

  |
|||||||||||||||||
|
|
Health-adjusted Life Expectancy at the Local Level in Ontario Abstract Health expectancy measures are becoming a common method of combining
information on mortality and health-related quality of life into one summary
population health measure. However, health expectancy measures are infrequently
measured at the local level, despite a shift toward health service planning
to that level. Using a modified Sullivan method, we calculated health-adjusted
life expectancy (HALE) for the 42 public health units in Ontario using
life tables that were derived from mortality and population data for 1988-1992
and the Health Utilities Index from the 1990 Ontario Health Survey. There
were large variations among health units in HALE at age 15 for both men
(range: 51.3-58.2 years) and women (range: 56.6-62.9 years). Generally,
rural and northern areas had the lowest HALE. Local differences in male
HALE were greater than for life expectancy (7.1 versus 6.0 years). Despite
a relatively large health survey (45,583 respondents, range: 729-1,746
per health unit), few HALE differences deviated significantly from the
Ontario mean, raising concerns about the feasibility of estimating local
health expectancy measures with adequate precision. Nevertheless, the
wider local differences and different geographic distribution of local
HALE compared with mortality measures, along with the additional benefit
of being able to model the complex interaction of mortality and morbidity,
suggest that HALE may be a useful population health measure. Introduction One of the most striking recent changes in health care delivery in Canada and other countries has been to allocate the responsibility for planning to the regional or local level.a Concurrently, there has been a growing interest in population health outcome measures, in particular summary measures that include health-related quality of life (HRQOL) and not merely mortality or disease. Health expectancy is a potentially useful measure that combines data on HRQOL with mortality data in the form of life tables; however, to date, local health expectancy measures have been infrequently reported. The main barrier to their development and dissemination is the lack of availability of life tables and local area surveys of health status with sufficient statistical power to yield significant findings. Health expectancy describes a family of indices that combine mortality (life expectancy) with different measures of health-related quality of life.1-3 In this way, health expectancy more closely reflects current definitions of health than do indicators of morbidity or mortality alone. Like other life table measures, health expectancy builds on the principles of a stationary population to model the effects of changing patterns of health.4 Among its various applications, health expectancy is one of the few population indicators, when measured over time, that can assess whether there is a reduction or expansion of morbidity. Health-adjusted life expectancy (HALE) is a particular type of health expectancy measure. It incorporates explicit weights to combine discrete health states into a single indicator of the expectation of equivalent years of good health. Other popular health expectancy measures that use dichotomous weights include disability-free life expectancy and healthy life expectancy (e.g. using self-rated health). HALE is particularly attractive to health economists since it can be appropriately compared with other health status measures, such as life expectancy or disease-specific utility measures. Also, since HALE uses polychotomous weights, it is sensitive to changes in the severity of disability within a population. For an illustration of the benefit of combining mortality and morbidity using health expectancy measures, consider the following hypothetical situation. Assume there are two communities that have identical mean HRQOL and life expectancy in 1998 (and therefore the same health expectancy). In 1999, there is a large outbreak of influenza in one community, and the frail people-those with a very low HRQOL-die. The other community is spared influenza. After the outbreak the cross-sectional HRQOL would be higher in the community with the outbreak, but the life expectancy for 1999 would be lower. Health expectancy will be lower in the outbreak community, and the difference between communities will be less than the difference between life expectancy. In this example, an acute illness has opposite effects on the community's HRQOL and life expectancy. A health expectancy measure is the most appropriate indicator to measure the population effect of the influenza outbreak. There are many other additional health indicators and planning applications that are readily available once the basic life table is created for a local planning area and combined with an HRQOL measure. These include the impact of eliminating individual diseases using expected years of life lost from simple abridged life tables or healthy years of life lost;5,6 the latter method is particularly useful for modelling the shifting burden of disease from acute to chronic conditions.4 In a similar way, it is possible to estimate the contribution of the different HRQOL domains (ambulation, pain, cognition, etc.) or socio-economic factors on HALE.7,8 Most of the existing health expectancy estimates are for nations,9 and most of the regional estimates are calculated for relatively large populations of 2-30 million10-13 (although there are exceptions14,15). Most of these analyses have estimated disability-free life expectancy or healthy life expectancy (for derivations of HALE for larger populations see the studies by Wolfson7 and others12,16). It is possible to calculate a utility-based HALE at the local level in Ontario because of the 1990 Ontario Health Survey (OHS), the first province-wide health survey to include health status attributes needed to derive the Health Utilities Index (HUI).17 This utility-based health status measure is included in the ongoing National Population Health Survey and Canadian Community Health Surveys. In order to calculate HALE, life tables for the local areas are also required. Although life tables have historically been calculated for small populations in many countries, the practice has been less common in many areas of Canada,18 at least until very recently.19 Most local planning areas can derive local life tables using established methods20 and vital statistics, if there is accurate geographic coding. This paper describes the derivation of HALE for the 42 health units in Ontario in 1990 using the Health Utilities Index17 and vital statistics mortality data.
Data Sources Data on health status were obtained from the 1990 OHS (described fully elsewhere21,22). Briefly, 61,239 subjects were selected through a stratified, multi-level cluster sampling method with the Ontario health units as the primary sampling unit. The target population included all residents living in private dwellings in Ontario. Residents of First Nations reserves and long-term care institutions, foreign service personnel and residents of remote areas were excluded. There were two stages of the survey, the first involving an interview-completed questionnaire. For this stage, one individual responded on behalf of all members of the household (response rate: 87%). The second stage consisted of a self-completed questionnaire that was given to all members of the household over the age of 12 (response rate: 77%, effective sample size 729-1,746 per health unit). The questions pertaining to the HUI attributes were contained in the self-completed questionnaire. Response rates were higher in rural areas, among women and in the older population. Mortality files from the Ontario Registrar-General/Statistics Canada for 1988-1992 were used to calculate the age- and sex-specific death rates for each health unit. In total, 358,490 Ontario residents died during the study period (range for health units: 1,980-29,671). Postcensal population estimates for 1990 by sex and age group were obtained from Statistics Canada.
The HUI is a multi-attribute health status classification system that estimates a summary value of individual health between 0 ("dead") and 1 ("perfect health") based on preference scores for different health states.23 Each respondent answers questions pertaining to eight attributes of functional health (vision, hearing, speech, mobility, emotional state, thinking and memory, dexterity, and level of pain and discomfort). Each attribute has from four to six possible responses representing a range from an unrestricted to a highly disabled state (see Appendix). The preference score for each attribute and the subsequent multi-attribute preference function were derived from an earlier (Mark II) version of the HUI that elicited responses from approximately 200 parents of school-aged children in a local municipality.17 Preference weights were estimated using standard gamble and visual analog methods.23 Mark II weights were applied to the Mark III questions included in our study using a provisional conversion scoring system.24 The most important difference between the two versions is that the Mark II version groups hearing, speech and vision into a single "sensation" attribute whereas the Mark III version treats them separately. All individual and summary HUI estimates from the 1990 OHS were weighted according to the likelihood that the respondent would be selected from the provincial population. These weights were inversely proportional to the probability of being selected for the survey. Summary weighted HUI estimates for health units were age- and sex-standardized to the 1990 population of Ontario, using the direct method.
Chiang's method20,25 was used to generate abridged life tables for each health unit by sex and 19 standard age groups (<1,1-4, 5-9,10-14 . . . 85+ years) for 1990 based on age-specific mortality rates for 1988-1992 and the 1990 mid-interval population estimates.
HALE at age 15 by sex and health unit was calculated using a modified
version of Sullivan's method.26 From the 1990 OHS, the age-
and sex-specific weighted HUI was estimated for the 42 health units by
five-year age groups, from age 15 to 85 and over. For each age group,
"life-years lived" (Lx in traditional life table
nomenclature, where x is the age interval) from the corresponding
life table was multiplied by the mean HUI estimate to create "health-adjusted
years of life lived"
To estimate 95% confidence intervals, variance for life expectancy was calculated by a method described by Chiang.25 Variance for HALE was calculated by a method described by Bebbington,27 which considers only the error of the health status measure (i.e. HUI), despite statistical error in the conditional probability of death in a life table. This assumption is reasonable since the statistical variance of HUI introduces much greater error than the probability of death, despite the small populations used in the present study. Standard errors took into consideration both design effect and sample weights. The large number of health units (42) meant that each health unit comprised a small proportion of the Ontario population, and therefore statistical significance was estimated by comparing each health unit with the Ontario mean. All analyses were performed using SAS (Statistical Analysis System) software, version 6.12.
Of the 46,583 OHS respondents aged 15 or older, 45,583 (98.3%) gave valid responses to the questions used to derive the HUI. The mean HUI for Ontario was 0.92 (males: 0.92, females: 0.91) with a range among health units of 0.89 to 0.93. The high score for mean HUI and the small difference between health units reflect the large proportion of the population in a state of "high health," especially those at younger ages. When only those in a high health state are considered (HUI > 0.95, indicating perfect health or those with perfect health but wearing corrective vision glasses or hearing aids), a larger difference was observed among health units (68% of Ontarians' HUI was greater than 0.95, health unit range: 57-75%). Figure 1 shows the mean age-specific HUI for Ontario and the 95% confidence intervals (CI) for the health unit estimates. Generally, health units with a high mean HUI in one age group had a high HUI in all age groups, an important consideration since the derivation of health expectancy combines the age-specific HUI scores with the age interval of life-years lived. The life expectancy at birth in Ontario for 1988-1992 was 74.8 (95% CI = ±0.1) years among males and 80.9 years among females; at age 15 it was 60.7 and 66.6 years (95% CI = ±0.1 years) respectively. The mean HALE among males at age 15 in Ontario for the same period was 55.2 years and among females, 59.8 years (95% CI: ±1.43). The HALE sex difference (4.6 years) was less than the sex difference seen in years of life expectancy (5.9 years). This longer period of ill health (1.3 years) reflects a lower HRQOL (as measured by the HUI) among females at all age groups over age 15, but especially those at older ages. Figure 2 shows the range of HALE across the 42 health units. Among males, the range of HALE was 51.3-58.2 years at age 15; among females, 56.6-62.9 years. The life expectancy range among males was 57.2-63.2; among females, 62.6-69.0 years. There were few health units that had a statistically significant difference in HALE (at p < 0.05) from the provincial mean (10 of 42 health units for males, 4 for females; range in 95% CI = 1.79-3.21 years) compared with life expectancy (37 of 42 for males, 33 for females; range in 95% CI = 0.23-0.93 years). HALE lost from ill health varied from 4.2 to 6.9 years among males, and from 6.0 to 8.4 years among females. HALE lost was moderately and negatively correlated with life expectancy (Pearson's unweighted correlation = -0.35). The geographic pattern for HALE for males is shown in Figure 3; the female distribution is similar and not shown. Generally, northern and rural health units had lower HALE than their urban counterparts. The urban/rural difference in HALE is more noticeable than that seen with life expectancy (data not shown). Males in the City of Toronto were the notable exception, with the lowest life expectancy and second lowest HALE. Females in the City of Toronto fared somewhat better, with both life and HALE ranking in the lowest and second lowest quintile.
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
FIGURE 1
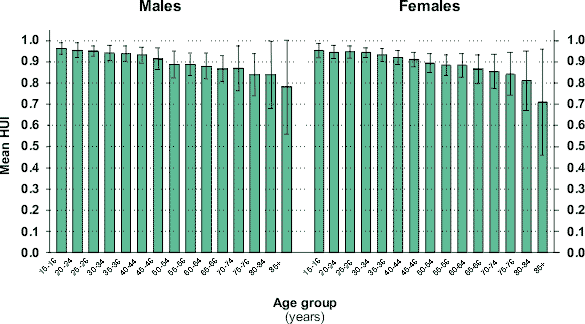 FIGURE 2 a Each point represents the life expectancy or health-adjusted life expectancy for one health unit. The horizontal bar represents the Ontario mean. HALE and life expectancy estimates that are significantly different (p < 0.05) from the Ontario mean are shaded in black. FIGURE 3 |
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
Discussion In this paper, health status at the local level in Ontario was estimated by combining mortality with a utility-based health status index. The results highlight two applications of HALE and other health expectancy measures. First, there is interest in using health expectancy as a summary population-based measure of health. Clearly, HALE measures health differently from other mortality-based indicators and, in some ways, it more closely reflects current concepts of health. Although there is a growing interest in the geographic comparison of health-related quality of life indicators, our theoretic example of the impact of an influenza outbreak demonstrates the difficulty in assessing population health status among only the survivors. This leaves us with the need to combine mortality and morbidity together in a combined indicator, of which health expectancy is increasingly becoming one of the most practical choices for developed countries.2 One advantage of a utility-based measure of health expectancy such as HALE, incorporating the HUI, is the ability to value the equivalent influences of mortality and health-related quality of life together to create a combined perspective of health. Since HALE captures a relatively broad perspective of health, even small HALE differences have important public health significance. In this light, the wide difference in HALE at the local level (7.1 years at age 15 among males, 6.3 years among females) suggests that there is a large and important disparity in health between local areas. As with mortality indicators there is a strong north/south, urban/rural gradient in health; however, the larger male difference in HALE compared with life expectancy (7.1 versus 6.0 years) indicates larger health differences than seen with mortality indicators alone. HALE at the local level indicates that the magnitude of health differences among males may be even larger than previously estimated using other indicators. Sex differences were smaller for HALE than for life expectancy (4.6 versus 5.9 years). Compared with males, women had a longer life expectancy but lived a smaller proportion of their life in a healthy state. The second application of health expectancy measures is the ability to model health effects that cannot be assessed using measures of mortality or morbidity individually. The message that male residents in northern and rural health units not only have a shorter life but also experience a smaller proportion of their life in good health is not captured by any other single population health indicator. For health modelling, health expectancy's largest potential is probably seen with further breakdown of disease, health status states and the transitions between these states in different populations and over time. For example, northern health units have a higher prevalence of acute diseases, such as childhood infectious diseases and unintentional injuries, resulting in a higher mortality at younger ages. However, there is also the concern that individuals and communities in these areas have fewer resources, and those non-fatal acute events are more likely to result in chronic disability. If this were the actual situation there would be a greater difference in local HALE compared with life expectancy, as seen in our estimates. This study does have some limitations to consider. The analysis highlights the difficulty of relying on population-based surveys to assess health expectancy at the local level. Despite the large sample and large absolute differences in HALE, there is likely insufficient power to detect statistically significant differences between many local areas in Ontario. This raises a concern regarding the benefit of estimating health status with a utility-based measure at the local level in large and costly surveys such as the OHS. One possible solution would be to have a limited number of questions on health status (not necessarily the HUI) included in the Canadian census. Questions on disability were included in the 1991 and 1996 censuses, and these could be used to estimate disability-free life expectancy. Another alternative is to first estimate the statistical power before performing analysis at the local level, and to proceed only if the power is adequate. The results presented here may be used to gauge the power for future analysis, but the estimation of life table variances is a complex problem, and no power estimation methods are currently available. Patients living in institutions were not surveyed in the OHS. Estimates would be lower if the highly disabled population in institutions were included, even though institutionalized elderly people are a small proportion of the total population.16 The effect is important when comparing the difference in HALE between men and women, since a greater proportion of women aged 65 and over are in institutions. Differences in HALE among health units would likely be slightly larger if institutionalized patients were included, since there is a strong positive correlation between the rank of HALE and the age-standardized institutionalized bed census data (data not shown). Health expectancy uniquely models complex morbidity and mortality interactions that are increasingly important for health planners and are otherwise extremely difficult to observe. Health policy directed at improving or reducing local disparities in health expectancy may be different from policies based on current indicators. Whether similar large disparities in local health expectancy exist in other areas is not known. However, local differences are seen in other health indicators, such as infant mortality and self-perceived health status, in other provinces in Canada, and they likely exist for health expectancy. Local life tables as well as health status data are required. Although the former are usually readily available, health status data are not routinely collected at this level of aggregation. The justification for collection of such expensive data is based on the need for local planning and the additional benefit over using provincial level data. Nevertheless, there are several methodologic statistical issues for local estimates that require further evaluation.
1. Adams O, Wilkins R. Development of health expectancy indicators: meeting of the International Network on Health Expectancy (REVES). Health Reports 1992;4(1):67-72. 2. Mathers C. Session III. Health expectancies: an overview and critical appraisal. In: WHO Conference on Summary Measures of Population Health [on-line]; 1999 Dec 6; Marrakech, Morocco. <www.who/whosis/smph/index.html>. 3. Mooney G. Session I. Discussion of the paper: uses of summary measures for population health by Murray, Salomon and Mathers. In: WHO Conference on Summary Measures of Population Health [on-line]; 1999 Dec 6; Marrakech, Morocco. <www.who/whosis/smph/index.html>. 4. van de Water H, van Vliet H, Boshuizen H. The impact of "substitute morbidity and mortality" on public health policy. The Netherlands: TNO Prevention and Health, 1994. 5. Nusselder WJ, van der Velden K, van Sonsbeek JL, Lenior ME, van den Bos GA. The elimination of selected chronic diseases in a population: the compression and expansion of morbidity. Am J Public Health 1996;86(2):187-94. 6. Mathers CD. Gains in health expectancy from the elimination of diseases among older people. Disabil Rehabil 1999;21(5-6):211-21. 7. Wolfson M. Health-adjusted life expectancy. Health Reports 1996;8(1):41-5. 8. Valkonen T, Sihvonen AP, Lahelma E. Health expectancy by level of education in Finland. Soc Sci Med 1997;44(6):801-8. 9. Bone M. International efforts to measure health expectancy. J Epidemiol Community Health 1992;46(6):555-8. 10. National Board of Health and Welfare. Public health report. Report no 18. Stockholm: Statistiska Centralbyran Sweden, 1997. 11. Bebbington A. Regional and social variations in disability-free life expectancy in Great Britain. In: Robine J-M, Mathers C, Bone I, Romieu I, eds. Calculation of health expectancies: harmonization, consensus achieved and future perspectives. London: John Libbey and Company Ltd., 1993:388. 12. Mathers C. Health expectancies in Australia, 1981 and 1988. Canberra: Australian Institute of Health Publications, 1991. 13. van Oyen H, Tafforeau J, Roelands M. Regional inequities in health expectancy in Belgium. Soc Sci Med 1996;43(11):1673-8. 14. Wilkins R. Health expectancy by local area in Montreal: a summary of findings. Can J Public Health 1986;77:216-22. 15. Lafontaine P, Pampalon R, Rochon M. L'espérance de vie sans incapacité en région au Québec/Regional differences in health expectancy in Quebec. In: The first REVES Workshop, International Research Network for Interpretation of Observed Values of Healthy Life Expectancy. Ottawa, 1992. 16. Berthelot J-M, Roberge R, Wolfson M. The calculation of health-adjusted life expectancy for a Canadian province using a multi-attribute utility function: a first attempt. In: Robine J-M, Mathers C, Bone I, Romieu I, editors. Calculation of health expectancies: harmonization, consensus achieved and future perspectives. London: John Libbey and Company Ltd., 1993:388. 17. Torrance G, Furlong W, Feeny D, Boyle M. Multi-attribute preference functions-health utilities index. PharmacoEconomics 1995;7(6):503-20. 18. Manuel DG, Goel V, Williams JI. Life expectancy at birth at the local level in Ontario. Can J Public Health 1999;90(1):52-4. 19. Gilmore J, Wannell B. Life expectancy. Health Reports 1999;11(3):9-24. 20. Manuel DG, Goel V, Williams JI. The derivation of life expectancy at the local level. Chronic Dis Can 1998;19(2):52-6. 21. Ontario Ministry of Health. OHS 1990: user's guide. Volume 1: Documentation. Toronto: Queen's Press, 1992. 22. Ontario Ministry of Health. OHS 1990: user's guide. Volume 2: Microdata manual. Toronto: Queen's Press, 1992. 23. Feeny D, Furlong W, Boyle M, Torrance G. Multi-attribute health status classification systems. PharmacoEconomics 1995;7(6):490-502. 24. Torrance G, Furlong W, Feeny D, Boyle M. Final report to Statistics Canada of Project No 44400900187. Provisional health index for the Ontario Health Survey. Hamilton: McMaster University Centre for Health Economics and Policy Analysis, 1992. 25. Chiang CL. The life table and its applications. Malabar (Florida): Robert E Krieger Publ Co, 1984. 26. Sullivan D. A single index of mortality and morbidity. HSMHA Health Rep 1971;86(4):347-54. 27. Bebbington A. Expectation of life without disability measured from the OPCS disability surveys. In: Robine J-M, Blanchet M, Dowd J, editors. Health expectancy: first workshop of the International Health Life Expectancy Network (REVES). London: MHSO,1992:23-34.
a In the context of this work, the local areas are the 42 health units in Ontario with a population ranging from 40,600 to 739,900 and a median of 385,900; total Ontario population was 10,341,200 in 1990.
Author References Douglas G Manuel, Vivek Goel and J Ivan Williams, Department of Public Health Sciences, University of Toronto; and Institute of Clinical Evaluative Sciences, Toronto, Ontario Paul Corey, Department of Public Health Sciences, Toronto, Ontario Correspondence: Dr Douglas Manuel, Institute for Clinical Evaluative Sciences, G-119, 2075 Bayview Avenue, Toronto, Ontario M4N 3M5; Fax: (416) 480-6048; E-mail: d.manuel@utoronto.ca [Previous][Table of Contents][Next]
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Last Updated: 2002-10-11 | |||