Common menu bar links
Institutional links
Diseases & Conditions
Health & Safety
Research & Statistics
Agency Information
Search Box
E-mail this page
HIV/AIDS Epi Update - May 2004
Perinatal Transmission of HIV
Introduction
Transmission of HIV from an HIV-infected pregnant woman to her newborn child is known as either mother-to-child, perinatal or vertical HIV transmission. HIV infection of the child can occur during gestation (in utero), during delivery (when the fetus makes contact with maternal blood and mucosa in the birth canal) or after delivery, through breast milk. In this Epi Update, the status of perinatal HIV transmission in Canada and HIV testing recommendations for pregnant women are discussed.
Positive HIV Test Reports
Between 1985 and the end of June 2003, 49,657 positive HIV tests among adults have been reported to the Centre for Infectious Disease Prevention and Control (CIDPC), Health Canada, including 7,256 (15.0%) among women. Of the positive HIV test reports among adult women, 78.4% were in their prime child bearing years (15 to 39 years).1
HIV Infection among Pregnant Women
HIV prevalence studies involving pregnant women indicate a rate for Canada of about 3-4/10,000, although rates are not available for all provinces, and data for some provinces have not been updated for 10 years. Rates for selected provinces are given in Table 1.
In Ontario, a total of 105 infants (< 2 years) born between 1984 and 2001 were confirmed to be HIV- infected. Almost 56% of the HIV-positive mothers reported that their risk factor for HIV infection was being from an HIV endemic country (a country in which the predominant means of HIV transmission is heterosexual contact). Another 32% reported non-endemic heterosexual contact, and 9% reported injecting drug use.9
In Quebec, between July 1997 and June 2001, nearly 60% of the 209 HIV-infected pregnant women were born in an endemic country. Of these women, 73 (34.9%) were African and 52 (24.9%) were Haitian.10
| Table 1. HIV prevalence among pregnant women in Canada | ||
| Province | HIV prevalence/ 10,000 pregnant women |
Year |
| British Columbia | 3.4 | 19942 |
| Alberta | 3.3 | 20033 |
| Manitoba | 3.2 | 1994-19954 |
| Ontario | 3.1* | 20025 |
| Quebec | 5.2 | 19906 |
| New Brunswick | 4.1 | 1994-19967 |
| Newfoundland and Labrador | 1.5 | 1995-19968 |
| * Among the 78% of pregnant women tested for HIV | ||
Transmission of HIV from Mother to Infant
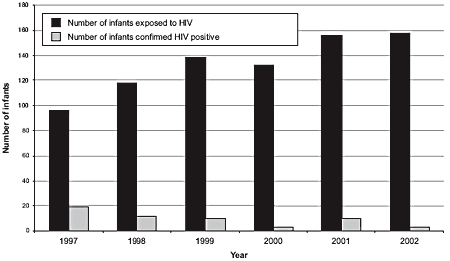
According to the Canadian Pediatric AIDS Research Group (CPARG), the annual number of perinatally HIV-exposed infants increased from about 50-70 per year in the early 1990s to 158 in 2002, as seen in Figure 1. Of the reported 1,584 infants who were exposed to HIV from their mothers between 1984 and 2002, 420 have been confirmed as infected. An additional 120 have an infection status that has not been confirmed (this includes indeterminate serostatus, died or lost to follow-up).11 The remaining 1,044 infants have been confirmed as not infected with HIV.
Figure 1. Reported number of infants exposed to HIV in utero and the number with confirmed HIV infection
Provincial/Territorial Prenatal HIV Screening Recommendations
In all Canadian provinces and territories, HIV testing of pregnant women remains the choice of the woman. Guidelines and/or recommendations for HIV testing of pregnant women have been developed in each province and territory to encourage informed decision-making; a summary of the various prenatal HIV testing approaches in Canada is given in Table 2.
A two-year chart review of pregnant women, which began eight months after universal prenatal counselling and vertical transmission guidelines were put into place in Ontario, indicated that perinatal transmission was continuing. As a result, the study authors concluded that existing guidelines were not being fully adopted and suggested that, to further decrease perinatal transmission, Ontario should include HIV testing as a routine prenatal test, ensuring that women are advised that they may refuse testing.12
| Table 2. Prenatal HIV testing approaches across Canada and year of implementation/recommendation* | ||
| Province/territory | Testing approach | Year |
| British Columbia | HIV testing is offered as part of routine prenatal care with informed consent and pre- and post-test counselling. | 1994 |
| Yukon | HIV testing of pregnant women is strongly recommended and testing of sex partner is also encouraged. | 1994 |
| Northwest Territories | Prenatal HIV testing was introduced in 1993 as an opt-in program, and in 1998 became integrated with routine prenatal care, although women have the opportunity to opt out and decline testing. | 1993, revised 1998 |
| Nunavut** | Same policy as Northwest Territories | 1999 |
| Alberta | HIV screening is part of routine prenatal blood tests for all women in Alberta, and HIV testing is done unless the woman declines to be tested (opt-out policy). | 1998 |
| Saskatchewan | Consent is obtained before any testing is done and appropriate pre- and post-test counselling are provided. | 1999 |
| Manitoba | HIV testing is offered to all pregnant women as part of routine prenatal care; the decision to be tested is voluntary and based on informed choice. | 2002 |
| Ontario | All pregnant women are offered an HIV test as part of prenatal care, with informed consent and appropriate pre-and post-test counselling. | 1998 |
| Quebec | All pregnant women and women contemplating pregnancy are offered an HIV test. | 1997 |
| New Brunswick | Physicians are to routinely encourage all pregnant women to be tested for HIV with appropriate pre- and post-test counselling and informed consent. | 1999 |
| Nova Scotia | HIV testing is offered to all pregnant women with the other prenatal tests in the first trimester. Women who decline testing in the first trimester or who are known to engage in high-risk activities are to be offered testing again during the latter stages of pregnancy. | 1998 |
| Prince Edward Island | HIV testing is recommended for all pregnant women and is offered at the first prenatal visit. | 1999 |
| Newfoundland and Labrador | HIV testing is part of routine prenatal screening and is done unless the woman declines. | 1997 |
*As supplied by provincial/territorial HIV/AIDS data coordinators, January 2003. **Nunavut became a new territory in April 1999 after separating from the Northwest Territories. |
||
Canadian Women Can Access Prenatal HIV Screening Programs
Data from prenatal HIV screening programs can provide important information on the effectiveness of prenatal HIV screening recommendations. Data from several provinces are provided below:
- British Columbia: About 55% of pregnant women in British Columbia were tested for HIV in 1995. This percentage was estimated to be up to 80% in 1999, 60% through routine prenatal testing and 20% through groups identified as at high risk (Dr. M. Rekart: personal communication, March 2002).
- Alberta: In the first four months (September to December 1998) of their opt-out policy, 4.7% of the pregnant women who were eligible for prenatal HIV testing declined this option. In 1999, 3.3% pregnant women seen at this hospital in 2002, 33 were given a diagnosis of HIV before pregnancy and 20 during pregnancy.14
- Newfoundland and Labrador: Since the 1997 implementation of Newfoundland and Labrador's policy of testing pregnant women unless the woman declines, 94% of all pregnant women have been tested. There have been no cases of perinatal transmission since 1994.15
Antiretroviral Treatment Can Reduce the Likelihood of Transmission of HIV from Mother to Infant during Pregnancy
HIV testing during pregnancy can provide the opportunity to offer antiretroviral treatment to the mother and infant as, for example, in the following:
- A full AZT (zidovudine) protocol, which includes administering AZT to the mother during the second or third trimester, during labour and delivery, and after delivery to the infant for 6 weeks, can reduce the likelihood of transmission of HIV from mother to newborn by about 65%.16
- Clinical trials in developing countries have shown that short course AZT regimens (given to pregnant women starting at 36 weeks' gestation and during labour) can reduce vertical transmission rates by about 50%.17
- Studies indicate that even greater reductions can be achieved using single-dose nevirapine.18
Data from the national surveillance program of pediatric centres and HIV clinics in Canada (where 95% of infants exposed to mothers with diagnosed HIV are followed) indicate that the proportion of pregnant women receiving antiretroviral therapy has increased steadily in the last 10 years, from 19% in 1992 to 56% in 1996, 84% in 2000 and 90% in 2002.11 The HIV infection rate of declined, and in 2000 1.7% declined.
Therefore, there has been a steady decrease in the number of pregnant women who declined HIV testing.3
- Ontario: HIV testing of pregnant women gradually increased from 40% in 1999 to 83% during the first three-quarters of 2003 (77% during the pregnancy and 6% previously).13
- Quebec: A recent study examined changes in medical practice regarding prenatal HIV testing in Ste-Justine Hospital, the referral centre for the province of Quebec, after the 1997 implementation of the HIV-screening strategy during pregnancy. The program consists of universal counselling and offers HIV testing to all pregnant women. The study found that the percentage of HIV tests offered to pregnant women was 61.8% in 2001.10 Of the 58 HIV-positive perinatally HIV-exposed infants has decreased significantly over time in Canada because of antiretroviral therapy, from 33% during 1994-95 to 2.6% in 2000.11
In Quebec, at Sainte-Justine Pediatric Hospital, the use of AZT reduced the likelihood of mother-to-infant HIV transmission from 28.3% transmission among mother-infant pairs who had not received any AZT to 3.8% among mother-infant pairs who had received partial or full AZT therapy.19
A study done from 1993 to 1999 on AZT use in British Columbia found a reduction in the HIV vertical transmission rate, from 28% in untreated women-infant pairs to 13% in partially treated pairs and 0% in completely treated pairs.20
In Alberta, a study examining the prevention of perinatal HIV transmission from 1998 to 1999 found that when HIV-positive mothers were treated with antiretrovirals during pregnancy and the intrapartum period, 31 of 36 babies (86%) were not HIV-infected.21
Canadian Prenatal HIV Screening Programs Are Valuable
Screening pregnant women for HIV clearly represents an important opportunity to prevent the transmission of HIV to infants through perinatal transmission. It is estimated that if such programs screened 90% of pregnant women across Canada, there would be a 65% reduction in the number of HIV-infected infants (compared with no prenatal testing and assuming 24% of untreated pregnancies and 6% of treated pregnancies result in HIV-infected infants).22
Comment
CIDPC has estimated that about 17,000 Canadians are HIV-infected but unaware of their infection.23 The proportion of positive HIV test reports in Canada attributed to women is on the rise. As a result, as more women become infected with HIV, the risk of perinatal transmission will increase. Given
this and the fact that perinatal infections are preventable, it is important that all pregnant women, and women considering pregnancy, should have access to prenatal care that includes the offer of HIV testing as well as appropriate counselling and care.
References
- Health Canada.
HIV and AIDS in Canada: Surveillance Report to June 30, 2003. Surveillance and Risk Assessment Division, Epidemiology and Surveillance, Centre for Infectious Disease Prevention and Control, Public Health Agency of Canada, November 2003. - Pi D, PJ Ballem and MT Schechter.
Final Report: the BC prenatal study: 1989-94. Report submitted to Laboratory Centre for Disease Control, Jan 1995, and Rekart M. HIV in pregnancy. BC AIDS Update Quarterly Report: 4th Quarter 1995. - Jayaraman GC et al.
Mandatory reporting of HIV infection and opt-out prenatal screening for HIV infection: effect on testing rates. Canadian Medical Association Journal 2003; 168(6); 679-682, - Blanchard J et al.
Manitoba antenatal study. Report submitted to Laboratory Centre for Disease Control, June 1996. - Remis RS et al.
Seroprevalence study among pregnant women in Ontario: preliminary report of the serologic component. Unpublished progress report submitted to Centre for Infectious Disease Prevention and Control. - Seroprevalence of HIV-1 antibodies in women giving birth to live infants: a five-year trend analysis for selected regions outside Montreal, 1989-93. Reported submitted to Laboratory Centre for Disease Control, Nov 1994 and Hankins D, Laberge C, Lapointe N et al. HIV infections among Quebec women giving birth to live infants. Canadian Medical Association Journal 1991; 144(3):277-80.
- Getty G et al.
Seroprevalence of HIV infection in pregnant women in New Brunswick. Canadian Journal of Infectious Disease 1997; 8:24A. - Ratnam S, Sutherland D.
A follow-up to prenatal HIV seroprevalence study in Newfoundland. Final report to Laboratory Centre for Disease Control, March 1997. - Remis RS et al.
Epidemiologic modeling to evaluate prevention of mother-infant HIV transmission in Ontario J AIDS, 2003;34 (2);221-230. - Boucher M, J Samson and N Lapointe
HIV Screening Among Pregnant Women in the Province of Quebec: Success and Failure. Can J Infect Dis 2002; 13 (suppl A): 30A (abstract 223). - Health Canada.
HIV and AIDS in Canada: Surveillance Report to December 31, 2002. Division of HIV/ AIDS Epidemiology and Surveillance, Centre for Infectious Disease Prevention and Control, Public Health Agency of Canada, April 2003. - Bitnun A et al.
Failure to prevent perinatal HIV Infection. Canadian Medical Association Journal 2002; 166(7); 904-905. - Remis RS.
Tables of prenatal HIV testing in Ontario: Summary.
- Santé et Services sociaux Québec
Portrait des infections transmissibles sexuellement et par le sang (ITSS), de l'hépatiteC, de l'infection par le VIH et du sida au Québec décembre 2003 - Mossman, CL and S Ratnam
Opt-out prenatal HIV testing in Newfoundland and Labrador Canadian Medical Association Journal 2002; 167 (6);630. - Connor EM et al.
Reduction of maternal infant transmission of human immuno-deficiency virus type 1 with zidovudine treatment. Pediatric AIDS Clinical Trials Group Protocol 076 Study Group. New England Journal of Medicine 1994; 331:1173-80. - Shaffer N et al.
Short course zidovudine for perinatal HIV-1 transmission in Bangkok, Thailand: a randomized clinical trial. Lancet 1998; 353(9155):773. - Marseille E et al.
Cost effectiveness of single dose nevirapine regimen for mothers and babies to decrease vertical HIV-1 transmission in sub-Saharan Africa. Lancet 1999; 354(9181): 803-9. - Antiretroviral Therapy in Pregnant Women (CPARG):
Access and Outcome (1995-1997) and the Experience of Transmission
of HIV in Treated Pregnant Women at Ste. Justine's Clinic,
Quebec.
Presentation by Lapointe N. in the Proceedings of a Scientific Meeting to Review the Vertical transmission of HIV in Canada, June 1998. - Forbes JC et al.
Effect of antiretroviral use on HIV vertical transmission rate and injection drug use on adherence in British Columbia, Canada. Can J Infect Dis 2000; 11:46B {Abstract 246P}. - Robinson JL and EL Bonita.
Prevention of perinatal transmission of HIV infection.
Canadian Medical Association Journal 2000; 163(7):831-832. - Archibald CP et al.
Estimating the impact of antenatal HIV testing in Canada: a lesson on the difference between efficacy and effectiveness. Canadian Journal of Infectious Disease 1999; 10:43B {Abstract C304}. - Geduld J, Gatali M, Remis RS, Archibald CP.
Estimates of HIV prevalence and incidence in Canada, 2002. Canada Communicable Disease Report 2003; 29:197-206.
[Back] [Table of Contents] [Next]
