory of disease presentation related to time of first contact with European settlers.
Although drug-resistant TB and HIV co-infection have not yet emerged as a concern, they remain potential threats. Difficulties in the delivery of drug therapy as well as marginalization and high risk behaviours may contribute to the development of these risks.
While the overall incidence of TB has been decreasing steadily over the past several decades, Aboriginal people still have a rate almost four times higher than the Canada-wide rate. Several authorities have presented reasons for this continued burden of illness in the Aboriginal population, including the existing large reservoir of infection in Aboriginal communities, difficulties in providing health services in remote areas, and poor socioeconomic conditions.
The Canadian Tuberculosis Committee (CTC) has established a goal of TB elimination in Canada. This goal will be particularly challenging in the Aboriginal population. However, through systematic and coordinated efforts addressing the improvement of social conditions, availability of adequate resources, and application of sound clinical management, the goal of TB elimination is entirely achievable. Reducing and controlling TB in this population will be dependent on early detection of cases followed by prompt and complete treatment in conjunction with a comprehensive, preferably centralized surveillance and prevention program.
The Canadian Tuberculosis Committee
Dr. Maureen Baikie, Department of Health, Halifax, Nova Scotia
Dr. Christofer Balram, Department of Health & Community Services Fredericton, New Brunswick
Ms. Patricia Bleackley, Yukon Communicable Disease Control, Whitehorse, Yukon
Ms. Cheryl Case, Government of the Northwest Territories, Yellowknife, Northwest Territories
Mr. Michael Clark, TB Program Manager, First Nations and Inuit Health Branch, Health Canada
Dr. Kevin Elwood, BC Centre for Disease Control Society, Vancouver, British Columbia
Dr. Brian Graham, Canadian Lung Association, Saskatoon, Saskatchewan
Dr. Brian Gushulak, Citizenship and Immigration Canada, Ottawa, Ontario
Dr. Earl Hershfield, Respiratory Hospital, Winnipeg, Manitoba
Dr. Vernon Hoeppner, Royal University Hospital, Saskatoon, Saskatchewan
Dr. Amin Kabani, Health Sciences Centre, Health Canada, Winnipeg, Manitoba
Dr. Barbara H. Kawa, Public Health Branch, Ontario Ministry of Health and Long-Term Care, Toronto, Ontario
Dr. Richard Long, Alberta Health, Edmonton, Alberta
Ms. Melissa Phypers, TB Prevention and Control, Health Canada, Ottawa, Ontario
Dr. Ann Roberts, Department of Health and Social Services, Iqaluit, Nunavut
Dr. Faith Stratton, Department of Health and Community Services, St. John's, Newfoundland
Ms. Nancy Sutton, Correctional Service Canada, Ottawa, Ontario
Dr. Lamont Sweet, Department of Health and Social Services, Charlottetown, Prince Edward Island
Dr. Terry Nan Tannenbaum, Quebec Ministry of Health and Social Services, Montréal, Québec
Dr. Peter Tilley, Provincial Laboratory for Public Health, Calgary, Alberta
Reference List
1. Enarson DA. Tuberculosis in Aboriginals in Canada. Int J Tuberc Lung Dis 2001;2:S16-S22.
2. Waldram JB, Herring DA, Young TK. Contact with Europeans and infectious diseases. Aboriginal Health in Canada. Toronto: University of Toronto Press Incorporated, 1995: 43-64.
3. Canadian Tuberculosis Standards, 5th edition. Ottawa: Canadian Lung Association, Government of Canada, 2000.
For more information, please contact:
TB Prevention and Control
Centre for Infectious Disease Prevention and Control
Health Canada
Tunney's Pasture, Postal Locator 0900B1
Ottawa, Ontario K1A 0L2
Tel: (613) 941-0238
Fax: (613) 946-3902
Aussi disponible en français
