Common menu bar links
Institutional links
Diseases & Conditions
Health & Safety
Research & Statistics
Agency Information
Search Box
Epi-Update
Hepatitis C Virus Infection in Canadian Street Youth (1999 – 2005)
At a Glance
- The prevalence of HCV infection among street-involved youth is high: for the 1999-2005 study period, the overall prevalence was 4.4% (vs. 0.01% reported rate among the general youth population).
- Street-involved youth with HCV infection were more likely to:
- be older, Canadian-born, and Aboriginal
- have a history of interaction with social services agencies, the justice system, and report a history of sexual abuse
- report that their primary source of recent income was from illicit activities (stealing, sex trade, dealing drugs)
- have been exposed to other bloodborne or sexually transmitted pathogens, including HIV and hepatitis B
- report high-risk sexual behaviour in their lifetimes, and to perceive themselves at high risk for sexually transmitted and bloodborne infections
Introduction
Enhanced Surveillance of Canadian Street Youth (E-SYS) is a multi-centre sentinel surveillance system that monitors rates of sexually transmitted and bloodborne infections, risk behaviours, and health determinants in the Canadian street youth population.
Street-involved youth, and youth who become homeless, even temporarily, are young people who are often marginalized in the education system and deal with unstable living conditions. Homeless and street-involved youth experience more mental health problems, exposure to violence, and higher mortality than their peers1. These circumstances, along with sexual and drug use behaviours, place them at increased risk for contracting and transmitting both blood-borne infections (BBIs) and sexually transmitted infections (STIs)2 .
Studies among Canadian street youth have estimated the prevalence of Hepatitis C virus (HCV) infection to range between 4% and 17%3 . Most people infected with HCV do not show any symptoms in the early stages, but 70-80% of those infected with the virus will develop chronic hepatitis4, and up to 25% of those will progress to serious liver disease, including liver cancer, during the following 20 to 30 years5. Currently, there is no vaccine for HCV.
In Canada, the most important risk factor for HCV infection is sharing of drug injection equipment. Factors associated with HCV infection in street youth reported in the literature include injecting drug use, being over age 18, and using crack cocaine3. Almost half of the Montreal street youth recruited in an ongoing cohort study reported ever having used drugs by injection2, as did a similar proportion in a prospective cohort study among Vancouver street youth7.
The purpose of this report is to examine the risk factors for HCV infection among Canadian street youth. Information presented is based on data collected from 1999 to 2005 by the Enhanced Surveillance of Canadian Street Youth program. There were 6053 street youth recruited from 1999 to 2005 from seven sites (Vancouver, Edmonton, Saskatoon, Winnipeg, Toronto, Ottawa and Halifax); results are generalizable to street youth from these urban centres. Not all sites participated in all years. For more information about the Enhanced Surveillance of Canadian Street Youth project, see http://www.phac-aspc.gc.ca/sti-its-surv-epi/youth-jeunes-eng.php.
Unless otherwise stated, the analyses presented below are restricted to those street youth who consented to provide blood for hepatitis C testing and who had definitive HCV results (n = 4334).
Results
HCV Infection in Street Youth: The prevalence of HCV infection among street youth is high; for the 1999-2005 study period, the overall prevalence was 4.4%.
Figure 1: Prevalence of HCV infection among street youth
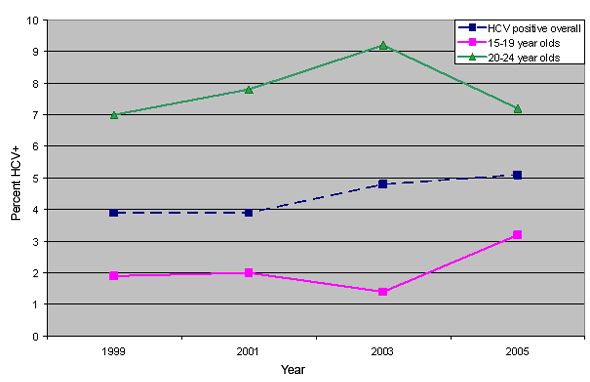
HCV demographics: Street youth with HCV were more likely to be older, Canadian-born, and Aboriginal, and were slightly more likely to be male. Youth who had completed less schooling were also more likely to be HCV-positive.
Variable |
Total |
HCV + 1 |
OR |
p value* |
| Age | ||||
| 15-19 | 2547 | 52 (2.0%) | Ref | |
20-24 |
1787 |
140 (7.8%) |
4.1 (2.9, 5.6) |
<0.001 |
| Gender | ||||
| Female | 1695 | 92 (3.8%) | Ref | |
Male |
2638 |
100 (5.4%) |
1.5 (1.1, 1.9) |
0.011 |
| Ethnicity | ||||
| Aboriginal | 1522 | 113 (7.4%) | 2.8 (2.1, 3.7) | <0.001 |
Other |
2811 |
79 (2.8%) |
Ref |
|
| Birthplace | ||||
| Canada | 3959 | 186 (4.7%) | 2.9 (1.3, 6.8) | 0.006 |
Other |
371 |
6 (1.6%) |
Ref |
|
| Highest level of education (excludes missing) | ||||
| Primary | 120 | 14 (11.7%) | 3.1 (1.7, 5.4) | <0.001 |
Secondary + |
3977 |
165 (4.1%) |
Ref |
|
1 Among those HCV +, 6.8% were HIV+; Among those who were HCV-, 0.5% were HIV+
Interaction with social and correctional services/family: Street youth with HCV were more likely to have a history of interaction with social services agencies and the justice system. They were also more likely to report a history of sexual abuse, but there was no difference in HCV prevalence between youth who were recently in contact with or living with a parent and those who were not. Many of the youth recruited in this surveillance system may be temporarily “homeless” or living on the street, but not completely without parental contact.
Variable |
Total |
HCV + |
OR |
p value* |
| Ever been in foster care | ||||
| No | 2599 | 75 (2.9%) | Ref | |
Yes |
1735 |
117 (6.7%) |
2.4 (1.8, 3.3) |
<0.001 |
| Ever had a social worker | ||||
| No | 1317 | 34 (2.6%) | Ref | |
Yes |
3012 |
158 (5.2%) |
2.1 (1.4, 3.0) |
<0.001 |
| Ever been in a group home | ||||
| No | 2413 | 75 (3.1%) | Ref | |
Yes |
1921 |
117 (6.1%) |
2.0 (1.5, 2.7) |
<0.001 |
| Ever been in jail / detention facility | ||||
| No | 1769 | 28 (1.6%) | Ref | |
Yes (overnight or longer) |
2547 |
163 (6.4%) |
4.3 (2.8, 6.4) |
<0.001 |
| Ever had a probation officer | ||||
| No | 2033 | 40 (2.0%) | Ref | |
Yes |
2298 |
151 (6.6%) |
3.5 (2.5, 5.0) |
<0.001 |
| Currently living with parent | ||||
| No | 3703 | 165 (4.5%) | 0.7 (0.4, 1.1) | 0.099 |
Yes |
546 |
16 (2.9%) |
Ref |
|
| Contact with parent / caregiver past 3 months | ||||
| No | 640 | 36 (5.6%) | 0.7 (0.5, 1.1) | 0.095 |
Yes |
3584 |
149 (4.2%) |
Ref |
|
| Left home because of sexual abuse | ||||
| No | 1718 | 70 (4.1%) | Ref | |
Yes |
255 |
20 (7.8%) |
2.0 (1.2, 3.4) |
0.007 |
Sources of income: Street youth who reported that their primary source of recent income was from illicit activities were significantly more likely to test positive for HCV.
Variable |
Total |
HCV + |
OR |
p value* |
|
| Primary income illicit source past 3 mos (sex trade, stealing, dealing) | |||||
| No | 3778 | 128 (3.4) | Ref | ||
Yes |
556 |
64 (11.5%) |
3.7 (2.7, 5.1) |
<0.001 |
|
Prevalence of sexually transmitted and bloodborne infections: Street youth with HCV were significantly more likely to have been exposed to other bloodborne or sexually transmitted pathogens, including hepatitis B. Although the prevalence of HIV among those who consented to testing was relatively low (0.8%), there is an extremely high risk of being co-infected with HIV among those with HCV infection.
Variable |
Total |
HCV + |
OR |
p value |
| HSV-1* | ||||
| Yes | 1836 | 113 (6.2%) | 2.7 (1.8, 4.0) | <0.001 |
No |
1297 |
31 (2.4%) |
Ref |
|
| HSV-2* | ||||
| Yes | 502 | 64 (12.7%) | 4.7 (3.3, 6.7) | <0.001 |
No |
2634 |
79 (3.0%) |
Ref |
|
| Hepatitis B core antibody* | ||||
| Yes (reactive) | 101 | 17 (16.8%) | 4.7 (2.8, 8.2) | <0.001 |
No (non-reactive) |
3860 |
157 (4.1%) |
Ref |
|
| HIV* | ||||
| Yes | 33 | 13 (39.4%) | 15.3 (7.5, 31.3) | <0.001 |
No |
4220 |
172 (4.1%) |
Ref |
|
| Ever told they had an STI | ||||
| Yes | 1054 | 122 (11.6%) | 6.0 (4.4, 8.1) | <0.001 |
No |
3273 |
70 (2.1%) |
Ref |
|
* Statistically significant at p<0.05; OR (95% CI) = odds ratio (95% confidence interval)
Sexual behaviour: Street youth with HCV infection were more likely to report high-risk sexual behaviour in their lifetimes, and to perceive themselves at high risk for sexually transmitted and bloodborne infections.
Variable |
Total |
HCV + |
OR |
p value |
| Ever same sex partner* (Males only, n = 2496) | ||||
| Yes | 360 | 26 (7.2%) | 2.2 (1.4, 3.5) | 0.001 |
No |
2136 |
73 (3.4%) |
Ref |
|
| Ever trade sex* | ||||
| Yes | 874 | 98 (11.2%) | 4.4 (3.3, 5.9) | <0.001 |
No |
3298 |
92 (2.8%) |
Ref |
|
| Self-perceived risk of getting an STI, HIV or HBV* | ||||
| High | 372 | 40 (10.8%) | 3.0 (2.1, 4.4) | <0.001 |
None to medium |
3767 |
144 (3.8%) |
Ref |
|
Drug use: Street youth with HCV infection were more likely to have used drugs by injection and other means, and to report recent daily drinking. Approximately 18% of street youth from 1999 to 2005 reported that they had ever used drugs by injection, and this behaviour is the single strongest predictor of HCV positivity in univariate analysis. Among the respondents who had used drugs by injection and answered the question about sharing needles or equipment, about 30% indicated that they did not always use clean, new needles or gear to inject drugs.
Variable |
Total |
HCV + |
OR |
p value* |
| Non-injection drug use ever | ||||
| Yes | 4083 | 191 (4.7%) | 12.2 (1.7, 87.6) | 0.001 |
No |
250 |
1 (0.4%) |
Ref |
|
| Injection drug use ever | ||||
| Yes | 922 | 169 (18.3%) | 32.8 (21.1, 51.1) | <0.001 |
No |
3385 |
23 (0.7%) |
Ref |
|
| Age at first IDU (median = 16) | ||||
| Less than 16 years | 327 | 64 (19.6%) | Ref | |
16 years or older |
436 |
94 (21.6%) |
1.1 (0.8, 1.6) |
0.502 |
| Cocaine injected most past 3 months* | ||||
| Yes | 208 | 74 (35.6%) | 2.3 (1.6, 3.5) | <0.001 |
No |
312 |
60 (19.2%) |
Ref |
|
| Morphine injected most past 3 months* | ||||
| Yes | 169 | 58 (34.3%) | 1.9 (1.3, 2.8) | 0.002 |
No |
351 |
76 (21.7%) |
Ref |
|
| Heroin injected most past 3 months* | ||||
| Yes | 131 | 36 (27.5%) | 1.1 (0.7, 1.8) | 0.615 |
No |
388 |
98 (25.3%) |
Ref |
|
| Ritalin¹ injected most past 3 months* | ||||
| Yes | 85 | 44 (51.8%) | 4.5 (2.7, 7.5) | <0.001 |
No |
360 |
69 (19.2%) |
Ref |
|
| Always use clean needle or other injecting equipment²* | ||||
| No | 127 | 54 (42.5%) | 2.5 (1.6, 3.9) | <0.001 |
Yes |
287 |
66 (23.0%) |
Ref |
|
| Daily drinking in past 3 months | ||||
| Yes | 284 | 23 (8.1%) | 2.0 (1.3, 3.2) | 0.002 |
No |
4040 |
168 (4.2%) |
Ref |
|
1 question asked in phases 3-5 only
2 wording changes to this question between phases 2, 3 and 4
Discussion
Enhanced Surveillance of Canadian Street Youth has illustrated that street-involved youth in several Canadian urban centres have a higher prevalence of hepatitis C virus, as well as other sexually transmitted and bloodborne infections. More importantly, the issues that may cause young people to leave their family homes and come into contact with social and correctional services may lead to a life of marginalization and risk. Leaving school, relying on illicit activities to make a living, and using non-injection drugs and alcohol are not direct causes of hepatitis C infection, but suggest a clustering of risk factors that may place youth in high-risk settings. Improving health outcomes among at-risk youth necessitates intersectoral support for young people who become homeless or street-involved.
References
- Boivin J-F, Roy E, Haley N, Du Fort GG. The Health of Street Youth: A Canadian Perspective. CJPH 2005; 96 (6): 432-437.
- Roy E, Haley N, Leclerc P, Sochanski B, Boudreau J-F, Boivin J-F. Mortality in a cohort of street youth in Montreal. JAMA 2004; 292: 569-574.
- Roy e, Haley N, Leclerc P, Boivin J-F, Cédras L, Vincelette J. Risk factors for hepatitis C virus infection among street youths. CMAJ 2001; 165 (5): 557-60.
- Public Health Agency of Canada, Blood Safety Surveillance and Health Care Acquired Infections Division. Hepatitis C Fact Sheet. Accessed April 9, 2008 at http://www.phac-aspc.gc.ca/hcai-iamss/bbp-pts/hepatitis/hep_c-eng.php.
- Gully PR, Tepper ML. Hepatitis C. CMAJ 1997; 156 (10): 1427-30.
- Zou S, Tepper M, Giulivi A. Hepatitis C in Canada. CCDR 2001; 27 (S3): 13-15.
- Wood E, Stoltz J, Montaner JSG, Kerr T. Evaluating methamphetamine use and risks of injection initiation among street youth: the ARYS study. Harm Reduction Journal 2006, 3: 18.
Acknowledgements
Enhanced Canadian Street Youth Surveillance (E-SYS) is possible as a result of collaboration between the Public Health Agency of Canada and researchers, provincial and local health authorities and community based organisations from participating sites across Canada. The organisations and people associated with E-SYS can be retrieved at http://www.phac-aspc.gc.ca/sti-its-surv-epi/youth-jeunes-eng.php. Special thanks to the street-involved youth who consented to participate in E-SYS.
For more information, please contact:
Surveillance and Epidemiology Section
Community Acquired Infections Division
Centre for Communicable Disease and Infection Control
Tunney’s Pasture
Postal Locator: 0603B
Ottawa, Ontario K1A 0K9
Fax: (613) 941-9813
